New episode: Food insecurity
What would you do if you saw a child at school stuffing toast into his backpack so his baby sister could eat, because there was no food at home? With four and a half million children in the UK living in poverty, food insecurity is a growing and deeply concerning issue. It has a profound impact on the health and wellbeing of children and young people.
This week Emma and the panel are joined by Professor Greta Defeyter to go over the effects of food insecurity on child development, the details of food deserts and food swamps, and the practical steps we can take.
Professor Greta Defeyter OBE is a Professor of Developmental Psychology at the Northumbria University and the founder and director of the Healthy Living Lab.
-
Episode 16: Food insecurity
Featuring: Professor Greta Defeyter, Dr Emma Lim and Dr Christo Tsilifis
[Music starts]
Greta: When you look at the eating habits of those people who are food insecure, they're not healthy. They can't be healthy because of the cost of food.
Emma: I don't think people realise that obesity is a disease of poverty.
Greta: And I saw a little boy putting toast into his pockets and into his backpack.
[music ends]
Emma: Welcome Greta Defeyter. I'm really excited to welcome you to The Paeds Round podcast, and it's really, really, exciting to have different people to talk to us. And I believe your work is so important that all paediatricians should know about what you do.
Greta: Well, thank you so much. I'd love to speak to paediatricians. So, thank you for this opportunity to speak to you today, Emma.
Emma: I think that many people in paediatrics, but not in the wider world, may not know who you are and what you do. So, you're a Professor of Developmental Psychology in The Department of Social Work and Education and Community Wellbeing in Northumbria University, and the founder and Director of the Healthy Living Lab. And you've been awarded all sorts of exciting medals. You're a food hero. You are a Fellow of the British Psychological Society, and I think you've just won an OBE - is that correct?
Greta: Yes, that's correct.
Emma: Tell me how did you get interested in what you're doing now? How did it all happen?
Greta: Okay, so it's a kind of strange story, in a way, because I was in the Department of Psychology at the time, and I had a PhD student looking at the effects of breakfast cereal on children's cognition. And these are very controlled experiments where we go into schools or we used to bring children into the lab, and we'd weigh out all of the food, we'd look at all the ingredients in the food, and then we'd measure children's cognition on a variety of different cognitive tests. And one day, she was conducting this research in a school, and I just happened to see a school breakfast club operating in the corner of the school hall. This was now nearly 22 years ago, so quite some time ago, where not many people knew about school breakfast clubs, and I definitely didn't know about them. And I asked the head teacher, what's going on over there. She just looked at me like I was really stupid, and said, it's a school breakfast club Greta. And I said, ‘well, why are you doing that?’ And she said, ‘well, some of our children live in poverty, and they come in to school, and they haven't had breakfast’, I said, ‘could I go across and have a look?’ Typical psychologist and a woman very nosy.
So, we went across and had a look, and I saw a little boy putting toast into his pockets and into his backpack. And I thought, that's strange behaviour. So, I asked the head teacher, obviously, for child safeguarding whether I could go and talk to the young pupil and she came across with me. I said, ‘you're not in any trouble, but can you just tell me why you're putting toast in your backpack?’ And quite matter of fact, in a matter of fact, he said to me, ‘I'm taking toast home for my baby sister, as there's no food in the house’, and it was the way he said it as a practical solution that his child had thought of to address what we now call household foods insecurity.
It's spoken about quite widely, but that was the first time I'd ever come across it. And the image of that little boy putting that toast in his backpack has stayed with me right to this day and that just overnight, I changed my whole kind of, like, course of my research, so to speak, to say, this is out there. I can see it. I've just seen it. I've seen it right. So, I started to look at what research has been done with children and young people in the UK about food insecurity, and found there was very little.
Emma: Greta, that's an amazing story, and it's such a stark reminder of what life is like for many children and young people these days. So, tell me about food insecurity and how it affects children and young people.
Greta: In the UK, we currently have about four and a half million children living in poverty. Poverty is associated with food insecurity. So, food insecurity can be through lack of access to food. So it could be, for example, for elderly people in particular, they can't get to shops, and they haven’t got access to food in their communities, but that's a small proportion of those families that we classify as being food insecure. The majority of families who are food insecure is because they live in poverty.
When you look at the eating habits of those people who are food insecure, they're not healthy. They can't be healthy because of the cost of food. So, you find that families have what we call food insecurity with hunger. And I don't mean just mean feeling a little bit peckish, I mean, feeling hungry and there's no food to eat. It's a very different understanding of it. And we also have families who are classified as low to moderate food insecurity. What you typically find in those families is that they either downgrade in terms of the quality of the product of food they are buying, the value ranges, or typically, they have diets that are high in salt, sugar, saturated fat, and often it is classified now as ultra process food.
Emma: That is shocking, shocking statistics, when you look at the millions of children and young people living in poverty today in the UK, because we are a developed world country and we have the resources, that is actually a terrible statistic. What I want to ask you is, you've described how many children don't have food at all, so they're hungry and they can't get any food, or if they can get food, the quality of the food that is available to them is poor. And as a paediatrician, access to healthy food and fruit and vegetables and milk and calcium is so important to wellbeing and growth. So, what difference does it make? What are the health outcomes for these children and young people who can't get the food they need?
Greta: The podcast won't be long enough for me to list negative outcomes, but for the first time in decades, we're seeing things such as rickets, stunted growth, dental caries, so linked to poor oral hygiene, but also to the sugar content and food. We're seeing obesity and malnutrition sit side by side. We're seeing poor mental health, and we know that actually the food you eat, in terms of being absorbed into your circulation through the blood brain barrier, the amount of glucose in the food. So, the sugar conversion in the food affects how your cognition works, so your decision making. It also affects how well the children do at school. Not enough food actually doesn't allow the neurotransmitters to work properly, and so you have deficits and working memory, sustained attention, etc. So, food and the quality of food is important for children's health and development, but it's also important for their mood, their mental health and wellbeing and their cognitive processing.
Emma: Yes, it's very stark, isn't it? And I think it's a really important point. There are two things I want to talk about. I think it's a really important point that you need a certain type of food with complex carbohydrates, with fibre, with vitamins, and there's more and more work on your microbiome showing you need a big variety, and these ultra processed, cheap foods are not supplying that. And I just want to highlight something you said about obesity and poverty, because I think there's a misconception that people who are obese are eating too much. I don't think people realise that obesity is a disease of poverty.
Greta: Correct, and it's purely the fact that people don't have enough household income to buy a healthy diet. Poverty is also related not just to what you can purchase, but to where you live. So, if you live in poverty, you're more likely to live in poor housing. If you live in poverty, you're more likely to live in an area that actually doesn't have access to healthy food. I mean, I can share with everybody. I live in Blythe in Northumberland. I live in one of the poorest towns in Northumberland. We do not have a greengrocer. We don't have a bakers, we have lots of betting shops, we have lots of charity shops. I have a kind of a discount broken biscuit store. But in terms of accessing fresh produce, local produce, it's just not available in Blythe. That's it. That's a really good example.
So, poverty determines where you live, what you have access to, and therefore, obviously it also determines your financial income, to your household. And when you start loading these factors onto one another, you can see the ill effects of poverty, but you can see actually that poverty, I always think of poverty is like a prison with no bars, because poverty affects what you have in terms of your choice. People living in poverty don't have the same choice. So, it's not an individual behaviour. It's a structural problem that we have with our society.
Emma: I think that is so true. It's really interesting. I went to Detroit, and the whole town had collapsed with the collapse of the automobile industry. And they actually had food deserts, so you couldn't get hold of any food, and the only place that you could get food was at the petrol stations, because the only thing that was available was petrol. So, if you could walk to a petrol station, you could get food, there was nothing else in between.
Greta: Yeah, and we have the same in the UK. We have what we call food deserts and food swamps, as I call them. So, food deserts is where you can't access food. Food swamps, and we've all seen it, right! It's where you have on a line Kentucky Fried Chicken, McDonald's, Burger King, Wendy's, all of them, right! And they're cheap and they're easy. If you don't have a car, and you can't get access, you can see exactly what happens. And that then becomes normative, because everybody's doing it in that community. And so, it's again, I'll say it's a structural issue that we have. And sometimes I look at what I call big food operating across areas where there is really deep poverty, and I kind of just have to sometimes shake myself to say, keep fighting the fight. Because we have to fight this. We cannot allow this to happen. It's been happening for years, and it's just not good. It's costing our health service. It's costing our education service, and more importantly, it's costing the life of children and young people.
Emma: And I think it's really important that people understand this is not a quick solution. You can't give people vegetables because, actually, they may not have a stove. They may not be able to pay the electricity bill for them to actually cook the vegetables. They may not have, not only the implements, like all the things that you need, pots and pans, but the knowledge about what to do with the vegetables, because they have lost out on their education, and they are literally just living day by day, just getting by. So, this is a complex problem. This is not a simple problem.
Greta: Correct? And I'm going to add a further thought to that, that even if you have the knowledge, even if you have access to a cooker, if you are in house of multiple occupancy, for example, even if you can afford the electricity, when you have to make food choices, when you are living in poverty and you have high food insecurity, every decision you make is riskier.
So, if, for example, you cook, I can think of my own household if I cook jacket sweet potatoes instead of a normal potato. And my family tried them and they don't like them. You know what? I can go and cook something else, when you're looking at it in the terms of the risk of trying to do that sweet potato, the risk is tenfold when you live in poverty, to somebody like myself who can afford to cook something else. And it's an important thing, because poverty then changes the decision and risk making process, so that cognitive process of how much you take a risk. Okay? And that applies to food. It applies to gambling. It applies to whether you take a loan from a loan shop. Things that don't look rational for somebody that has money are completely rational when you live in poverty.
Emma: It is a really important thing that doctors and people in the medical profession who are looking after all these children with these effects of poor diet, which we know are huge, so obesity, diabetes, hypertension, malnutrition, and you're absolutely right. We've seen rickets. We've seen diseases of the Victorian age come back, which we have not seen in years. And it's really important that doctors understand the life that their patients lead.
Greta: Correct. So, I have examples where I've been working with children and young people, and they've been discharged from hospital, and they've been given a diet sheet. I mean, I have to laugh. I can absolutely appreciate what the clinician is trying to do. But I look at it, and I look at what I know the family can afford, there's a Red Sea. There's a there's an ocean between us, right! Because it's fine saying yes, you should eat according to the Eat Well Plate as one guide, for example, around food groups and nutritional standards. But the families I work with can't afford to eat an Eat Well Plate type of diet.
So, it then undermines, in a way, what the paediatrician, for example, is trying to do. And it also means that from the recipient point of view, that then starts to have a lack of trust, because it looks like the paediatrician doesn't understand the kind of home environment in which that child or young person live or you ask parents or carers to do something that maybe they can't do. Maybe they don't have access to a cooker. Maybe they have a refrigerator, but the food is stolen from the refrigerator. It's very difficult to try and match the two.
So, we have to think about how we reach out and how we work in a kind of, what I call a linking arms type of way to make people or support people, rather in having a better diet, but being really aware of the constraints on the situation in which young people live. Somebody will come out from hospital with a diet sheet, and the person that's taking care of that child or young person will say things like, we'll have a treat and we'll stop at McDonald's on the way home. There we go. And it's become a cultural treat, if not a normative everyday situation, and so we need to work with families to change that, but we need to work on the food system as well, and we need to work on the social welfare system, and we need to work on poverty. And all these levers have to work cross sectoral in terms of programmes, isn't it!
You can't just fix one programme. People's lives aren't like that. So, it is a complex problem, but it's something that both sides, having that greater understanding for both sides of the equation will go a long way to helping and supporting children and young people.
Emma: Yeah, I think it's really interesting what you say. t's so true about the McDonald's as a treat. What are treats? And I know from my children just going to the local state school, and they tell me that they actually don't like people looking in their packed lunch, because that makes them stand out. Their packed lunch doesn't have crisps; their packed lunch doesn't have biscuits. Their packed lunch has homemade food. One of my children doesn't like sandwiches, so I'll just take rice and lentils and things that are culturally appropriate for them. But that's very unusual. And children come to my house, and they sit down and they look on the table and they say, ‘what is that’? We were originally talking so we've talked about how food poverty and food insecurity leads to poor health. But what about the effect on your schoolwork? Because we are talking about children and young people here.
Greta: Yeah. So, we know when we look at studies that have looked at cognition and schoolwork, we know it is actually not just the fact of not having food, but the type of food you eat that affects your cognition. And the main processes that are affected are sustained attention and working memory. So, if you think about it in terms of schoolwork, well, you need to pay attention and you need to have a good working memory. So those processes are affected by default. Your educational attainment is going to be affected. And the government has been quite good and quite active in the last few months around school breakfast clubs. So, in England now we have a slow roll up, a good roll out of National School Breakfast clubs. And of course, we have the extension of free school meals to an additional 622,000 pupils come next September. So, both of those are really good programmes that the UK Government has introduced to try and combat both food insecurity, dietary intake and, also educational attainment.
Emma: Greta, what happens in the holidays because there's no school?
Greta: Well, so in the in the holidays and in days when children aren't in school, so children typically in state schools are in schools for about 190 days. But there are 173 days where children are not in school. So, you know, if you want to have an intervention, you have to think of the whole child, the whole system, the whole family. And so, I was very lucky that the All Party Parliamentary Group on school food gave me permission to conduct some research on their behalf. And we mapped the holiday clubs across England. We had over 400 organisations delivering but there was no governance, no quality assurance, and we spent the next five years collecting evidence about the impact of these clubs. And in 2017 Frank Field, actually presented a bill called the School Holidays, Food and Activities Bill to Parliament, and luckily the bill passed. It was a brand-new social policy, and after a few years, we got funding. And currently the government in England funds what they call the Holiday and Activities Food Programme, which I helped co design.
Emma: Tell me what the Holiday and activity Food Programme is?
Greta: The Holiday and Activity Food Programme is a programme that's funded by the Department for Education. It's funded at 200 million pounds a year, and it goes across every higher tier local authority in England. The programme itself is designed to offer free food and enriching activities for children aged 5 to 16 who are in receipt of free school meals.
Emma: I think that's so important. I would remember a friend of mine saying to me, I had 100% attendance at school because it's the only place I knew I would eat. I never missed a day of school. And as you said, like 173 days a year there is no school. So, this is a very, very basic need for people, and young people and children to have food. We've talked so much. There are so many things I could ask you, but I want to ask you something very specific. What is your ask to paediatricians when they see children and young people in their clinics or in their emergency departments, what do you want them to think about?
Greta: I suppose what I would ask them is try and put yourself in the shoes of your patients and think about them as people that may well live in a different environment or different household to your own. And the other thing I would ask them to do is to ensure that their hospital or their practice or their clinic has contacted the local authority and knows of the actual resources that are available. So whether you look at the HAP programme, whether you look at food pantries, whether you look at Citizens Advice numbers, whether you look at schools that are running breakfast clubs be aware of what's happening in your local vicinity, so that yourself or your social prescribers can actually direct and support families into those actual areas of help.
I think one of the things that's really difficult is keeping abreast of it for clinicians, but local authorities have that information, so the social prescriber has a really good link with the right person in the local authority. It's then quite easy to keep up to date with what's happening in your local area, and to think of some of the programmes, like the holiday activity programme, not as a deficit programme, but as an asset-based programme. And it doesn't have to be big things, even small things that we often take for granted, a trip to the park, for example, well, maybe it's buying a lollipop, or maybe it's taking a picnic. Well, if you don't have money and you don't have access to food, those things now become a problem, right! Or it may be something like going and playing football, but if you can't afford the football boots, then there's a problem. So, you're not engaging in the physical activity. So when you're thinking about food insecurity, remember that's just one part of that family's life, that life is affected by, especially if you're looking at poverty multiple factors so, damp housing, poor ventilation, can't afford the heating in the winter, clothes, school uniform, meals and the content in a packed lunch. I could go on and on, but hopefully you'll see it is complicated, but having that empathy, I think, and then setting realistic goals that that family can achieve, I think, is really important.
Emma: Yeah, I think the first thing I want people to do is just ask the question in a sympathetic manner. Very recently, I've been in clinic, and I was asked to see a baby who wasn't growing very well, and I said to the mother, you know, ‘what are you feeding?’ ‘What's happening?’ And she said, ‘at the end of the month, I can't afford formula milk. I can't afford milk for my baby’. It's just, if I hadn't asked the question, I could have gone down a whole route of investigation and taking bloods when I just needed to ask a simple question in a way that she felt safe to talk about this. As a result, there are the formula milk vouchers, and also the family might be eligible for warm home benefit and understanding, as you say, knowing that this is available, knowing that people can access it, you don't have to do it yourself. You just need to sign post them to the right place.
Greta: Yeah, and talking about it in a way that's normal, so you normalise it. Families trust paediatricians and school teachers much more than they trust academics so we're further down the list. Okay, but actually thinking about it in a normal way, if you're discharging a child or young person, or you're taking care of them, then actually, surely, you know, forgive me if I'm saying something out of term here, but surely you're taking care of the whole child, and a whole child isn't just in hospital. The whole child is going to go home to an environment there's no point in treating a child to me in hospital to send them home to, like a damp home or a home that's got mould coming down the wall or home that has got no food in the cupboards or the fridge, right! Because the child is just going to end right back with you again. So, it's thinking about how we as a whole society support what I call whole children, whole people.
Emma: Absolutely, there's no point in prescribing loads and loads of asthma inhalers when actually the root of the problem is poor housing.
Greta: Correct, and likewise there's no point in giving a diet sheet if the root of the problem is food insecurity,
Emma: Absolutely, and I think that, there's lots of ways that people can do small things. So, a good example is that we've started collecting for the children's clothes bank. I collect children's clothes that have been passed down from any of the staff in our hospital and secretaries, and every single time I tell people, if you don't give those clothes, children can't go to school, they can't go out of the house. There are people who don't have shoes. Tell me what we can do to make things better.
Greta: So, I think what we have to do is, as professionals, I think we have different roles to play at different levels. So, I think advocacy and campaigning around the issue, so that central government to look at policy. I think also locally, so thinking about how we work in the northeast, with our Northeast Mayor around interventions that she's putting in around her child poverty strategy. So, both the local and the national coming together, thinking about even small things. So, for example, how hospitals could play a role in - I'm going to say it, it's probably controversial, but I'm going to say it, it will be no surprise to Emma that I'm going to say it probably. But thinking about food served in hospitals, okay, thinking about, is that food really healthy!
Emma: I couldn't agree more. I think it's important. I think it's the one place where we can not only nourish children, but we can actually give parents and families the opportunity to see what they could have. But I'm actually quite ashamed of what happens in hospitals. We have done a whole lot of work, which I know you're aware of, where we don't actually, we haven't been feeding parents who come to hospital. And we have stories where we ask the parents, what do you do? And the parents said, I wait till my child was finished, and then I eat the scraps off their plate so they can't afford to eat. Generally, the cost of coming to hospital, and the pressure that then puts on the family for unnecessary admissions is huge. So, I think it's a really important thing to think about. You know, does this child need to be here? Do they need to be admitted? Is this the best place for them? Could you deliver this care closer to home? So, you've talked about what you want paediatricians to know, how you want paediatricians to ask questions, how you want paediatricians to understand where their patients come from, but we haven't really talked about what you'd like hospitals, management and even universities and academics to do on this. I'm sure you have an opinion, Greta, because you always do.
Greta: I do have an opinion on this. Okay, so, and I'm going to give you my opinion for what it's worth, I think that we really need to review the quality of food in hospitals and universities. So, I'm going to talk about universities, but what I'm going to say, I think, will apply to hospitals. So, when I look at schools or holiday activities and food that are - what we call school food standards - that actually govern the quality, and the food groups served to children and young people. Now we know from the science that brain development occurs all the way to age 21 right! So, this is now university students are included in my zone of development. When I look at the guidance for the food served in universities, you may be surprised. It's a completely blank page. There is no policy or guidance whatsoever. Emma: None. Greta: None. When I look at hospitals, if there is guidance, they are probably breaching it. I was at a local hospital to me not long ago, and the offer at the cafeteria was chips, or double cooked chips, or a bag of crisps or a sandwich that had so many ingredients in whose name I couldn't actually pronounce, and yet, these are places of learning and health and wellbeing, in terms of getting as well,
Emma: Right! Well, there's two bits of that, the hospitals, I absolutely agree, and I think it's really interesting, because I think that we can learn from other places that do it well. So I worked as a VSO (Voluntary Service Overseas) volunteer in the South Pacific, and I was a paediatrician in a hospital in Vanuatu, and what we did is, we had a hospital garden, and anybody who was staying more than a couple of days, they would go in their spare time, because there's a lot of time when you're sitting around in a hospital where things aren't happening and the garden was right below the wall, they would go to the garden, and they would help tend the garden, and they would pick the vegetables and food in the garden, and they would cook it all together for all the children and families on the ward. And it was such a good thing. It was such a sustainable thing, and it was fun, and it was an opportunity for the nurses and the children and the staff to do something together that wasn't just about immediate, I don't know, nasty things like giving injections and taking blood. So, it was a really positive thing. And I think something like that, we should be having things like that. So, there you go. That's what I think we should have.
Greta: So, I agree with that, but I think we should go further than that as well.
Emma: All right, Greta, it's been a huge pleasure. It's a bit like Desert Island Discs. You don't have 10 choices of discs, but you do get to give us your three top tips. So, we like to end on your three top tips. What would you like to say to all the paediatricians, all the healthcare workers who are looking after children and young people?
Greta: First thing I'd like to say is, thank you for all your hard work and professionalism. You saw us through Covid. You're still doing a grand job. You have my full support. That's the first thing I'd like to say. Second thing I'd like to say is, be aware of the whole child and young person, not just when they're in clinic or in your hospital but thinking about the environment that that child is going back to. And thirdly, is, have the conversation.
Emma: There we go, just like we are. It's been a great pleasure. Greta, it's just been so fun to talk to you, and you're right. We could have done this for a couple of hours, so we've just had to cut ourselves short.
[music starts]
This podcast is produced by Odland Education. The views, thoughts and opinions expressed in this podcast relate solely to the speaker and not necessarily to their employer, organisation, the Royal College of Paediatrics and Child Health, or any other groups or individual. You can find a wealth of information on the important work of the Royal College of Paediatrics and Child Health on rcpch.ac.uk, or #choosepaediatrics.
[music ends]
About this podcast series
Listen to real-world advice and guidance on how to manage a range of clinical topics and much else on education, training and working in paediatrics. With Dr Emma Lim, Consultant Paediatrician and Dr Christo Tsilifis, Academic Paediatric Trainee, plus parents, paediatric specialists and junior doctors.
-
EPISODE 1: Neonatal herpes simplex virus disease - THANKS (Think Hands And No Kisses) (released 24 October 2023)
Though common and self-limiting in older children and adults, herpes simplex viral infection can cause a spectrum of neonatal disease from simple lesion to devastating encephalitis. How can we identify babies at risk and provide appropriate treatment?
In this episode, Sarah discusses her devastating story of losing a child to neonatal HSV and her work in raising awareness of neonatal HSV.
Featuring Emma Lim and Christo Tsilifis with Sarah de Malplaquet, parent of Kit, and founder of the Kit Tarka Foundation.
This podcast is a collaboration between the Royal College of Paediatrics and Child Health (https://www.rcpch.ac.uk) and Odland.
RCPCH The paeds round
Neonatal herpes simplex virus disease – THANKS (think hands and no kisses) Transcript of podcast – October 2023[music, with snippets]
Emma: Us not being open and talking about herpes so that we can do something about it, have all led to this awful tragedy that is part of your family history.
Sarah: Don't let anyone hold your baby without washing their hands, and, and don't let anyone other than the parents kiss your baby.
[music ends]
Emma: Let’s get down to rounds. Hello, my name is Emma Lim and I’m a consultant paediatrician at the Great North Hospital, and I would like to welcome you to The paeds round, your regular podcast from the Royal College of Paediatrics and Child Health
Emma: So Sarah, well welcome today and it's really lovely to speak to you. Would you just like to introduce yourself and tell us why you're here?
Sarah: Yep. I'm Sarah de Malplaquet. I'm the CEO and founder of Kit Tarka Foundation, which is a charity I started after the preventable death of my son Kit when he was 13 days old. Um, and he died from neonatal herpes.
Emma: First of all, Sarah, I just want to thank you for coming because to do what you did to start a foundation and to continually talk about what must be one of the most distracting things to ever happen to a mother is, is just so hard. If we go about how many years ago was this now?
Sarah: So he died in September, 2017, so he should be five now.
Emma: And how did you feel when you were pregnant with your first child?
Sarah: Um, absolutely over the moon. So we were really lucky. Um, and yeah, the pregnancy was pretty smooth. I mean, the usual like aches and pains and heartburn, but absolutely no concerns throughout the whole pregnancy until the very end.
Emma: And when was it that you had some inkling that things weren't quite right?
Sarah: when I was around 39 weeks, I actually got a rash on my fingers. Um, And this was actually a red herring that because I had a rash, I was taken into hospital and tested for, um, icp, cuz it was like an itchy rash. It actually turned out to be pom, it's, it called conflicts the, um, eczema. So that was a complete red herring. But because I was in hospital and my blood pressure was checked as a matter of course, and it was found to be high. Um, and that's when kind of alarm bells ring for the doctors. I mean, I'm absolutely convinced it was the white coat syndrome and However, once I was on that kind of intervention train, um, Because it was so close to the end of my pregnancy, I was kept in hospital and an induction was recommended.
Emma: So you'd had this wonderful pregnancy. It was your dream. It had all come really quickly and nothing had gone wrong, right till the end where you had a little rash, you got admitted and was found to have high blood pressure, which you reckon was seeing doctors and being in hospital.
And from that point on, it all became quite medicalized and you were booked for an induction. Do you want to tell us what happened next?
Sarah: Yes. So the planned home birth I wanted was out of the window. Um, absolutely devastated, but obviously wanted to follow what was right. And obviously it was a, the pre-eclampsia risk that, um, doctors were concerned about. I was really, really terrified because all I'd heard from friends who had had inductions were absolute horror stories.
And that went ahead with it had a PEs, the Pessie. Um, but within an hour or so, I started getting contractions and they were absolutely, unbelievably painful. Um, and they didn't stop.
And on top of that, I had a reaction to the PEs. So the insides of my vagina were incredibly, incredibly, like sore and painful. So any. Investigations down below were agony. But I wasn't really dilating at all at this point. I mean, to me, my body just wasn't ready to give birth.
Um, and probably the fat that I was so tense didn't help either. Um, anyway, we cont continued for a few hours. So, however, during this time, kit was being monitored. Um, and at first was, was thought to be okay. Um, but then there were some concerns around Kit. So at that stage it was suddenly category one cesarean section, and I was rushed into the operating theater
But Kit was born and he was born healthy and he was absolutely perfect, sweetest, sweetest little boy. Um, started crying straight away, had his AGPAR test and scored 10 out of 10. No concerns at all. Um, was given to me and James were doing skin on skin. And it was all like, I mean, I'll say it was all amazing, but it was, it wasn't because I was still in agony and it was, um, the exact opposite of the birth that I had planned.
And, but still we had our son and he was amazing. Um, and we thought that was the end of the nightmare. Um, and his blood sugar was found to be too low.
Um, and also at this stage he was a little bit cold as well. So there, there was some attempts to try and bring it back up. However, it was decided that he was at risk at this stage of getting ill. So he was taken into the special care baby unit.
Emma: So Sarah, You'd been through this awful birth, which was the exact opposite of everything you'd hoped for, which was a nice home birth. But as you said, you had the boy of your dreams, you were, it was everything. Seeing Kit. Had you thought what might happen after your baby had been born and had you ever considered that your baby might not be Well?
Sarah: Um, it just didn't cross my mind. And also, I guess at that stage we had met Kit and he looked like a very healthy, happy. He almost looked like he was smiling in the, his first couple of hours.
Um, he looked like a healthy baby. So even when he was taken into special care, I didn't think he was ill. And actually I was just desperate to get him home. Um, I went along with it, but till now I wish I hadn't. I wish I'd just taken him home and he might have still been here today.
Emma: So is this bit, you've been through this hellish labour, but you've got your baby, he's amazing and he just has slightly low blood sugars and he is gone to the special care baby unit and all you want is to have him back. What happened next?
Sarah: So he was taken upstairs. I was physically unable at that stage to go with him. I couldn't move. Um, so we decided James should go up with him, my partner. Um, and I was downstairs and that was absolute torment. I felt like he had been taken away from me. It really felt like that, like almost against my will, although of course it wasn't against my will.
We'd given consent, et cetera. But it felt like my son had been taken away. Um, and it was a, it was, wasn't until another few hours that I think James managed to get a wheelchair, managed to put me in the wheelchair and take me up to see Kit and pretty sure I was crying for most of those hours. Just so sad that after everything we'd been through and then for this to happen.
Um, and also I was kind of, yeah, pretty sure that he wasn't ill. I just really wanted him home.
Emma: And you were right because, um, they gave him some feeds and then he came back down to you a bit later, didn't.
Sarah: He did. It took six days. So although he had a trip downstairs still whilst he was in the special care unit, he was a, he was taken downstairs to see me at some, at one point when again, I wasn't well enough to go upstairs.
Um, and it was during that time where there were red flags that we now see as red flags, but at the time we didn't know. So kind of from day three, four, um, he was really, really sleepy. So he wasn't waking up for feeds.
I think he only woke up for about 20 minutes a. . Um, I was asked, I asked doctors, nurses, midwives, like, is this normal? You know, everything you hear about newborn babies is that they hardly ever sleep. They cry all the time. And Kit was hardly crying. Barely at all actually.
Um, and I was just told that he was a sleepy baby. Some babies are sleepier than others. Um, boys are sleepier than girls. Maybe it's because I'm allergic to codeine, so I'd have morphine at the birth. So maybe it was a after effects of morphine in my breast milk cuz I was at this stage trying to breastfeed him, but also pumping milk for the, um, bottle feeds.
Um, maybe it was that he was having too much milk because they're trying to get his blood sugar up. , there were all these reasons given, and I, I know my Google search history at the time is just like, how much should baby sleep? Why is my baby not waking up? Et cetera, et cetera. Um, but I was reassured that that is normal.
Emma: So Sarah, you told me that even though Kit was upstairs on the special care baby unit, you were worried that something wasn't right because he was sleepy and he was hardly crying and you even described how he didn't cry with painful stimuli.
Sarah: Yes. Yeah. So that was another thing that we were asking about. I mean, I think at this stage I wasn't necessarily worried. I was asking the questions, but because I was told it was normal and there was nothing to worry about, it was kind of Oh, okay. Even though that didn't, it didn't feel right.
We were consistently told that it was fine. he didn't respond to pain at all. So he didn't wake up often. He didn't wake up for the heel pricks that he was having, what feels like thousands of, um, and even when his cannula was, were being inserted, he didn't respond at all.
And, and I remember talking to James and talking to one of the nurses about it, like, why, why is he not responding?
Emma: So you are telling me that when somebody put an intravenous cannula, so uh, a line into his vein to give fluids, he didn't wake up and he didn't cry.
Sarah: Yeah. Correct. So if he, if he was awake at the time, which was rare, he. He didn't cry. Um, didn't wim her, didn't yeah, didn't flinch. Which we, we thought was unusual, um, but we're told it was normal.
Christo: Sarah, at this point, um, what communication, uh, had happened between you and either kind of midwives or the nurses and doctors on the special care baby unit to explain, um, because by this stage he'd been up on the unit for a few days, is that right?
Sarah: Yeah, so at this stage it was just a case of he, this is very normal for even full term babies born by caesarean.
Um, he's just taking a little bit longer to get stabilized. Um, we're being extra cautious to make sure he's okay. Um, and it wasn't until he was six days where they were happy enough with all the observations that he could then get discharged to the postnatal ward.
Emma: And you did manage to get your son home, didn't you?
Sarah: Yes. So he was down with us on the postnatal ward, um, on day six, I should say. This was pre covid, so thankfully I was in the whole time cuz I was still quite poorly. But James could stay with me
So we, we we're absolutely delighted to get kit back to the postnatal ward. He fed quite well, breast fed quite well on his first night there. Um, but the next day there were some concerns about whether he had jaundice or not.
So he was put under that special light, um, but that stabilized quite quickly and he was actually allowed home on his seventh day.
Emma: And how did it feel to get him home?
Sarah: Um, it was really mixed feelings. I was, we were absolutely so happy to have him home. Um, but at the same time, I was desperate to establish breastfeeding and it wasn't happening and I was in agony and. And that's, I think that that just felt like the only way I could help him at that stage, and I wasn't able to do that.
Emma: Why was it so painful to breastfeed? So with something else that worried you then wasn't there?
Sarah: Yeah, so I think it was about day four or five when I started getting blisters on my nipples from one of them particularly.
Um, and at the time I raised this with the midwife and also one of the neonatal nurses, and she got one of the breastfeeding specialists to come and speak to. Um, and at that point the blisters were thought to be as a result of using the wrong size like breastfeeding found.
Um, I was googling as usual, suspected flush. It was tested for flush, um, found not to be flush. Um, and what we now think is, you know, that's, that was a sign of HSV that perhaps kicked had transferred to me, and that was one of the signs that wasn't picked up.
Emma: So Sarah, these blisters, they were very painful, weren't they?
Sarah: Yeah, really painful. So it was, it made. Expressing milk. Really difficult, very challenging.
Emma: And how did they develop or heal?
Sarah: it just started as like red soreness, which I guess is expected with breastfeeding. Um, and then it was only a bit later that I noticed some blisters.
Emma: Um, and just at this point, having saw nipples when you start breastfeeding, I think that's really common.
But having blisters is quite unusual. And you'd never had blisters before and you'd never had cold ulcers either had.
Sarah: No, I've never had colds in my life or blisters anywhere that I can remember.
Emma: Yes. You, you, I know this is a bit personal, but you've not had genital herpes either.
Sarah: No, absolutely not.
Emma: Did you think it was anything else at the
Sarah: time? Uh, I didn't know what it was. I, I, I took what I was told to be the truth.
Emma: So we'll come back to those funny blisters a bit later. But meanwhile, you've been struggling to breastfeed.
It's been agony. Kit has got home, but he's still sleepy. But things weren't right. .
Sarah: Yeah. So after we got home and kind of announced his birth to the world, which we hadn't felt comfortable doing until then
Um, but we did, and then it was that first night where Kit just didn't really wake up at all. you know, we had our instructions about he has to take this much meal every two hours. I think it was at the time. Um, because Kit had been so sleepy, we'd been given techniques to wake him up, like strip off his baby, Glu grow, um, blow on his face, tickle his toes, but none of these things were working.
And he had hardly any milk at all that first night. And then the community midwife came round the next day for her, like day one visit. and I told her about my concerns and at this point he started to look a bit more yellow again. So I showed her a photo of him the night before and him that day, and she agreed that he did look a bit more yellow.
Um, she said in every other respect, he seems like a healthy baby. His tone is really good. Um, he looks really well, but she agreed he does look a bit more yellow. Um, so she recommended then that we take him back to the children's hospital to check again for jaundice, and she thought that the jaundice might be the cause of his tiredness.
Emma: just as you think that you're ready to get the congratulations and that your baby is back home with you, he seems more unwell and jaundice and sleepy, and you take him back to hospital. And what happened next?
Sarah: So we got to the hospital and saw a doctor really quickly. Um, and that doctor immediately recognized something in Kit that he was a poorly baby, um, and admitted him straight away and he was put back on antibiotics and his infection markers were high. Um, within a few hours, his care was escalated to the higher dependency unit in the children's hospital. Um, and he was, you attached to all the wires. Um, and he remained there for the next five days until he was 12 days old.
Christo: How did it feel, Sarah, to go from, uh, having your delivery and the first few days of Kit's, life being very medicalized to then going home, uh, and then to be thrown back into, um, another very medical and clinical, uh, situation with, um, high dependency care?
Sarah: Um, getting home was so nice. , I was just, from the minute I was admitted to hospital, I was desperate to get home and then subsequently to get Kit home. And then to go back, I, when I went back, I thought it would just be, he would just be under the lights for a little bit longer and then he would, we would have him home again.
But when he was admitted, yeah, it was like all our nightmares come true. Really. And just absolutely devastated to be back there.
Emma: So Sarah, you talk about how you've been at home and you've just been a bit sleepy and not feeding and you come back in thinking perhaps you'll just need the lights. But in fact, he needs antibiotics, he needs fluids. He's on the high dependency unit. Does anybody know at this point, what's the matter with kit?
Sarah: Lots of tests were done. So he had a lumber puncture. Um, There were various theories, like maybe it's a metabolic condition, maybe he's allergic to my breast milk. Cuz they, there seemed to be a pattern there, um, I guess all the usual tests that at no point was Hs feet suspected or tested for.
Emma: So Kit is now seriously unwell and he is getting a lot of treatments, but he is not getting better, is he?
Sarah: So at this stage, the doctors were still telling us that we would be home in, it was days and then it was weeks, but it was, we will be home soon and this will just feel like a bad dream. It was a difficult start to Kit’s life, but we'll have our little boy in our arm soon enough at home.
Christo: When you were speaking with the doctors and they were trying to find out more information about what might have led kit to be unwell, did they ask questions about your health, so about infections prior to delivery, or about any warning signs that with retrospect might have related to hsv?
Sarah: No, they didn't ask anything.
Um, so the, the, the big warning sign that was we there, which I've already talked about, is the blisters on my nipples, and they were well aware of these. In fact, James, who was my champion, was fighting for me to be seen by anybody because I was in so much agony from these blisters. Um, but they were never connected to kits, welfare kits, health.
Emma: So at this point, you and Anny, you've still got these funny blisters around your nipples and kits, despite everything that is being done for him is not getting any better.
How did things change from there on?
Sarah: So on his 12th day, it was by this stage he was having seizures, um, struggling to breathe grunting, which is the medical term for what we just thought as he just sounds like he's in a lot of pain.
But then he just start, he did start to look really unwell and really sad to be honest. . Um, so yeah, when he was 12 days and he was having all these uh, deterioration, they decided that he needed to be taken to the intensive care unit at the Alina.
So he was put in an induced coma and he was rushed up to the hospital there. And
Emma: How did that feel?
Sarah: So that was really difficult. That was the first time anyone had mentioned that your son might die. So that was an absolute shock.
We had to go behind kits in the car cause there wasn't room for two of us in the ambulance. Um, that alone was really difficult because Kit had always had one of us by his side until that point, except for his lumber puncture, and that was the only point that he hadn't had a parent by his side.
Emma: So you described Sarah, how, um, this is the first time you suddenly think, actually Kit is seriously ill and he may not survive, but so far nobody really knows what's wrong. Did they have some ideas when you got to the Alina Children's Hospital, which is in London?
Sarah: Yes. So when we first got there, one of the first things a doctor said to us was, have either of you had a cold?
So recently, because I suspect this could be herpes infection. So he sees several, often tragic, usually tragic cases by the time they get to him, um, a year. So Hal Kip presented that kind of overwhelming infection. Uh, the, he'd had, I think he had liver failure. So I think that was a warning sign for the doctor.
Um, and that was the very first time that we had heard the word herpes and were like quite shocked to be honest.
Emma: And what was your first thought when you were told he might have herpes?
Sarah: Um, I've never had a cold saw in my life.
We kind of moved on like I did Google it, but. We kind of dismissed that as it wasn't the cause at that stage, I think.
Emma: And things didn't go as you hoped. Kit didn't get better.
Sarah: Um, no. So by the time he was admitted into intensive care, they were just doing all they could to save his life.
They did send his blood off to be tested for various things, including H S V, but they knew that even if it was H S V at this stage, like they, it's too late to be just starting antivirals.
They needed to stabilise him first. Um, and it seemed like they had stabilized him, um, and recommended that we go downstairs and try and try and get some sleepand then we got a phone call saying, you need to come upstairs. And so we did. We kind of knew what we were gonna find, I think, at that stage. Um, and we found a doctor desperately giving CPR ticket to try and bring him back to live. Um, but it didn't work.
And he, yeah, he, he died shortly afterwards.
Emma: Sarah, I'm so sorry. This must be so hard for you to talk about this. I think the thing that makes it so difficult is that horrible, inevitable feel that things are getting worse and you still don't know why at this point. Did they ever find out?
Sarah: Yes. After he died, We held him for a little bit, but by that point he didn't feel like kiss anymore.
I remember saying to James like, this isn't our little boy. He was really swollen. Kit was so like delicate and perfect, He, he just didn't look like him anymore and he had died so he didn't feel like our boy anymore. Um, we were taken home shortly afterwards, so we had to leave kit there.
Um, and we got a knock on our door of a couple of hours after we got home. A pair of police officers because at this stage it's an unexplained child death. Um, so officially we are suspects, I guess, and I absolutely don't fault that system. That's what should happen in a circumstance like this, but it was an extra.
Kicking the teeth to us. Um, they interviewed us. Um, left still had no answers. And it was not until the next day the police officers came back. They'd heard from the hospital that he had a diagnosis of H S V one, um, and that was what was gonna be put down as a cause of death. So the HSV had caused the organ failure, um, because it was a disseminated herpes version.
Emma: So Kit had died of type one herpes sinex virus, the virus. That gives people simple common colds.
Separate quote: we would ask any clinician working with newborn babies to not work clinically if you have a cold sore.
Emma: Uh, thank you Sarah. This is a terrible story and outta that terrible story, you've actually done amazing things, which is start a charity in Kit's name that champions working with hospitals and foundations around herpes simplex for the Kit Tarka Foundation.
Do you want to tell us a bit about it
Sarah: I did speak to a number of larger charities to see if they would help with what at the time was an obvious gap in the research. So the latest, the latest BPSU study that had been published at that time was 25 years old. There was an interim, interim one, which hadn't, I think it only got published a couple of years ago.
Emma: So Sarah, once you'd started thinking about it, you actually found there was a big gap in the knowledge around herpes simplex and how it affects babies. So there wasn't any recent research or studies, there wasn't much for public awareness and there wasn't enough for clinicians to be aware of what they should look out for
Sarah: Um, obviously there was a huge gap there amongst health professionals, doctors, um, on that side, what to look out for in babies, that kind of non-specific signs.
It's not always a bacterial infection. It could be a viral infection. Um, and on the other side, there was a huge gap in knowledge amongst parents.
Emma: That's amazing. And I think you're so right. I think viruses are really neglected and you've done more than that because you've also done a public awareness campaign called Thank. Haven't you, do you want to tell us a bit about that?
Sarah: Uh, yeah, so off the back of that survey we launched the Thanks campaign, which is Think Hands and no Kisses. Um, so it's all around the importance of good hygiene around newborns. Um, a lot of parents told us that although they let other people kiss their baby and don't wash their hands, they're not comfortable with it and that they don't want to be seen as overprotective parents or they feel awkward having these conversations. So we produce all these resources, posters, um, postcards, et cetera, and social media campaigns who kind of empower parents to make those decisions for their vulnerable newborns.
Emma: have you got three top tips or three top messages that you would like new parents to know?
Sarah: Um, don't let anyone with a cold sore near your baby. Don't let anyone hold your baby without washing their hands, and, and don't let anyone other than the parents kiss your baby.
And this might be number four, but anyway. Any expectant parents. If you have any known history of genital herpes, then please, please, please talk to your, um, midwife about it or your obstetrician. Um, don't be embarrassed. 25% of the population have genital herpes infections. Um, and we know that's actually is the most common way that babies contract HSV.
Emma:. This is such a tragic story and I think that your message of parents not knowing what is the right thing to do as in washing your hands and not exposing your baby's cold source, and clinicians not recognizing these nonspecific symptoms and treating it early and thinking about hsv herpes simplex virus, and.
Us not being open and talking about herpes so that we can do something about it, have all led to this awful tragedy that is part of your family history.
Sarah: Um, another thing that really surprised us from our survey was that only 15% of our respondents were us during pregnancy about previous genital herpes infections.
Um, I'm nearly 50% of birthing per appearance with a known genital herpes infection said it was not discussed at all during, with a health professional during pregnancy.
Emma: And that survey led you to lobby and change a whole lot of things, didn't it?
Sarah: Yeah, so one of the main changes that's come out of that is the nice antenatal guidance We, um, campaigned for that to now include information on herpes to be given to all expectant parents, and that's in there now, which is brilliant.
Emma: So Sarah, it's been a tremendous privilege to talk to you and to hear your story and hear about Kit, and I think that you need to reflect that it's, you one person has changed so much. You've changed the way clinicians think, you've changed how parents think, and you've changed policy at a national level, which is an incredible achievement for any one person.
[music]
This podcast is a collaboration between Odland, medical education and the Royal College of Paediatrics and Child Health. You can find more creative learning resources and a wealth of information on the important work of RCPCH on www.rcpch.ac.uk or #ChoosePaediatrics.
[music ends]
-
EPISODE 2: Neonatal herpes simplex virus disease – mother-to-child transmission (released 5 December 2023)
Special guest Dr Hermione Lyall joins our hosts Emma Lim and Christo Tsilifis to talk about maternal to child transmission of herpes simplex virus and the importance of early detection of this rare condition.
Hermione is a paediatric infectious diseases consultant at St Mary’s hospital in London and brings a wealth of experience to this discussion. She has a special interest in congenital infections and has worked tirelessly to prevent their transmission, which she discusses at length in this second of our three-part series on HSV.[music, with snippets]
Emma: When you see these mothers and parents, and you have any hints that it could be herpes simplex, you need to make everybody horrified. You need to have these babies clean and assessed clinically.
Hermione: People haven't seen enough of it, to have it in their mindset when they see a sick baby. So there may have been a history of exposure, from the mother, from the grandmother, from anybody. There may have been a history of exposure, but people haven't asked.
[music ends]
Emma: Hi there, I'm Emma Lim, a consultant paediatrician at the Great North Children's Hospital. You're listening to The Paeds Round, a monthly podcast and the Royal College of Paediatrics and Child Health. Every month we invite experts to answer important questions on the issues that matter in paediatrics, from areas as wide ranging as obesity, to social media. So, thanks for joining us on our rounds.
This is our second episode of our special edition on Herpes Simplex or HSV, and it is my great privilege to have our next speaker here with us. Dr Hermione Lyall, and Hermione is going to talk to us about maternal to child transmission of herpes simplex virus (HSV).
Hermione, would you like to tell everybody what you do and where you work?Hermione: I'm a paediatric infectious diseases consultant and I work at St. Mary's in London. I have been doing this for quite a number of years, and I have particular interest in congenital infections and trying to prevent mother to child transmission of congenital infections. And that includes a number of viruses and also bacteria, and of course HSV.
Emma: Thank you. I always feel that viruses are somehow underrated and undera ppreciated.
Hermione: Okay, so I think one of the biggest issues here and we're really talking about neonatal Herpes Simplex, infection that comes on in the baby after it's born, rather infection that it's actually had in utero for some time and that it is born with, which is congenital herpes simplex, which is exceedingly rare. And I have looked after two children with that condition over the last 25 years, and that is devastating destruction of the brain and other organs by the infection, but that is an extremely rare presentation of herpes simplex.
Emma: Hermione we're talking about two different scenarios here. Congenital herpes simplex, which is devastating and very rare, and neonatal herpes simplex which are going to tell us more about now.
Hermione: So even neonatal herpes simplex is still a rare condition. And this is one of the biggest problems, that people haven't seen enough of it to have it in their mindset when they see a sick baby. Neonatal herpes simplex has been increasing. And Katie can tell you more about the latest BPSU (British Paediatric Surveillance Unit) survey. But you know, it's still only somewhere between maybe 5 or 70 babies per 700,000 live births. So that means that most paediatricians, unless they're in a very specialised unit, will not seea baby with neonatal herpes simplex during their training.
Emma: And so, there's rare occasions, and I think it is really hard to remember this. What do you want them to think about and ask about?
Hermione: So, we want to think about women who are pregnant. Now, unfortunately, if you look at it from the baby's end, about 80% of the time when a baby has neonatal herpes, nobody has picked up that the mother had any symptoms, or that there was a risk of infection. And indeed, the infection doesn't always come from the mother. In somewhere between 70% or maybe even up to 20%, the infection may have come from someone else, whether that wasa healthcare worker, or a family member, or somebody else who has been involved with the baby.
So, the classical thing that people get taught about is a woman delivers with lesions, ulcers, or vesicles at the time of delivery, and there you think, oh my goodness, could this be herpes simplex? But the chances of that happening are actually extremely rare, and even if a woman has herpes simplex at the time of delivery, she may have no lesions at all. She may be systemically unwell; she may not actually develop the lesions until a few days later. She may have very painful vaginal grazes or symptoms a few days after the delivery, and people may be saying, oh this is thrush, or this is bacterial infection. And because they don't see blisters, they don't think of HSV.
Emma: Alright, so you were right, all neonatal illness starts in pregnancy. So we need to be really mindful of thinking about asking mothers about any rashes they've got, any blisters they've got, any blisters on their fingers, as well as in their vulva or vagina. But more importantly, what you're telling me is that most of the time, these babies turn up with very nonspecific symptoms, and really no history of being exposed to herpes simplex virus.
Hermione: Well, even worse than that, people don't ask. So, there may have been a history of exposure, from the mother, from the grandmother, from anybody. There may have been a history of exposure, but people haven't asked. And they may not have asked the right question, because the mum may have been really sick with a high fever and very unwell, and it's all assumed to be bacterial infection, but it could just as easily be primary herpes. That's just the situation if you're really looking at it around the time of delivery, but we also have to think about the weeks and months before that. And if a mother has herpes simplex genital infection in the weeks in the third trimester, so say after 28 weeks, her baby is still at risk. Because it takes a bit of time to produce an antibody response. She needs to be treated; she needs to be referred to the GUM (genitourinary medicine)
service. She needs to get on to acyclovir and she needs to stay on acyclovir until the time with the delivery. And indeed, if it's later in that third trimester, she should be offered a caesarean section.
Emma: Is there difference between women who are meeting herpes simplex for the first time and a reactivation?
Hermione: Okay well, it's not straightforward either. If you had your first herpes earlier in that pregnancy, and you could be having a reactivation, your baby is probably still a bit more at risk, so you needed to have been treated then. And you also needed to have been offered the opportunity to go on to prophylaxis in good time for the delivery. The current RCOG (Royal College of Obstetricians & Gynaecologists) and BASH H (The British Association for Sexual Health and HIV) guidelines only suggest going on to prophylaxis from 36 weeks gestation.
But there are two really important points here. One is that herpes simplex itself increases your risk of having a premature delivery. And in addition to that, the babies who become sickest and are more at risk of dying from herpes simplex are premature babies. So in our view, actually women should be offered to go on to prophylaxis from much earlier. There's a recent Ugandan study, which looked at this, and in that study, women went on to treatment from 28 weeks. In the original studies, women who had antibodies protective antibodies, their babies had a much lower risk of complications. But I don't think it's necessarily so easily black and white. And I think women, especially women who've only had herpes simplex in the last year or two they need to be offered prophylaxis.
Emma: So the Royal College of Obstetricians and Gynaecologists (RCOG) guidance and the British Association of Sexual Health and HIV (BASHH) suggests we should start acyclovir prophylaxis from 36 weeks. But know that acyclovir is safe, it's relatively easy to take, and it could prevent devastating disease and death like we've heard from Sarah.
Why do speak that people aren't offering prophylaxis so often?Hermione: I think, firstly, they don't ask the question, they don't ask if women have had genital herpes or not. Secondly, as we said, there are plenty of people who may have had genital herpes and they didn't know it. I think we don't routinely tech check women serology and it would need women to be referred to GUM to actually have this properly assessed, which I think very rarely happens.
Emma: People don't want to disclose it? You must remember that sometimes people's partners don't know that they have genital herpes. And I also think in the general public, there is a not an understanding that this is a treatable condition, and that this may cause illness in a neonate. So I think these things are really not well understood. I think you've put how difficult the situation is in diagnosing and treating herpes simplex in pregnant mothers. But when it comes to it, and you're faced with a child, who potentially has it, what should we be thinking about at that point, and who should we suspect of herpes simplex infections?
Hermione: Okay, so I am going to just usesome cases that I've been involved with, which I think are very clear examples of where we can think better. So, here's a baby who was born normal delivery to a teenage mum, and bear in mind actually, teenage mums have a
higher risk of having herpes simplex as a primary infection. Normal delivery, everything was fine. And about four or five days the baby was noted to have some crusty lesions on the head. It was taken to primary care, a diagnosis of staph aureus infection was, made the baby was started on flucloxacillin. New blisters and crusty things continued to appear, and a couple of days went by,and it wasn't really improving. Then it just gradually settled down. And a few days after that, the baby was found in status epilepticus, and was admitted to intensive care. And this baby had devastating brain damage from herpes simplex and encephalitis. The baby has four limb cerebral palsy, is cortically blind and his life has been changed completely.
Now, if that first person who saw those crusty things on that baby's head had thought, this could be staph aureus, but it's a presenting part with crusty lesions, and maybe some little blisters this could also be herpes simplex. If that person had thought about that, and admitted that baby, and done the investigations, and started that baby on acyclovir, it's quite possible that that baby would only have presented with what we call skin, eye and mouth disease, and would not have gone on to develop and encephalitis with its devastating outcome.
Emma: As a quick summary, when is the highest risk period of being infected with herpes simplex virus during pregnancy?
Hermione: I think the most dangerous time is where the maternal infection happens right at the end of pregnancy, so that the mother is by remake, and there's a placental transfer a virus, or the mother has lesions in the birth canal, and the baby picks them up at the time of delivery. So this is the most dangerous time.
Emma: And you said teenage mothers were more risk of herpes simplex virus. Who else does more risk?
Hermione: So young women, women with HIValso are more at risk and it also depends on your ethnic group. There are some ethnic groups that are more risk as well. So young women, Afro Caribbean women also. But fundamentally, it's all women who are having sex. So, and because it's a very rare condition, you have to think about it for everybody.
Emma: And let's face it, if you're pregnant, you must have had sex at some point! Just as a summary, you and I think about acyclovir like vitamin A, like who shouldn't take it? But, what are your recommendations?
Hermione: My view on this would not be the same as the current RCOG and BASHH guidelines, because I think if you have a woman who presents with herpes simplex for the first time in pregnancy, you should probably go on to acyclovir from then and continue on it right to the end. If you have a woman who has recently become infected, or whom for some reason is diagnosed to be infected, she should start on the treatment, especially if it's beyond 24 weeks gestation, and stay on it.
Emma: I think that, as you say, taking acyclovir it's not unsafe, it's not going to harm their child. I think we're very few reasons not to.
Hermione: And actually, we would normally give valaciclovir every year, which is the pro drug of acyclovir, and only has to be taken twice a day and the dose that you would use for prevention of herpes simplex is very, very well tolerated. But obviously women need to be advised to keep well hydrated, because you know, it's renally excreted so you want to make sure that they are in a good hydration state.
Emma: Okay, so my last question is, of course, caesarean section. Talk for me about the risks and benefits of caesarean section in mothers with herpes simplex virus.
Hermione: So, the classical situation is if you have a woman who is found to have vesicles, or ulcers at delivery, and it's considered that she's having primary herpes at the time of delivery. Trouble about that is that you have to go on your clinical expertise, because you won't have time to send a swab to the lab, and you won't have time to check the mother's serology. So, you have to make a clinical decision about that, and as we said, very often women don't have obvious genital lesions, so making that diagnosis of gentle lesions at delivery is really difficult. In addition to that, if the membranes have already ruptured, the longer they've ruptured for, then the less likely the baby is going to be protected. So, people do say that if the membranes have ruptured for less than four hours, then it's still reasonable to do a caesarean section.
If you know a woman got primary herpes a few weeks before, in the third trimester, then you would definitely want to offer her an elective caesarean section, and she should obviously also be on her acyclovir prophylaxis. If you have a sick woman at the time of delivery, and you're worried that shecould actually be viraemic with herpes simplex, then you should be offering that woman to be on intravenous acyclovir.
There are all these different kinds of nuances to it. And what it really means is that you need very good interaction between obstetrics, midwifery, virology, adult GUM, neonates, PIO everybody needs to be working together putting their heads together and thinking.
Emma: I think that's so important. You've talked about the risks in premature babies, you've talked about premature ruptured membranes, and you've talked about really sick women that could be viraemic, women who have had really recent herpes simplex virus infections, and the need for them to have really joined up care between all these different departments. Do you have three top tips for us?
Hermione: Okay, I think the most important thing is that if you have a woman who has severe pain in the vaginal area, a woman who is unwell and everybody thinks she's got Group B strep, but the cultures are negative. If you've got a woman who has new lesions in the third trimester, around the time of delivery or after the delivery, you still have to know that there is a risk to the baby of herpes simplex infection. It's always putting the kind of bits of the jigsaw puzzle together, and it's asking that question to the woman herself, about exposure and to the neonatal team and to the kind of obstetric team.
People have to think about it.The particular things that make me worry are any baby with abnormal LFTs (liver function tests), any baby in DIC (disseminated intravascular coagulation), any baby with abnormal neurology. All of these babies should be given acyclovir until you've either proven something else or you've got HSV. We should also be making sure that we get rapid test
results, so we should get biofire or rapid PCRs (polymerase chain reaction) back on CSF (cerebrospinal fluid) from these babies. And like you said, you need to send a blood PCR, but we can get rapid results, which is really helpful.
Emma: I think that this is really important. First of all, all sick babies deserve the right to have some acyclovir. The other thing for me is your last point is that it's quite easy to start acyclovir but it's really hard to make a decision stop. And we will never know if we can safely stop if you haven't sent tests off. When you see these mothers and parents, if you have any hints that it could be herpes simplex you need to make everybody horrified, you need to have these babies seen and assessed clinically, you need to have done all these investigations and possibly started them on acyclovir before they come to the stage where it's irretrievable.
Emma: Thank you very much Hermione for a fantastic episode. The Royal College of Paediatrics and Child Health, British Association of Sexual Health and HIV Guidelines for the Management of Herpes Simplex in Pregnancy and Neonates are currently out to consultation. There are some changes and, in it, the advice for prophylaxis in pregnancy has been updated to: please start acyclovir from 32 weeks generally or 22 weeks in any women where there is a suspected risk of prematurity. For more information, please look at: www.bashhguidelines.org
[music]
This podcast is a collaboration between Odland, medical education and the Royal College of Paediatrics and Child Health. You can find more creative learning resources and a wealth of information on the important work of RCPCH on www.rcpch.ac.uk or #ChoosePaediatrics.
[music ends]
Emma: The views, thoughts and opinions expressed in this podcast relates only to the speaker and not necessarily to their employer, organisation, the Royal College of Paediatrics and Child Health, or any other group or individual.
-
EPISODE 3: Neonatal herpes simplex virus disease – Management (released 19 December 2023)
We’re back for episode 3 of The Paeds Round with special guest Dr Katy Fidler joining our hosts Emma Lim and Christo Tsilifis to talk about the management of herpes simplex virus. We discuss stigma, when to worry about HSV, the importance of early detection and what to look out for. Katy is a Paediatric Infectious Diseases Consultant in Brighton and a Reader in Paediatrics at Brighton and Sussex Medical School. She also currently runs the national study on neonatal herpes through the BPSU. This is the final episode in our 3-part mini-series on HSV and we’ll return in the New Year to discuss fever.
[music, with snippets]
Katy: We can treat it if we know early enough.
Emma: There is such a stigma about herpes simplex virus.
Katy: Your result is only as good as the swab you take.
[music ends]
Emma: Hello, welcome to The Paeds Rounds. We host a regular podcast from the Royal College of Paediatrics and Child Health on key issues affecting paediatric practice. My name is Emma Lin and I'm a consultant paediatrician at the Great North Children's Hospital in Newcastle upon Tyne. I'm here today with my co-host and colleague, Christo Tsilifis, and this is our final episode of three on herpes simplex virus (HSV) and today we're looking to round up our learning from what we've heard before, from Sarah and Dr Hermione Lyall.
So, let's get started with today's round and hear from Dr Katy Fidler, a great friend and colleague of mine who I've known for a very long time. Katy, would you like to introduce yourself?
Katy: Hi, Emma. I'm Katy Fidler, I'm a paediatric infectious disease consultant in Brighton and a reader at Brighton and Sussex Medical School. And, also I currently run the national study on neonatal herpes through the BPSU (British Paediatric Surveillance Unit).
Emma: Katie, what do you want to tell doctors about when to worry about HSV and what to look out?
Katy: Well, and the neonatal HSV can present in one of three different ways: with skin, eye and mouth disease; with a CNS (central nervous system) disease, so encephalitis; or with disseminated disease. And for the first two of these, presentation may be easy to recognise, because they have skin lesions or they may present with fevers and seizures. But it's this last group with disseminated disease that is really, really difficult to recognise, because they present very nonspecific symptoms, of poor feeding, lethargy, they may present with a sepsis picture, but everybody will think they've got bacterial sepsis, and not think about treatable viral sepsis.
Emma: Thanks, Katy. I think the difficulty is that basically babies don't present in many different ways when they either get a fever, or they cry, or parents come in and say they're just not themselves. So, is there any time you shouldn't use acyclovir? Because it seems to me that it will be really hard to unpick beforehand whether this is a HSV infection or not.
Katy: I think that's a very good question Emma, about when you shouldn't use acyclovir. From an infectious disease point of view, we would like to consider HSV and starting acyclovir in pretty much the same way as you do antibiotics, that you start and then you can stop when the cultures are negative antibiotics, or the viral PCR (polymerase chain reaction) tests are negative, but HSV. However, we have to put that into the context of many, many babies presenting to the emergency department and how that would affect 1000s of babies per year.
Emma: I think that brings us back to that reminder, that Hermione talks about, to take a really good history and to talk to the parents. I think the second problem is that we don’t have good point of care tests. So, what we really would love is a point of care tests that will tell us if a child has HSV (herpes simplex virus), when you see them is that slightly sleepy and lethargic, possibly febrile and other moments when to care that don't exist like that. But what tasks can you do, or what tests should you Katy?
Katy: Well, I think the most important thing is to go back one stage, and even before the testing, you have to think of the diagnosis to send off the test. And we've done studies to show that when you ask registrars what diagnoses they consider in an unwell baby presenting in the first week of life, only 3% think of HSV, whereas everybody will think of bacterial sepsis. For instance, everyone thinks of listeria, however, listeria is not nearly as common as HSV in the neonatal population.
Emma: I think that's incredible, because the number of listeria cases in neonatal population is maybe two figures per year, like 10s or 20s.
Katy: Yes, so we know that both junior doctors, and indeed the public, are all very aware of listeria infection, but hardly anybody is aware of herpes simplex infections in neonates and what they can do to reduce their risk of babies getting infected.
Emma: I think that really goes back to that idea that there's such a stigma about herpes simplex virus.
Katy: Yeah, I think there's still a huge stigma around it and it's such a shame because of course, it would turn neonatal herpes into a much more easily treatable disease. Doctors should ask women in pregnancy, and those who are presenting in the emergency department if they have a history of this illness, because we can treat it if we know early enough.
Emma: And it is that horrible combination of being completely stigmatised to talk about genital herpes, and then also disregarding cold sores as anything serious so most people don't bother to treat cold sores, and don’t think that cold sores are in anyway serious.
Katy: Yes, and I think Hermione talked very nicely about what we can do to prevent these infections. And of course, prevention is better than cure, and she talked about the antenatal things we can do. But of course, between 10-25% of these infections are acquired postnatally, and we really need to educate parents and staff in hospitals about the importance of postnatal transmission of herpes from a cold sore lesion or a herpetic whitlow, and providing advice about how not to work with newborns or touch newborns if you have these lesions.
Emma: But what does a herpetic whitlow actually look like?
Katy: Well, it looks almost like blisters, often on the side of your finger, but it can also present like a paronychia, so redness around the nail bed, and it's often confused for a bacterial infection.
Emma: Let’s imagine we live in the world where you could have anything you want. What are the tests that you really dream about if you're concerned about HSV?
Katy: Well, in my dream world, we'd have a point of care test, like we have for COVID these days, to look whether a baby has herpes infection, when they initially present, so we can treat with antivirals at that point.
Emma: But we don’t, so what is our second-best real-world scenario?
Katy: So then we want to think of the diagnosis and take samples from as many sites as possible. Many people think of taking a CSF (cerebrospinal fluid) and sending this for HSV PCR, along with enterovirus and some of the other viral infections. However, we really, really want to catch these babies when they're at the by viraemic stage before the virus is disseminated. And therefore we have to take a blood sample, which is an EDTA (ethylenediaminetetraacetic acid), looking for herpes simplex PCR. So this is not the antibody test, the serum clotted test, which shows your response to herpes, we really want people to send off the viral DNA sample on admission.
Emma: What can you tell me about the kind of swabs we'd like?
Katy: Well, we want the viral swab, which in our hospital is a green swab not a charcoal swab, and it's the same swab of course everybody knows about with COVID these days. And what I would suggest is, any baby with any skin lesions, you may think it's erythema toxicum, you may think it's a staph infection, but please, please send that viral swab as well and you may get a surprise. This means you could start treatment earlier than if you forget that.
Emma: If we were to hit the jackpot and have every investigation that we wished for, that actually exists at the moment, we would like a CFS PCR, we'd like a blood PCR that's in an EDTA tube, and we'd like viral swabs of absolutely everything. So any blisters, any lesions, any redness, and anything that looks like a paronychia, and that swab would be a viral swab, which would be a green swab, not a charcoal bacterial swab.
Christo: Katy, Is there any value in popping blisters to get some of the fluid inside the vesicles?
Katy: Yes, I think we would like to pop the blister and really try and get that green swab into the base of the blister even if it causes a little bit of discomfort for the baby. Your result is only as good as the swab you take.
Well, it's a bugbear of mine that I've been training our juniors about for research studies, on the meningococcal disease, to doing COVID swabs. You don't get your swab to the back of the throat, or in this case to the base of the lesion, a negative result does not necessarily mean anything.
Emma: Katy, going back to our investigations. Remember, this is a baby who doesn't necessarily have a fever, who may look just a bit sleepy. We've talked about what investigations we'd like to try and isolate the virus, but what other tests would you like to do?
Katy: The tests that are very helpful would be the CRP (C-reactive protein) and that's usually low in herpes simplex virus, liver function tests because once your ALTs (alanine aminotransferase) start to rise, your risk of mortality increases significantly, and clotting because again, this can go off in these babies.
Emma: Okay, so we have a list of all the investigations would like. Do we need to talk about treatment?
Katy: I'd love to talk about treatment. I think it's very difficult, and a contentious area at the moment, because infectious disease doctors would like to treat all babies with acyclovir. It's relatively well tolerated; however, it does cause problems with the cannula and the veins, and the cannula tissuing.
Emma: So, although we like vitamin A and acyclovir, we'd like to give it to everybody, it’s a bit like thinking about antimicrobial stewardship, and we need to think who needs to have it. Or we could start it on more children and then stop it if we've done the right investigation. I agree with you, it's always difficult to give, we always struggle with cannulas, and I don't think I have a good answer for that.
Katy: I think any baby in which mum has any history of herpes illness at all we would treat. Any baby who is unwell with nonspecific signs of infection, or sepsis, it would be good to treat. And certainly, any baby who has abnormal liver function tests, or deranged coagulopathy, or who is not getting better after 24 to 48 hours of IV antibiotics.
Emma: And I think you were particularly interested in babies who are under 16 days old, in the first few weeks of life?
Katy: Yes, so we're conducting a national study at the moment and it does seem that the median age presentation with disseminated disease is about six days; with skin, eye and mouth it's eight days; and with encephalitis it’s ten days.
Christo: We worry a lot about antimicrobial resistance, do we need to be concerned about acyclovir resistance in HSV?
Katy: We're lucky at the moment that we don't seem to see acyclovir resistance very often in women who are treated or children who are treated with acyclovir.
Emma: We're still standing! I'm going to give you five minutes to tell us about the BPSU study that you have just recently finished, o that is the British Paediatric Surveillance Unit, which we were just talking about a bit earlier.
Katy: Yes, so this is a study we've been running over the last couple of years, where we look at all anonymous cases of neonatal herpes in the first few months of life in the UK and Ireland. We have interim results to date, the study is not fully concluded yet, but we have found most importantly, that the incidence of neonatal herpes infection has doubled again since the last study that Sarah mentioned that was undertaken about 20 years ago.
Emma: So that means I have to talk to you again, another excuse to come and meet up!
And finally, thank you so much for being with us, Katy, and for the enormous amount of work you've done in this area. And I think it's such an important area because of the lack of recognition and awareness of the horrible disease and the possibility that it could be avoided through a few questions and maternal prophylaxis.
So, do you have three top tips that you'd like to share with our listeners?
Katy: Three top tips are really that antenatal transmission can be reduced, as discussed by Hermione. Postnatal transmission will be reduced by good hygiene and not touching babies if you have a cold sore or a herpetic whitlow. And lastly, we can reduce mortality if a baby does get infected, by treating them early with acyclovir, the key to this is really thinking of HSV as a possible diagnosis.
As you know, Emma I've been badgering you for years to talk about treatable causes viral sepsis, as well as bacterial sepsis. And I think everybody thinks for things like enterovirus, and RSV (respiratory syncytial virus), and viruses that you can't really give specific treatments to, you just have supportive care. But herpes simplex is one of those viruses that you can completely alter the course of the disease if you treat these babies early and mustn’t be forgotten.
Emma: Thank you, Katie. It's the day of the virus, your time has come! I really appreciate it and it's been great fun to talk to you all and we probably should make a date to come and chat again once you've got all the results from the BPSU study.
Katy: Thank you. Thank you very much for having me on your podcast.
Emma: Thank you very much Katie that’s amazing and as always we add all our links on our show notes. For guidelines under management please look for the paediatric and microbial stewardship group. This can be found at: https://uk/pas.co.uk At the time of our recording the guidelines for the treatment of HSV were being updated. The general consensus among the UK paediatric antimicrobial stewardship network is based on Dr Fidler’s current BPSU data. The UK PAS guidelines for neonatal herpes simplex have now been updated. It is recommended for acyclovir to be used in the treatment of neonates with suspected sepsis and any of the following features:
ALT or AST greater than 2 times the upper limit of normal or abnormal liver function tests
Coagulopathy
Vesicles
Seizures
CSF Pleocytosis
Suspected Meningitis of Encephalitis
Recent maternal HSV disease
Post-Natal contact with HSV
The recommendations also strongly recommend considering acyclovir in neonates who present on days 3-14 with one of the following, in the absence of the above risk factors:
No obvious cause
Not improving
Or unexplained maternal, febrile illness peripartum to 14 days postpartum, especially if premature. Thanks you very much I hope you enjoyed the episode
[music]
This podcast is a collaboration between Odland, medical education and the Royal College of Paediatrics and Child Health. You can find more creative learning resources and a wealth of information on the important work of RCPCH on www.rcpch.ac.uk or #ChoosePaediatrics.
[music ends]
Emma: The views, thoughts and opinions expressed in this podcast relates only to the speaker and not necessarily to their employer, organisation, the Royal College of Paediatrics and Child Health, or any other group or individual.
-
EPISODE 4: What's hot on fever? (released 23 January 2024)
It’s January and all the children are back in school. And that means it’s a chance to swap viruses and herald in the new year with fevers!
This month’s episode has the answers to your questions as child health professionals on this burning problem. Should you worry about the height of the fever? Should you give antipyretics? How do you reassure parents and carers that fevers are part of everyday life?
All of these issues are discussed, along with a passionate plea to make hand washing great again. So don’t get hot under the collar, listen to The Paeds Round as we take time out to chat to special guest, Dr Alasdair Munro, senior clinical research fellow in paediatric infectious diseases at the University of Southampton (https://alasdairmunro.substack.com/about and https://twitter.com/apsmunro).
With your hosts, Dr Emma Lim and Dr Christo Tsilifis.
[music, with snippets]
Alasdair: Fever is a normal physiological response to an infection, and then if you're able to explain that to parents, you will change their whole perception.
Emma: Fever makes parents scared, they fear fever.
Alasdair: Make hand washing great again, that's my new motto!
[music ends]Emma: Hello, and welcome to The Paeds Round. This is a regular podcast and the Royal College of Paediatrics and Child. Health, and focuses in on key issues impacting child health. I'm Emma Lim, a consultant paediatrician and as ever, I'm here with my colleague Christo Tsilifis, and we're coming to you from the Great North Children's Hospital in Newcastle upon Tyne, and every month we invite experts to bring you important educational learning points. So, let's get into today's Paeds Round!
I'm very excited today to have a guest from down south, Alasdair Munro! So hello Alasdair.Alasdair: Hello, thank you so much for having me on, what a pleasure it is.
Emma: I've always been a big fan of yours for two reasons. Number one, we have a rule in our house that you can argue any point you like, as long as you have the evidence to back it up. So that's one of my big fan points. And number two, I always think if people have good ideas, but they don't tell anybody about them, there is no point having that idea. And I think it's so underrated the way we use social media and the way we put out important messages. And I think as paediatricians, we're really bad at this.
Alasdair: Well, thank you so much, that's a very kind thing to say. And I agree, I think the problem is that paediatricians often very humble and feel that they couldn't possibly have anything useful to add. If I know this, surely everyone knows this. But, as it turns out, there's lots of good stuff to learn, it's great to share it. As soon as you start sharing it, you realise that lots of people want to hear a lot of it and it's not all quite as obvious as sometimes we tell ourselves. So yeah, good to get the knowledge out there, I guess.
Emma: We did miss a really important point, because you didn't actually tell us what you do and where you come from.
Alasdair: Oh yes, let me tell you. I'm a paediatric registrar down in the South of England. I'm currently out of programme, working as a senior clinical research fellow in paediatric infectious diseases. I'm working in the NIHR (National Institute for Health and Care Research) clinical research facility in Southampton, and I've been doing my PhD. It was a very interesting time to be doing a PhD, because I wasn't very far in when COVID derailed the whole thing, but it's been it's been somewhat to my advantage as well. I've had some wonderful opportunities, working in vaccine science in the pandemic has been quite something else. My interest is obviously infections in children, and I do my clinical shifts in the emergency department, so most of my clinical work is primary care. So I’m seeing a lot of the bread and butter paediatric stuff, and I have a real passion for making sure that we can get that stuff as good as we can do.
Emma: And as always, I have Christo with me.
Christo: Yes, thank you very much Emma. I am Christo, I'm a clinical research fellow in Newcastle, in the final year of my PhD. I work closely with Emma in general paediatrics and infectious diseases, so it's really great to be able to have Alasdair with us. And I think you mentioned before that there are various ways in which you've tried to communicate various gems about general paediatrics infection. Where are some of the places that we can read more about some of the articles you've put out?
Alasdair: Oh thanks for asking Christo, allow me a minute to plug my material, thanks! So I use Twitter, the social media platform quite a lot, and you can find me through the tag @apsmunro and I tweet and share a lot of my stuff on there. I also have a newsletter on Substack. I can't remember the URL for that, but if you go to my Twitter the link is in the bio. And some of my old stuff is also on Don't Forget the Bubbles, which I'm sure most paediatricians will be aware of. But if you're otherwise involved in child health, and you're not aware, just Google ‘don't forget the bubbles’. It's an absolute treasure trove of clinical paediatric resources. And yes, some of my earlier blogs on there are still online. So that's where you can, go check it out. Some of them might be good!
Emma: Honestly, I think he must have paid you earlier!
Christo: We’ll have links to all of this in the show notes.
Emma: So let's get down to business. This is a really interesting topic because we all think we know quite a lot about fever, but we often don't answer the questions that parents really want to know. So I'm going to start at the beginning and this is a question that Christo put to me. What is fever? What is the definition of fever and what is normal?
Alasdair: Glad we can start with a very uncontroversial topic. Well, thanks for easing us in there!
What is a fever? Well, it's completely arbitrary in some senses, I guess we use it to indicate a raised body temperature outside of the normal limit, usually in response to an infection, but not always. And when does raise temperature become a fever? Now in the UK, I guess we would say usually above 38 degrees centigrade, some people would go even higher and say 38.5, the really hardcore people would cut it off there. But it's because we don't really know precisely what the normal range of temperature is and it's all based on sort of historical data that’s not quite as certain as it should be. In fact, it's amazing how many normal ranges if you go back far enough looking for the beginning end up this way! But we would normally say a normal temperature is somewhere between 36.5 degrees and
37.5 degrees. And then there's this beautiful grey area where everyone disagrees on what the temperature between the 37.5 and 37.9 means. And then I think most people would agree that from 38 onwards, that is a fever or a raised temperature.Emma: One of the things that interests me, and I think people don't think about this enough, is that you can be really sick with a bad infection and no fever. And you can also have a very high fever and not really be that unwell.
Alasdair: Yeah, I think there's a lot of stuff about fevers that intuitively we feel should be true. And then when you look at the data, actually, it's not true. So, things like if the fever is really high, as you said, this must be a sign that the child is more ill. And actually, the predictive value of the higher the temperature is so poor as to be almost useless.
Emma: So Alasdair, that's such an important point. We always get parents coming in saying, ‘my child had a fever, they must be really ill.’ And you're telling me there is no good evidence linking high temperatures to an increased risk of a serious bacterial infection or any other serious infection?
Alasdair: That's right. We talk about these things having a predictive value, so how likely is a really high temperature to predict a serious infection, and outside of children who are really high risk of having a serious illness like those with immunodeficiency, in otherwise healthy children the higher the temperature is basically of no value. So once they've crossed the threshold for a fever, it's a fever, how high it was is not really that important. As much as it feels like it should be to parents and often to doctors as well.
Christo: So knowing that the height or the grade of a fever doesn't necessarily predict the likelihood of serious illness. Are there any physiological changes that go along with this that we might see in clinical practice?
Alasdair: Yes, there are. So, we know that the height of a temperature is correlated to the change in heart rate, in particular. We always used to think it was respiratory rate too, some degree that's probably true, but actually the most up to date evidence would suggest respiratory rate is much less affected by the height of the fever, but heart rate certainly. Now of course, this is the cause of a huge amount of anxiety and time spent, particularly in the emergency department. Because one of the things we always say we like to see is that temperature when it does normalise or comes down, that the heart rate starts following it down too. So of course we're all on the lookout for abnormal heart rates and things because they're all over our sepsis tools, as another trigger warning tool. But because we know it can be normal, it makes it really difficult in clinical practice for paediatricians to try and make sure people feel reassured and the documentation obviously looks complete and that you've done all the right things to check it all out.
Christo: I think this is a really interesting paradox that we know that fever changes your physiological observations. We are happy with the idea that response to fever to antipyretic doesn't necessarily predict how serious the illnesses is. Yet, we do feel uncomfortable seeing a child with a heart rate of 160, who is febrile who otherwise looks well, and discharging them from the emergency department without a longer period of observation or seeing those observation normalise. I think it's one of those kinds of big problems, and Emma has previously talked about trying to identify sepsis being like looking for needles in a haystack. And I think this kind of epitomises that.
Alasdair: Yeah, it does. And I guess the problem is, is that a lot of it does come back to where there's been bad outcomes for children, very often there'll be this retrospective look back and it's combing through all the details to see anything that could have picked up that the child was ill. And because the abnormal heart rate is so common, it very commonly gets picked up in these retrospective reviews and then gets implemented as a learning point. And people really feel like they can’t discharge children with abnormal heart rate, in case this is the one in a million children who does end up coming back very seriously unwell, which could not be detected at that first point. But this is one of the concerns that weighs very heavily on health care providers, particularly in paediatrics.
Emma: I am burning, burning issues with all these normal values. I'm getting I'm going to get it all out now!
First of all, one of my issues is that a lot of paediatric normal values were based on very small populations, so the original data. And we have a lot of new data with electronic observations, but it hasn't yet been incorporated into practice. So that's number one.
Number two, I think you're completely right about people looking at all the children who got very sick and then looking back and saying that's the problem. Actually, we should be looking at all the children who well, So there was a really good study by Winter, who looked at 33,000 children that were discharged with abnormal and normal paediatric early warning scores. Very few, it was like less than 1%, had any abnormal outcomes. So, the majority of children are safe to send home. That is the message that people need to know. If you have a fever, you get checked over and the parents are happy and reassured, you're more or less safe to send them home.Alasdair: I agree, and I think it's one of the things that we struggle with isn't it. We all know that that's true, and in practice, it's so frustrating feeling like you can't do that, because were someone to look back they won't see all the other children who went home. They don't see how the heart rate is in normal in every child you see and the difficulty is that that makes sense to manage a busy department.
Christo: Yes, so I think you mentioned earlier that there are some special patient groups outside of the general paediatric population, where actually the presence of fever or even the grade of fever, might put you in different risk categories. Would you like to talk us through some of those?
Alasdair: I think that it's really important because I think actually, when you're managing a children's assessment unit or an emergency department, we spend a whole lot of time looking at different physiological parameters to try and risk assess children. But actually, we know that there are risk categories, the risk associated with them absolutely obliviates any of these other factors, by orders of magnitude, you should be more concerned about children who fall into these categories than any of the children with abnormal heart rates or respiratory rates, because they are at so much more increased risk. So it all essentially comes down to some issue with immunity, either an immature immune system, or a breach in the normal immune system, or actual innate or acquired immune deficiencies. So things like neonates, we know they have very immature immune systems. They are the most dangerous time of your whole life through an invasive infections, within the first few days or weeks. And so we all know you never trust a neonate, that's probably one of the most important groups.
Then there's children who may have breaches to normal immune system, so a central line in situ, for whatever reason, is a breach of the normal protection to your bloodstream from bacteria because there's now a line in from the outside world and so we always have to be cautious with them. And then there are children who have their immune system, their immune cells are not functioning as they should be, either because they were born with a problem with their immune system or they've acquired a disease that suppresses their immune system, particularly some of the oncology patients, or they're on treatments which suppress their immune system. So, the children who have inflammatory diseases, where there are medicines that suppress that it also suppresses the normal function of your immune system. Children who are a long time on long term steroids, these kinds of things. And these are the children that even if they have normal physiological parameters, we should be thinking much, much more carefully.Emma: Thank you, Alastair, I think it's really important. That brings me down to one of my favourite things to say, it's all in the history. Most of what you'll find is in the history, and your examination is actually only going to back up that history. A good history is what you need. So are you in a high risk population? Are you immune suppressed? Do you have a line? Are you on medication that suppresses you? Have you've got chemotherapy? Have you got an autoimmune problem? Are you a rheumatology patient? I think we so often think about steroids, we often miss children like those with inflammatory bowel disease and don't recognise them as functionally immunosuppressed.
Christo: And I think this brings up another challenge assessing children with autoimmune or inflammatory disease who present with fever, and that's determining what is due to infection because of their impaired immunity, versus what is due to their underlying disease. And whether this is a breakthrough of their arthritis, or if they're about to have a flare of their colitis, for example, I think that's really challenging.
Emma: Which is a really important point because I think we get really focused on infection, but there are multiple causes of fever. What are the other common causes of fever that get overlooked?
Alasdair: What I would say is I don't think there are any other common causes of fever. There are there are other causes of fever there, but they're all relatively uncommon and obviously because they're not related to infection they are less interesting, sorry, to all of the non-infection specialists out there, but that is the truth! They are most commonly probably inflammatory conditions, so auto inflammatory conditions. And I guess the one that paediatricians think most about would be Kawasaki disease, that we are hopefully thinking about in any child who have a fever or five days or more duration. But then there are other kind of rheumatological diseases that can present with fevers, and obviously one of the other ones with a persistent fever not to miss is malignancy. And this can very often be one of the presenting features of that. So I think those are the big three to think of. So, it’s infection, infection, infection, infection, and then also autoinflammatory and haematological malignancies. Those are the big three.
Emma: While we're talking about the causes of fever, the other thing that I think people get really hung up on is how long the fever lasts. So apart from coming in and saying my child was better 40, lots of people come into me and say the fever still there after five days.
Alasdair: I think there's probably two reasons for that. So one is the all of the bottles of paracetamol and ibuprofen liquid say on them don't give for more than three days. And so after three days of giving their children paracetamol and ibuprofen, parents think that they need to see a doctor no matter how well their child is, which is obviously not true.
And then the other thing is, this magic five day cut off that paediatricians try and drill home. And that's purely because that's the point at which we want to make sure that the child has an infection and doesn't have something like Kawasaki disease, and we want to roll that out. And that's because we know that early treatment really improves the prognosis of that condition, so we want to catch it early.I think what's really worth bearing in mind however, is that there's not really a well characterised normal duration of fever for sort of benign childhood viral infections. You know, a lot of them will resolve in two to three days, but we see plenty of normal coughs and colds where the fever will go on for five, seven days, sometimes even longer. And we do end up investigating these children once it's gone on for quite a prolonged period of time, but often for children with a very clear source, who are well as long, as you're providing good safety netting advice, even a fever of a duration of five to seven days doesn't necessarily need anything special being done. Because we know that this is just normal or, you know, a non-insignificant portion of children with these illnesses.
Emma: I couldn't agree more. I think things like RSV (respiratory syncytial virus) and influenza, they really drag on and people forget, and they think why this like a normal cold is so they tend to worry. The only time that I really worry is when a child's got better and then worse again, so the classic time is catching chickenpox, having a bit of a fever, fever goes away, child gets better, child then develops a second fever and I do worry about those secondary bacterial infections after a serious viral infection. So classically, chickenpox, occasionally flu, and we've seen it with COVID.
Alasdair: Yeah, that's a really good point, and it's one of the things I've started saying more often, in the past few months, actually, to parents as part of my safety netting advice because we do see quite a lot of these reattendances when the clinical picture hasn't changed. And so what I'm trying to reassure parents more these days is, within a period of a few days, if child hasn't improved much, that's not necessarily a concern. We know that it does take a while for kids to get better from these, so staying the same is not so bad. Deterioration is when we become concerned, so if they're getting worse, that's a much better sign that you should be bringing your child back to be reviewed again. But staying the same for a while can be just normal.
Emma: It’s the one question I always ask parents, I often ask parents, what is it about this illness that is different to previous illnesses that made you come? Or in what way has your child changed or differed?
Christo: At this point is probably worth highlighting, and I think it's something that we could all do with communicating to parents and families that we see presenting with a child with a viral illness, that there is a normal number of viral illnesses that your average child under five might have in a year.
And this might vary, but the number of normal episodes can be quite high. And I think there's often a mismatch between what we see as a normal number of illnesses in a given winter or in a given year, and what parents feel should be normal.Emma: I always tell parents that you can have 10 to 12 viral illnesses a year. Now say, you don't get one or two in the summer, that's absolutely one a month or more, so you'll be ill for two weeks, well for a week and then you're on to your second one. In real terms, if you've ever had a child that's snotty the whole entire winter with intermittent fevers, and that's normal and that's important. And that's part of maturing your immune system. So it's a good thing, not a bad thing.
Alasdair: Yeah, and I guess that's one of the things that we often see these children who get brought in and they don't look very unwell and the parents will say, you know, he’s not that sick, but he's been ill so many times there's got to be something else ging on, this is like the fourth cough. And then this is the conversation that sometimes take a little bit longer, to just try and break down the fact that, particularly really young preschool aged children, this is unfortunately par for the course, particularly if they're in nursery or preschool, or they've got an older sibling in nursery or preschool or, in the early years of school. This is where all of these bugs come home and where they get encountered for the first time. And so your body is just learning how to recognise them and respond to them, and unfortunately, that means feeling a bit poorly, for pretty much a whole winter for a while.
Emma: But actually there's a positive side to that, because if you meet these viral infections when you're young, so take the example of EBV Epstein-Barr virus, it will be a minor viral illness you’ll never notice. If you live in a nice, middle class, very clean house, don't socialise with other children and you only meet EBV you're a teenager you're in for a much more serious, prolonged illness. So I do say to parents, although they're ill, actually this is what you want. This is part of building up your immunity and meeting viral illnesses at a young age is important, and it's positive.
Alasdair: I guess the sad truth of life is that there's a very large number of viruses for which infection is ubiquitous, there's no avoiding it. Almost everyone is going to encounter it, at some point. And for a lot of those, your body is really designed to encounter them for the first time in those early years.
That's what we're adapted to, because that is the normal experience, that is when you're normally coming to terms with them for the first time so your immune system is geared up for that. And that does mean that a lot of them, you will experience a much more minor course in that very early period of life rather than later on. The really classic example is chicken pox that we all know, get it when you're really young, generally pretty mild and as a you know, a teenager or adult it's pretty, pretty horrendous. It's just the way we've adapted to be sadly!Emma: Well controversially, we could be like America and Australia and vaccinate for chickenpox, but I don't want to stir up more controversy in this podcast.
Alasdair: We should definitely vaccinate for chickenpox, I'll just put it out there. We should just get on and do it.
Emma: So, we've talked about what fever it is. We've talked about what's normal. We've talked about high fevers not being a problem. We've talked about the length of fevers and having lots of infections over a winter as also being normal. But what about pyrexia of unknown origin (PUO)? At what point can they call something a PUO?
Alasdair: It's two weeks Emma, as I'm sure we all know, it’s two weeks obviously.
What I guess important is to remember, I'm not very pedantic about a lot of things but PUO is one of the things I am a little bit pedantic about, because when we see children who have been febrile for a few days, who present and there's no clear source of the fever, they will often be labelled as a PUO. But it's not a PUO, that has quite a specific meaning in medical terminology, and it refers to a prolonged fever, longer than two weeks of duration that has no clear source. And it's important, because for normal children coming into primary care with a brief history of fever, with no clear source, it will almost always be infectious in origin, over 99% the time. For a PUO, and that prolonged duration of fever with no clear source, actually infection is still on the list, but you need to really be thinking about other conditions because it's very unusual for an infectious fever to last that long. And so that's when it does prompt, much more detailed investigation, and you really need to be confident of the source of that fever before you can move on and do anything else.Christo: And it's probably worth highlighting that true PUO Isn't that common. Certainly, in comparison to the number of children, like you described, that have a fever without an obvious source for three or four days. These aren't patients that you should be seeing every day, or even necessarily every week, depending on how big your catchment areas.
Emma: I'm just saying that PUO is a child with a fever and no upper respiratory tract symptoms, o not a cough and a fever, not a snotty nose and a fever. It's just that the fever.
I think this brings us along to a really interesting question because you said to us, if you have a prolonged fever you need some investigation. Now I read that is if you have a normal fever, you do not need much investigation. What do you have to say about that?Alasdair: I'd say I'd largely agree with that. I have my own sort of internal framework for managing fever, because it's by far and away the most common thing we see in paediatric acute paediatrics. It's really useful to have that kind of framework so you can very quickly move through your assessments and do it in a consistent way.
So, obviously, the first question with any child with a fever is do they need resuscitation? Most of the time? It's no. So that's an easy point to move past. And then the next question is, is there a clear source? If there's a clear source then you very rarely need any investigation because you just manage the source as it needs managing and most of the time, that is no treatment. Then for a small proportion of the time that will may be bacterial infection like pneumonia or a urinary tract infection, and the overwhelming majority of those can be managed with oral antibiotics. And sometimes you may want to use IV antibiotics for children who are very severely ill.
And then if there's no source, the next question is, are there any red flags? So, we will see actually quite a lot of children who have a brief history of fever with no clear source, and then you're going to be looking for things in the history or on your examination that are signals that this is more than a benign childhood viral infection. So that's things like the child appearing more unwell than they should, not responding, being lethargic or floppy, very poor urine output or fluid intake and these kinds of things. And if there's red flags, that's the time at which you need to do investigation, because now you're wondering, is there something more than a normal, benign childhood virus here that would need a treatment? And the question that's really on our mind is, could this be an invasive infection like a bacteraemia? That's the question you really want to answer with your investigations.Emma: The problem about the red flags is we know that if you look at the nice red flags, I think they did a nice study in Liverpool and they showed when they looked at 20 and 30,000 children that half have red flags, straight off. You're in a really difficult position because half that’s fine, you can send them home, you've still got half children with a fever, but we know that about 10% of the children are likely to have serious bacterial infections when they present to the emergency department and the red flags have only chopped that in half. Now we don’t want to investigate too many and I think the bit that everybody struggles in is who gets blood test, and which blood tests do you do on these children who probably have viral infections.
Alasdair: Everyone does struggle with that, you're right. What I would say is that there's a difficult trade off here between expediency and invasiveness of your management, I think. So one of the famous paediatric sayings is ‘the observation is the best investigation’. And quite often these red flags, like abnormal physiological parameters or the child behaving unusually, it can just be due to having a fever at the time. And once you've given them a little while to have an antipyretic and to drink an hour or two later, they'll look completely different. And anyone who's worked in acute paediatrics will know, you can go from having a child who you're wondering if you should move them round to Resus, to jumping on the bed eating, a packet of crisps and singing, within the space of like an hour or two, just because the fever resolves. So I always think if you're not sure, if the child is stable, it is fine to just wait a little while because if you do blood tests and you weren't sure if you should do blood tests, you will quite often end up being unhappy that you did a blood test. Because your inflammatory
markers may well be in a zone where they don't rule anything out and they don't make anything likely enough to really make you feel compelled to act. And that is a really difficult position, I'm sure we've all been in more than once.Emma: I couldn't agree more. And I think you need to remember the new sepsis international consensus guidelines say that you only need to do investigations and treat within an hour if you're shocked, and very few children we see are shocked, most of them are febrile. And in those febrile children you've got three hours, so that is long enough to give them paracetamol, ibuprofen, and a drink, and wait because watchful waiting, as my grandmother and you say, is the most invaluable thing, or masterly inactivity.
Christo: I think you've mentioned there Alasdair about the amazing recovery some children can make with just some antipyretics. Are there any downsides to treating fever in an otherwise relatively well child has no risk factors and most probably has a viral upper respiratory tract infection?
Emma: Okay, so Alasdair I'm a bit hardline about this, because I think that having a fever is a good thing. I mean, it's the body's way of trying to get rid of viruses. So, I tell parents they should only give their children paracetamol and ibuprofen if they look miserable, or they're clearly in pain. They do not need to keep giving paracetamol and ibuprofen just because they have a temperature, if they're running around and looking fine. What's your view on this?
Alasdair: I'm sure it will come as no surprise to you Emma that I completely agree. I think you're completely right. And I guess the reason is to understand what why are we treating fevers? The reason is not because the fever is a danger to the child, so having a high temperature poses no risk for the childhood at all. It's a function of your body trying to help you clear the infection. So why do we treat it? Well, we treat it because actually, as one of the side effects of a fever, you feel dreadful, quite often you feel terrible. And actually, this is another adaptive mechanism of fevers, you're supposed to feel terrible so you go and lie down and you don't go and infect your tribe members or your members of your household or whatever. So it's supposed to make you antisocial. But we don't we don't like children feeling awful, and so we know that there's something quite effective we can do to try and help them feel better, so we can give them medicines like paracetamol, ibuprofen, which are quite effective at switching off that internal mechanism driving the high temperature and can make you feel more comfortable.
Emma: Now, interestingly, we use paracetamol and ibuprofen a lot in this country. But my German friends think we're absolutely crazy because they never use ibuprofen in Germany and they think it's a very, very dangerous drug.
So are there contraindications for using ibuprofen?Alasdair: If you have certain platelet problems or clotting abnormalities, you might be told to avoid ibuprofen or similarly, children who have a history of gastric ulceration or very severe gastroesophageal reflux disease might I'd avoid it.
But the one that gets talked about probably the most is chickenpox as a reason to avoid ibuprofen, this is somewhat controversial I must say. The recommendation is based on some quite old observational evidence that found children with chickenpox who went on to develop necrotizing fasciitis, a flesh-eating bacterial disease, as an adverse effect of the chicken pox, they were more likely to have been given ibuprofen earlier in their illness than children with chickenpox who didn't get necrotizing fasciitis. Now, what’s not clear is whether children who got necrotizing fasciitis looked more sick, and so were more likely to have been given ibuprofen rather than being given ibuprofen made them more likely to get necrotizing fasciitis. So, it's what is the cause and effect of that association? It isn't clear. And so because there is an alternative to ibuprofen that isn't associated with this risk, the advice has just been to avoid ibuprofen because there's a safe alternative, so why do you need it?
In practice, we, as healthcare providers will sometimes see children who have chickenpox whose symptoms are not well controlled with paracetamol. And I think it's perfectly acceptable to give children ibuprofen in that setting to try and relieve their symptoms because if there is an increased risk, the absolute risk is really, really small. Very, very, very, very small. And I think most people would agree, it’s easily outweighed by the symptomatic benefit of giving a briefing to children whose symptoms wouldn't otherwise be well controlled.Emma: Great, so paracetamol is absolutely everybody. Ibuprofen cautiously in anybody with clotting disorders, gastric problems, asthma occasionally, chicken box give it with caution.
Christo: What causes fever in a physiological sense?
Alasdair: So a fever is a normal physiological reaction to an infection. So, this is something that's conserved across all sorts of animal species. So even cold-blooded animals will go and lie in the sun to make themselves hotter than they would normally be, to try and drive their body temperature up when they sense an infection. So you see this across all hosts of animals. And it's triggered by chemicals that are called pyrogens, and these can either be endogenous, the chemicals you make yourself like cytokines, and things that you would make in response to your body noticing an invader, or sometimes elements of the infection themselves can be pyrogens, things like the lipopolysaccharides membrane on the outside of Gram-negative bacteria. And when your body recognises these chemicals, your hypothalamus sets a new higher target temperature. So, the part of your brain that controls normality says right, we need normal to be higher. And so, your body then sets about doing all the normal things that would do to try and make you warmer, so it makes your hair stand on end, it sends blood away from your fingers and toes and into your core, it makes you feel cold so you go and do things to warm yourself up, by putting on a blanket and going somewhere warm. And the reason it happens is actually not that obvious. It's not very well defined, precisely the effect that fever has that's beneficial, but it appears to slow down the growth of viruses and bacteria, so it helps stop them going so quickly. And it also seems to activate different parts of your immune system to help them respond.
So, I always say to parents, fever is something your body is doing to the infection, not something an infection is doing to your body. So, it's the body's way of trying to help and the reason why that's useful to know, is it takes some of that fear away because people are often very scared that their child is going to come to harm as a result of the high temperature. And once you let people know that your body is in control, it's doing it to benefit you, it's something healthy that's happening, that can help take the edge away of some of that fear that the child is going to come to harm because their temperature is too high.Emma: I think that is the crux of this whole podcast. That fever makes parents scared, they fear fever. Fever is part of the normal adaptive response, and we should all embrace fevers and recognise that it is normal.
Alasdair: Absolutely, sign of a well functioning immune system.
Emma: And the flip side to that is that parents need to recognise deterioration in their child and know what a sick child looks like. And that's not just a fever, that's a whole host of things.
Christo: To follow on from that, Emma. It's also worth pointing out to parents that sometimes absence of fever doesn't mean that there is no risk. So, thinking particularly about neonates and immunosuppressed patients who might be normothermic or even hypothermic in response to even significant invasive infection, or patients who are on immunosuppression, who might have the same inflammatory response. And it's sometimes easy to give the wrong message that not all fevers are bad, but absence of fever is a good thing. Whereas if your child looks unwell and you're worried and you think they're deteriorating, then not being febrile shouldn't be a reason to not seek advice.
Alasdair: One of the things that I say to parents as part of my home fever spiel is that the fever itself is not really of interest to us as doctors so that a fever is just one of the many symptoms of an infection. So, when we know that you have a fever, we just know there is likely an infection somewhere. The fever then is not that interesting. What we want to know is what is the infection and is it an infection that can be treated or that poses a serious risk to the child. But although so much attention goes on fevers, and actually the relevance of a fever is not that much once it's told you there's an infection present, it is the infection that needs the attention.
What I try to do is the best summation of you, what is normal sick, what is sick sick? I as parents try and remember the last time you had like a nasty flu like illness, and remember how you felt and how you behaved, and you just wanted to go to bed and sleep all day, you weren't interested in foods, you might drink a little bit, but if someone came to try and wake you up, it wouldn't be difficult to wake you up. And you know, you were still able to force a little bit of food and drink down if you knew you had to, and you didn't have any of difficulty breathing or those kinds of things. And that's I hope is a useful shortcut for parents to try and think well, if my child is sick, they're going to look like that, because they're sick so they'll look like sick. But what is sick enough, or you know what is out of the ordinary and needs additional medical attention? So trying to put that in a in a frame of reference from their own experiences I hope it's helpful.Emma: I think that's what we call the Mars bar or £20 note tests. So you say, Would you like a Mars bar? Would you go and pick up a Mars bar? Would you pick up that £20 note? If you're so sick that you wouldn't go pick up the £20 note, or if the child says, ‘no, I don't even want to Mars bar’ that's when I worry.
Christo: Alasdair, do you think this frame of reference that we're talking about has changed at all over the past three years? And we ask this in January 2023, after three years almost living with COVID and it going from pandemic to endemic, and the recent fear about group A strep. Do you think our frame of reference and parents frame of reference about what normal is for infections has changed?
Alasdair: I think that's a really good question. And I think I don't really get a good sense to be honest as to how it's changed at a population level. I think it's very different for individuals. So certainly, it's been a very traumatic few years for a lot of people and I think health anxiety will be a real problem for some families, certainly. And understandably so. I think, perhaps, for want of a better word, the normalisation of COVID and the discussion around the symptoms you could have with it, people are coming to terms with the fact that it is now a normal part of life and to expect that people will catch that infection and they will have these symptoms and then they will go away and that's okay. Maybe for some people this may help normalise viral or respiratory infections as a sort of a fact of life. So I think, it could sort of go one of two ways for different people as for how that's averaged out, and how many people may have been pushed one way or the other? I'm not sure.
Emma: I think your point about health anxiety is really important. I think people are worried and anxious. And I think that's on the backgrounds of during lockdown, children didn't see other children. They didn't go to school, and they didn't get any infections, so for a year they appeared well, and then of course when they finally got back to school, they got all the infections they missed, and they seem to be a bit more unwell and that was a nasty shock to everybody.
One of my take homes is that people forgot what viral infections look like. The other is, everybody washed their hands in COVID and infections went down. And I'm just saying hand washing is a very good thing, probably more important than all those antibiotics unnecessarily get!Alasdair: Washing is very, very underrated, very underrated. We're going to make hand washing great again. Make hand washing great again! That's my new motto. You'll see it on my hats I'll be wearing in the future.
Emma: At the end, we always give everybody the chance to give us their three top tips. What are yours?
Alasdair: Number one, a fever without a source doesn't need investigation if the child is otherwise well, and there's no red flag signs.
Number two, fever is a normal physiological response to an infection. And that if you're able to explain that to parents, you will change their whole perception of febrile illnesses in their child going forwards. So, it's a really worthwhile investment on that first encounter.
And I think my third one is that observation is really a wonderful investigation for febrile children because it is normal for children to look quite dreadful whilst they're febrile. And if you're concerned, sometimes just a little bit of time, allowing that fever to come down and the child can honestly look like a completely different child and save you the hassle of the investigations and all those other things.
So, I think those are my top three.Emma: I’m just going to take you to task with number one. So the child that looks well has a fever, do they need a urine culture? Or not?
Alasdair: Most of the time, they don't in my opinion. though, there will be some, any child under three months, I would always do it. Under six months with no clear source is probably wise. And then from that point onwards you can sort of risk stratify based on how long they've been febrile, and also if it's a boy or a girl. So, older boys sort of over the age of two with no history of urine infection, the likelihood of picking up a first UTI it gets progressively lower and lower and lower, especially without any urinary symptoms. So, think twice before, reflexively requesting that urine sample that is going to come back contaminated.
Emma: Now we're in complete agreement. And in my books, anybody who's got a runny nose does not get a urine sample because it’s the runny nose causing the fever.
Christo: There's also something about the way in which you collect your urine sample. The common approach of sticking a piece of cotton wool in a nappy to fester for four hours, and then our surprise when it grows, staph epi or some other skin commensals, that really needs to stop.
Alasdair: I think I'm going to try really hard not to go off on a rant here. But please, please don't ever put a urine bag on a child. That's all I'll say about it. And I'll just draw a line under it there. Never put a urine bag on a child. That's the end.
Emma: I wanted to say, clean catch only.
Alasdair: Or catheter in a little baby. You could do a catheter, some people would still do SPAs (suprapubic aspiration). Wild people, I'm not sure why they're still doing that.
Emma: So, SPAs, suprapubic aspirations, were a great thing when I was a junior doctor. I actually loved it because you could do your sepsis screen super quick because you do blood, Lp (lipoprotein) quickly, stab the bladder with a clean needle, an aspirate. Now obviously this was A) very invasive and B) a number of my friends got gastric contents, and you did wonder about the safety of this.
Fortunately, those days have passed, SPAs are dead to us now, unless you have ultrasound guidance and a very good reason to do it.Christo: I think particularly in the face of things like the patented quick wee methods. I don’t know if you’re familiar with this. There was a great paper that was in archives a few years ago looking at basically if you get some cold water on some cotton wool and rub the tummy, it's likely to encourage urination in a very high proportion of infants, so great for those sceptic work ups.
Alasdair: Just speaking from my own experience, I did do it a few times and the looks the parents gave me put me off doing it again! I’ve only done a couple of quick wees as the parents stared on at me in complete disbelief. Here's the weird doctor, just got to get the wet cotton wool, stroking their child's lower abdomen with it!
Emma: I think it's been a great pleasure to talk to you Alasdair. It’s been really fun. I love your top tips. I think that you have really reassured us, and I think that listening to this, having these facts at your fingertips means that we can reassure parents that in the majority of cases fever is not something to fear.
Alasdair: Thank you so much for having me.
[music]
This podcast is a collaboration between Odland, medical education and the Royal College of Paediatrics and Child Health. You can find more creative learning resources and a wealth of information on the important work of RCPCH on www.rcpch.ac.uk or #ChoosePaediatrics.
[music ends]
Emma: The views, thoughts and opinions expressed in this podcast relates only to the speaker and not necessarily to their employer, organisation, the Royal College of Paediatrics and Child Health, or any other group or individual.
-
EPISODE 5: Having a GAS – Group A Strep (released 05 March 2024)
This month on The Paeds Round, Emma and Christo are joined by Dr Liz Whittaker, a paediatric infectious diseases consultant in London, an academic at Imperial College and convener of the British Paediatric Allergy, Immunity and Infection Group (BPAIIG) to discuss the bacteria, group A Streptococcus.
They get into questions such as what is Group A Strep and what are its carriage rates? How do we pick apart those with just viral illnesses from those with strep throat? Whether or not to use antibiotics, rashes and much more. So please download and listen to the latest instalment of the podcast.
[music, with snippets]
Liz: Common things are common. And you get to recognise things that are uncommon
and need different attention, so seeing lots of children with viral infections while is
annoying at three o'clock in the morning, makes you a better doctor.
Christo: It's not a case of not wanting to prescribe antibiotics. It's about wanting to do the
best thing for the child in front of us.
Emma: Part of what we do in medicine is explain and reassure, that is actually harder
than giving out pills or giving out medicine. And that is the art of being a paediatrician.
[music ends]
Emma: Hello, everyone, and welcome to The Paeds Round, your regular podcast from the
Royal College of Paediatrics and Child Health. My name is Emma Lim, I'm a consultant
paediatrician at the Great North Children's Hospital in Newcastle upon Tyne. Together
with our guests, we'll dive into some of the hottest issues affecting our specialty. We'll try
and bring you insights from paediatric experts and round up some of the key learning
points for your practice along the way. So, let's get started with our Paeds Round!
It's the beginning of the new year, and I thought it would be really interesting to talk
about one of my favourite bacteria, group A streptococcus. And so to help me because we
always need help from experts. I have Liz Whittaker here to talk to us.
Liz: So I am Liz Whittaker. I'm a paediatric infectious diseases consultant in London and
an academic at Imperial College, and I am the convener of the British Paediatric Allergy,
Immunity and Infection Group (BPAIIG), which is why I ended up talking at a lot of these
things.
Emma: Liz is one of my ‘phone a friend’ people, so when I’m horribly stuck, she’s one of
the people who is A very nice, and B knows all the answers.
Liz: I actually know all the people who know the answers, I think that's the key.
Emma: I also have my sidekick to keep me on the straight and narrow, Christo.
Christo: Morning. My name is Christo, I'm a research fellow in Newcastle working with
Emma currently doing a PhD in paediatric immunology.
Emma: So, let's dive straight in. One of the things that I always think about with bacteria,
people seem to think that bacteria are bad, but actually bacteria live on our skin and in
our throat all the time and don't really cause as many problems. So, what I'm really talking
about is commensals. Liz, can you talk a bit about group A streptococcus, what it is and
carriage rates.
Liz: Group A streptococcus is a member of the Streptococcaceae family, and we learnt
about this in med school, and I remember spending a lot of time on streptococcal and
staphylococcal bacteria in microbiology. And I've got to be honest, at the time, it didn't
make any sense. But subsequently, both as a junior doctor and then as a consultant, I've
realised how important both of these wonderful pathogens are. So, they're not just
pathogens, we are covered in bacteria. It's really important for our immune tolerance and
our development of our T cell responses and our ability to recognise foreign from not, and
in particular, our pathogen recognition receptors. And so, we are covered from head to
toe in not just by bacteria, but also viruses as well. We have a biome and microbiome,
which is both bacteria and viruses, and carriage rates are surprisingly high. So, we have
this problem, and this is one of the reasons why diagnostics become slightly challenging,
particularly in this context, is that many people carry streptococcal bacteria at the back of
their throat without causing them any harm at all. And so it's really difficult to say just
because you found something on a throat swab or in a rapid test, that it's causing a
problem. You have to take it in the context of how the child is clinically presenting as well.
Emma: Thank you. I mean, I think that says it all so clearly, that lots of people have strep,
but it only causes disease in some people. And even those people that might cause minor
disease and very, very few get seriously ill.
Christo: Liz, is this why rapid antigen testing isn't recommended by NICE (The National
Institute for Health and Care Excellence)?
Liz: This is almost exactly why rapid antigen testing hasn't been adopted in our setting.
And it's interesting, lot of people say ‘Oh, but it's used all across the United States and
Canada and Germany’. They have a very different healthcare system structure as well
though and they are used in the context of clinical scoring systems and not just as a tool
by themselves. But we know that if you treated every child who had a positive rapid
antigen test with antibiotics, you'd probably be overtreating by between 90 and 95% of
those children. And that's a lot of antibiotic that's not needed. So, we should try and avoid
that.
Emma: Absolutely, they are my favourite words, ‘avoid antibiotics’. Let's say we have
people where bacteria just sit on their throats and they don't do anything, but we see a lot
of children with sore throats. That is a really common presentation. So how do we pick
apart those with just viral illnesses from those with strep throat?
Liz: That's such a good question, and there are a number of scoring systems that have
been developed and really validated in adults, if we're honest, with some data in children.
So the Centor scoring system with a feverPAIN scoring system are the ones that we use,
and usually in children over the age of three. But as a general rule, if they're full of snot,
and they're coughing and spluttering, classic virally looking rash, and they've got a sore
throat with that, that's probably going to be a viral infection. This is where, as you get
more senior it's easier, you learn to trust what you know. And this is why we make you go
to A&E to see lots of patients, because common things are common, and you get to
recognise things that are uncommon and need different attention. So, seeing lots of
children with viral affection for us annoying at three o'clock in the morning, makes you a
better doctor.
Christo: Those scoring systems that you've mentioned Liz are really helpful for trying to
pick apart viral versus bacterial tonsillitis and sore throat, but do you think every bacterial
or likely bacterial tonsillitis requires antibiotics?
Liz: That is such a good question and no, I don't think they do. The vast majority of
tonsillitis is self-limiting. There is lovely evidence showing that antibiotics might reduce
your symptoms by maybe a day, but not much more than that. And actually, when we go
back to that immune question before, having repeated episodes does help you to develop
protective immunity against some of these infections, provided they stay mild and allow
your immune system to develop the way that it should. Because although we don't have
a vaccine against group A strep, and so protective immunity is a little bit elusive, we don't
continue seeing tonsillitis and group A strep infections throughout childhood. At some
point people develop the right kind of immunity that stops them from getting ongoing
tonsillitis.
Emma: I think that's so important. I'm always saying to parents, when they bring us snotty
children, there is a plus side to this. This is going to help your child develop a good
immune system. And I think that's really vital.
Going back to talking about antibiotics, number one we just shouldn't prescribe. Number
two, even if we do prescribe them, as you said, it might only shorten the course of the
illness, not even do it much else. But I think it's really important to think how we give
antibiotics. You know, we're a big fan of pill swallowing. And I'm very keen that people
don't give 10 days of oral penicillin. Have you tried giving oral penicillin four times a day to
a struggling toddler? And there are lots of other better options.
Liz: Absolutely, I couldn't agree more. I think there's a great opportunity here whilst the
stage is looking at antibiotics, to do a bit of education for parents in particular, but also
those who work in primary care and in frontline settings who prescribe the bulk of this
kind of antibiotics, to say that we should be encouraging children from the age of five,
maybe younger, if they’re on it, and to try and swallow pills. I have to confess, my children
have been very lucky and haven’t had many illnesses in their life and I taught my nine
year old to swallow Tic Tacs over Christmas because I was so embarrassed that it had
never come up before! But I realised that it just hadn’t been on my agenda of things that
we need to do, we need to make that part of parenting, that actually over time you teach
them to ride a bike, you need to teach them to swallow a tablet, it’s part of growing up.
Christo: On the topic of antibiotics. What are the kind of good alternatives to penicillin
be?
Liz: One of the things that was extraordinary in December of this year (2022) was the big
media coverage of antibiotic shortages, which I think was very alarming for both parents
and clinicians. And a rapid protocol was developed to allow pharmacists to give good
alternatives. So actually, I was involved in some of those meetings. We've talked about this
a lot. So first line recommendations are amoxicillin, very palatable for children and
penicillin. After that, the other options are things like macrolides, although we have to
remember there's between 8-11% resistance to streptococcal infections from macrolides
and that is from azithromycin and clarithromycin, augmentin, but again, it's quite broad
spectrum and is more associated with GI (gastrointestinal system) side effects so that
wouldn't be top of our list. And we have Keflex, very underused antibiotic but actually very
effective and quite palatable. And then we have things like Septrin which was what we
got when I was a child, and but kind of has gone out of vogue a little bit but is a really
good alternative as well. And so I think there are lots of options. Currently until things
change, you can just write penicillin on the prescription and your amazing pharmacist will
choose an option if they do not have what you want available for them, including
probably Amoxil quite high up there.
Emma: And this is one of my huge bugbears, is that people don't understand when they
get antibiotics, antibiotics have side effects. And you mentioned GI, gastrointestinal side
effects, so when you have an antibiotic, it doesn't just kill the bacteria in your throat, it kills
all the healthy bacteria in your gut and you get a bit of diarrhoea, it does not mean that
you are allergic to that antibiotic. All medicines have side effects and that's why they
should only be prescribed with caution.
Christo: I think this is really important to communicate across to parents and families
when we're counselling them and safety netting, that it's not a case of not wanting to
prescribe antibiotics. It's about wanting to do the best thing for the child in front of us.
And if the potential side effects are going to cause more distress, and add, say diarrhoea
on top of a child who's snotty and miserable, then foregoing antibiotics might be the
better choice for that child. It's just sometimes difficult to be able to communicate that
when you’ve got parents who are stressed or tired, and you're busy in the GP surgery or in
A&E.
Liz: And they just want their child to get better, Christo. So yeah, I think I'm slightly
worried that with all these children with viral infections who are given antibiotic,s that
they will go through the normal history of a viral infection and develop a maculopapular
rash, which is self-limiting, but that that will be labelled as an allergy. And what I also
think that as clinicians both in primary care, but also in A&E, that we can say to parents
that doesn't look like an allergy so they don't get labelled as having an allergy for the
future.
I also think that the important thing about not giving antibiotics is to give parents the
decision-making ability about when to come back, because although the vast, vast, vast,
vast majority of these children will get better and not need more medical attention, a
teeny tiny subset might get severely unwell, and the safety netting advice and that ability
to give that decision making to parents is so important, as part of our job.
Emma: Thank you Liz, thank you Christo. I think this is such an important thing. I think
part of what we do in medicine is lean or reassure, and that is actually harder than giving
out pills and giving out medicine. That is the art of being a paediatrician.
[music]
Emma: Obviously, we've talked about strep throat, but group A strep can cause more
significant illnesses. And one of those is scarlet fever, which actually used to be really
common.
Liz: It was, and also in Victorian times, and you read about in literature, don't you? It's so
fascinating, and Little Women is my go to book for scarlet fever and rheumatic fever
education! So, scarlet Fever is something that we probably need to think about a bit more
seriously. Interestingly, probably most people get better from scarlet fever without
treatment, without any sequelae, but it is slightly more likely to be associated with
complications. So at the moment, the recommendation is that we would treat it, however,
fever and a rash is probably the second most common thing that you're going to see in
primary care, A&E. So understanding how to recognise scarlet fever is quite important.
So, children with scarlet fever develop a flu like feeling with headaches, high fevers and
sore throat, and then the following day or the day after that will develop a very red rash.
And very interestingly, and very importantly, it doesn't always look red at all skin types.
But the fascinating thing is, you can feel it, people say sandpaper, it's rough skin, and it's
kind of all over the body. It starts on the trunk and then it can also spread upwards. That's
different to other rashes that might look similar, like measles, and we're a bit worried
about measles vaccination uptake for preschoolers, so you do need to know what measles
looks like; starts on the face and spreads down. So just remembering to take a history, not
only of where the rash started and what it looked like, but how it progressed over several
days, will help you to make that diagnosis.
Emma: That's so funny, Little Women. I totally think you’re Jo!
I think that's a really good point about rashes. We see a lot of rashes. The first thing I
always think about is take your history is the child actually ill with the rash, because so
often it's really minor and they're not ill and therefore they don’t have scarlet fever.
Children with measles have really red eyes and they're incredibly unwell. And people
aren't really used to seeing it here because it's so rare, they’re much more unwell than you
would expect. And then the last thing I think we need to mention because I always get
this, I get this quite a lot, is EBV (Epstein-Barr Virus). So, the teenagers who turned up with
a sore throat and a rash!
Liz: This the other thing I was thinking of when I mentioned antibiotic rashes earlier. So
EBV in its own right actually gives about 10% of kids a rash which I think people don't
realise and they'll often have a few and they’ll be quite fatigued, and they might often
have lymph node involvement, so they'll have palpable lymph node somewhere and the
rash is much more maculopapular and not palpable in the same way that the scarlet
fever rashes and we are likely to see the kind of post antibiotic EBV amoxil related rashes,
that timing of rash onset is also going to be really important to this cohort. And EBV is a
common virus.
Emma: So Epstein Barr Virus, glandular fever, I always think, again it's going back to the
history, this is often in older children, they have a slightly different history. And the other
thing is, I get this question all the time in the emergency department, people say, ‘Oh,
maybe I shouldn't give Amoxil because I don't know if this is EBV’, but the incidence of
amoxicillin driven rash in EBD is actually relatively small. And if you take a good history,
and then if they're much older and you think it's EBV, but in young children EBV causes a
very minor kind of viral illness. So it is all about going back to the history again,
Christo: I think when we're talking about rashes, and Liz you mentioned this, it is really
important to recognise that a lot of the textbook descriptions describe how rashes look
on white or Caucasian skin. And I think this would be a really useful opportunity to
signpost some resources for how different rashes might look in people who don't have
white skin, and there are various websites such as brownskinmatters which provide
reference photos, as well as the ever trusty dermnetNZ.
Emma: You can also use Don’t Forget the Bubbles who have produced a whole section on
rashes in non-white skin.
The other thing I think we forget about Liz, I worked in lots of other countries, in the South
Pacific, in New Zealand, and actually there we hardly ever saw sore throats but we saw
lots and lots of skin infections and pustules, impetigo also caused by group A strep.
Liz: Yes. So this goes on to the other end of the spectrum of streptococcal and
staphylococcal infections, which cause all sorts of skin infection and can cause all sorts of
problems, so folliculitis, cellulitis, really worrying things like necrotizing fasciitis, that
people just need to have at the back of their mind. And actually, this is really important in
the context of chickenpox, and so we know that a really strongly recognised association
between varicella or chickenpox infections and subsequent group A strep infections, both
cellulitis and then more worryingly, necrotizing fasciitis, which is an extremely painful, just
remember indurated, looks very tender, is very tender spreads very rapidly, bright red skin
infection and doesn't respond to antibiotics. So this is the reason why when you’re a
trainee people have got you to draw around red lines, literally for necrotizing fasciitis. So,
just to be aware of that, and that is a type of invasive group A strep that can become very
serious, very quickly and is a skin emergency. It needs plastic surgery, and debridement,
and broad spectrum antibiotics including potentially cataracts zone and a toxin killing
bacteria antibiotic, such as clindamycin or linezolid.
Emma: Oh Liz, so many pals in one paragraph! So as always, because we're in infectious
disease, we can't actually make a diagnosis, unless you do some tests, so it's all about
seeing children, thinking about what it could be and taking some swabs. So, what are the
samples that people don't do that you want to do?
Liz: That's very good. Well, there is a balance. Not every child who comes in with
something needs a swab. If they're being admitted, or if you're giving them treatment for
a rash, that’s when we want you to do a swab. And we want to have swap at the site,
anything that’s wet basically, you can swab anything that's wet or looks nasty. But also
can you send your MRSA (methicillin-resistant staphylococcus aureus) screen at the
admission so that if they're not responding after 48 hours, we have a result and know
whether to escalate to things like vancomycin, t’s really annoyingly when you don’t have
that. But it's good to send groin, anywhere gooey, groin, axilla, neck swabs, and a throat
swab will also tell us what kind of commensals are around that we might want to take
into consideration for a child who is deteriorating.
Emma: I also ask people to do viral swabs at the same time because of course if they're
wrong, and it's not strep, and in fact you send a rapid viral screen and it comes back as flu
A you've got your answer and you don’t need to give antibiotics.
Christo: Liz, the bacterial swabs have another role more than just guiding management
for that patient because they have a role in surveillance. Is that right?
Liz: Yes, that is such a good point, Christo. So, a lot of what we knew for this outbreak
going into November and December came from three places. One was scarlet fever
notifications, which is GPS and doctors mainly who tell Public Health England, it’s a
notifiable disease and they have an obligation to tell people if they've made that
diagnosis. One is from invasive group A strep notifications. But the third one is
surveillance, which is done in a number of laboratories across the country, where they
look at the level of positivity of throat swabs for group A step for example, but also as, as
Emma mentioned, positivity in sterile sites, that will include things like empyema fluid,
lumbar puncture fluid, etc, etc.
Emma: And that's where sending these notifications and that recent information, that's
where we notice this early rise in invasive group A strep.
So, do you want to tell us a little bit about how it happened and what we should look out
for?
Liz: Interesting, it actually all happened way longer ago than anyone remembers. I’m
going to give a bit of context, it's going to be a slightly long answer warning for those with
a shorter attention span.
So we had seriously high waves of group A strep every spring from 2014 to 2020. And then
in 2020, everyone started washing their hands (what were they doing before?) and
wearing masks, behaving differently and group A strep really went away in very dramatic
fashion for two years. And then it reemerged really late in the season, so early summer
last year, and there was an actual alert from UK in July, to say that they were worried they
were seeing quite high cases of your group A strep at that time using the surveillance
that we've already mentioned. And that settled down in the summer holidays when
everybody washed their hands again, apparently, and then it came back again in the
autumn when the children went back to school. And this is unsurprising. Children are the
ones who get these infections and they pass it around amongst themselves. And so in the
autumn, cases of positive throat swabs and invasive group A strep increased at an
unseasonable time of the year, leading to the outbreak that was slightly unexpected in
November, December.
Emma: That's really interesting. And it makes me feel better because often I say to
families when they come with their snotty miserable children, you don't need antibiotics,
actually what you need is hand washing, cough hygiene which means wash your hands
before meals, cough into your elbow, if you sneeze into a tissue throw it away! Do not stick
it up your sleeve! You should kill it, bin it.
Liz: Yes and it's very interesting. I think we just need to clarify a few things about the
actual notifications of what actually has happened in the last few months because I think
the perception if you are somebody who just read mainstream media, is that the death
rate is massive, there's loads of this really severe end of the spectrum invasive group A
strep and it's all a bit of a disaster zone. Actually, although cases have been higher than
expected at this time of the year, the proportion of serious cases and tragic death in
invasive group A strep is completely in proportion, in fact it may be slightly low compared
to the mild and self-limiting illness. So it is just that it's happening at an unusual time of
the year, rather than it's a disaster zone and that we need to really worry about this
particular pathogen. It’s just the wrong time.
Emma: Perfect. And that kind of brings us around to the fact that occasionally, group A
strep does cause serious invasive infections. But these are very varied. And it kind of
brings me around to my general message, which is: do people know how to recognise
really sick children?
So Liz, do you want to talk a bit about the range of invasive group A strep infections that
can affect children and why are we really scared of them as a paediatrician?
Liz: So invasive group A step is a devastating illness, I'm not going to sugarcoat that and it
is rare, but we do need to know what it means. So what that means is that the
streptococcal bacteria has managed to get through our barriers of the skin or the
mucosa, and into a site where it isn't normally found. And we do see, as I've mentioned
already, chickenpox because you've broken down the skin barrier. It also can be seen after
flu, that's very well recognised when your mucosa is all inflamed, and the bugs can get in.
And then I think this autumn we've recognised that other viral infections that cause
mucosal damage can allow the bacteria to get in as well. And so we can see meningitis,
we can see sepsis, we can see empyema and pleural effusions. We see necrotizing fasciitis
from the skin. We also see osteomyelitis and septic arthritis, and all of these are actually
surprisingly hard to treat, they take quite a long course of antibiotics.
But the thing that as a frontline worker you need to know is, they get very sick very
quickly, and that's why it's so devastating. So you might see a child who has a viral
infection on one day and within 24 to 48 hours, they've become very septic very quickly
and that's where the safety netting and telling parents when to come back is the most
important part of your job.
Emma: Absolutely, I couldn't agree more and I think that it is hard to understand how
quickly that happens. So I think Matt Thomas here in Newcastle did some really nice work
showed that empyema from group A strep can actually appear within 12 to 24 hours. So
really, really quickly. The point about safety netting is my be-all and end-all because it's
rarely difficult to think that actually you're seeing a child at one point in time, so you have
no idea whether they're going to get better or worse after you leave that room. The only
person who can judge that is the parents, and therefore they need to know what to look
out for, when to come and get help and where to get help. And that doesn't mean that
everybody should come to the emergency department. It may mean that you can safely
self-care home, and I'm going to do a huge plug for our healthier together. website
because I think that it has got a really clear red, amber, green rating for parents so that
they can look at their children with coughs or colds or fevers, know where and when to
get the right treatment.
Christo: With regards to treatment of invasive group A strep, what are some of the
differences above and beyond the usual care that you provide to a sick child so, fluids,
senior review and so on.
Liz: So these children are likely to come into A&E being very tachycardic, very hot,
tachypnoeic. So all those things that we hopefully trained you to recognise as red flags,
and they need good access. We really want you to get good samples of these children
before they get antibiotics, so blood cultures and throat swabs, but absolutely the blood
culture. Early antibiotics was broad spectrum, so we use BLANK, but look at your local
guidelines. And the thing that's key if you're particularly worried about group A strep or if
there's any profound erythema or redness anywhere, is to add in something that has an
anti-toxin effect and the first line is clindamycin, and that's why we add it. It can be
stopped if we find another diagnosis, but what it does is it stops the bacteria making
more toxin and it's often the toxin that drives the really devastating, rapid process. So the
clindamycin is really important here,
Christo: Along with antibiotics, is there a role for intravenous immunoglobulin and what
are the limitations around this?
Liz: This is a really interesting point. So intravenous immunoglobulin is magic, a little bit.
What it does is it mops up that toxin that we were just talking about, and it may have a
role, but it should be following discussion with your local tertiary infectious diseases
service. It's not going to be appropriate for every child. It is a rare commodity and it is a
big load of fluid, and that that may not be helpful if you're somebody who's in shock
where fluid management can be quite tricky. And so, the children need first line
supportive care, so small fluid boluses if you're needing more than 20 or 30ml per kilo, you
absolutely need to escalate to your transport services or to your intensive care unit for
advice. Consider early inotropes, which they will give you advice about those drugs that
help with blood pressure, making sure we're monitoring really closely input and output
and considering catheterization. And all of those basic tools of looking after a very sick
child, which you should be supported with, there are extremely good support systems in
our setting. So do reach out and ask for help.
Emma: I think that the thing to remember for invasive group A strep, it's like any serious
disease, if you can recognise it early, then you're more likely to be able to treat it and get a
better outcome. Treatment like the big study from New York, treatment bundles to sepsis
includes fluids, but just sufficient fluid, so 10ml per kilo boluses, always reassessing to look
if they’re overloaded, giving antibiotics early, thinking about whether you need
clindamycin, thinking about giving inotropes early, much earlier than we would have
before, so, after about 40ml per kilo. And the most important thing of all, which Liz said
very nicely, is get help. You are never there alone. Who is your local transport service? Is
there an anaesthetist in your trust? Do you have intensive care? Don't do this alone. You
need help in this situation.
[music]
Emma: We've talked about recognising very serious invasive with group A strep, but I just
want to add in what about contact facing and treating contacts?
Liz: Thank thanks so much for bringing that up, Emma. This is really crucial.
So, group A strep has a very high second attack rate, which means that other people
within the household are at risk of becoming unwell. And so about one in five of those in
the household may develop an infection, and actually can be more seriously unwell than
the person who presented in the first place, particularly if they're vulnerable. The
vulnerable people are pregnant women or those who have recently given birth, neonates,
the elderly, particularly those over 75 And anybody who's immunocompromised. And
actually, what you're meant to do is report it to your local health protection team, who can
then organise prophylaxis. What I would ask you to do, is if this child comes into your A&E
department at six o'clock in the evening, that you just find a way to give antibiotics to a
vulnerable person there and then, because actually the health protection team won’t get
onto the case until the following morning and these second cases can often occur within
24 hours. So, this is where trying to get appropriate prophylactic antibiotics, that can just
be penicillin, but there are very clear guidelines on this that can be lifesaving.
Emma: Yes, absolutely. And we've had cases like that where if a child is brought in and
they die, the last thing you need is for their grandparents, or their siblings, or their
pregnant mother to get sick as well. So, it's so important and really easy to forget, because
actually we're not good at asking who else is living in the family? What are their names?
What are their dates of births? I just want to make a really quick point. Liz, what is a
household contact?
Liz: Household contact is somebody who lives in the house, and spends a large amount of
time with the person. So, we would say probably more than eight hours in the last 24
hours would be a significant amount of contact. And so around Christmas, it's easy,
they've spent all Christmas day in your house, but they went home to sleep somewhere
else. They are still a household contact because they spent the whole of Christmas day in
your house.
Emma: Don't worry about the school and the class, that will be somebody else's job, but it
is your job to contact public health and for them to trace and sort out that. You're just
doing those immediate family contacts.
Liz: If you want to notify a case of scarlet fever or invasive group A strep, please contact
your local health protection team whose details you can find on the gov.uk website.
Emma: Last of all, so we've been the whole way round from having group A strep as a
commensals, sitting on your skin doing nothing, to causing really invasive disease. But
actually group A strep, it's like a party with a hangover because you can have post
infectious complications. Just when you think everything has got better, something else
happens. So do you want to tell us a bit about the post infectious complications?
Liz: Yes, thank you. So, this is what was really fascinating at med school, I thought. So post
streptococcal complications are actually quite rare, and we were worried and we are
going to do some surveillance to see if we see more of them after this outbreak. But
actually after the big outbreak in 2017/18 it doesn't appear that there was a big increase in
them.
So the most common or the one that you will most likely see is post streptococcal
glomerulonephritis, and this is the child who presents 5 to 10 days after a sore throat or an
episode scarlet fever with blood in the urine, in essence. And these children need the
usual renal monitoring with blood pressure and urine analysis.
After that, we have rheumatic fever, and I'll give a fiver to anyone who can tell me without
googling the Jones criteria, I look them up every time. This is a combination of carditis
and arthritis, so bone and heart involvement. And there are strict criteria there. You have
to identify strep, so you have a positive throat swab or a positive ASO (antistreptolysin O
titer) that's very high, that you have changes on an echocardiogram or an ECG
(electrocardiogram), and that you have met some criteria in terms of the joint
involvement. This is really rare in our assessing actually, which is good. It is much more
common in low and middle income countries ,where presumably, we think that there's a
lot more general exposure to streptococcal infections than we see, which is then never
treated. But it is an important one to pick up because if not managed well it can result in
damage to the valves of the heart.
And then we also see something called Sydenham’s chorea, and this is worth looking up
on video. So lovely videos of the type of unusual movements that are chorea, which is
often writhing or gripping and grasping and again, this need management with between
rheumatology, neurology and infectious diseases. And the reason all of these are
important is that these children may need to go on to preventative doses of antibiotics for
a period afterwards, discussed with your local IDT (Inter-Deanery Transfers).
Emma: Fascinating Liz, it's really interesting that it's so rare and wasn't a huge spike after
the last lot of complications. One of the things I wanted to say was, if you give antibiotics,
although that reduces the incidence of rheumatic fever, there is no evidence that it
reduces the other complications, you can still get those. So I think that's another reason
not to give loads and loads of antibiotics.
As you say, all these things are rare. I do see a bit of post streptococcal or post infectious
arthritis, juvenile arthritis. And these are children who have red swollen joints for more
than six weeks, need high dose ibuprofen and when you stop it, the symptoms come
back. I do send those to the rheumatologist and that's a little bit more common, but they
don't have the full rheumatic fever criteria. So I see that a little bit more often.
Liz: A little interesting point about the arthritis and arthralgia with streptococcal infection,
it is very sensitive to aspirin and nonsteroidals where the arthritis, due to juvenile
idiopathic arthritis, tends not to respond to it. So, it's always worth a trial of a good dose of
ibuprofen or even naproxen for these children as part of that trying to understand what's
going on.
Christo: Liz, you mentioned measuring antistreptolysin O titre, what are some of the
limitations with this? Because I think it's something that if you try and read about there's
often a lot of conflicts about how useful it is in day-to-day clinical practice.
Liz: I should never have mentioned it. So antistreptolysin O titre is an antibody response
to having streptococcal infections, and we told you this is really common. And actually if
you took a poll of children, a huge number of them would have a positive ASOT, and it
comes in ranges depending on how much of it is around and how much you have to
dilute the sample in order to find it. And so we would tend to see children who have a
range of 200 to 800, relatively commonly. If you've had a very severe or very recent
infection, your titre is more likely to be above 1200 or even up to 3600. So that's the kind of
range where we would consider that to be significant, but I agree as a kind of screening
tool it’s not very useful. You have to take us in the context of the child and the history they
have presented with, and what your question is. You can't just do it, you have to know
what you're asking about.
Christo: I hate the ASOT because it’s always sent by people who don’t have to look at the
result.
Liz: I was going say though that we just audited ASOT, and got all the ASOTs that were
sent into the trust in under 21 year olds, and that positivity rate is ridiculous. All like 200 to
400, the most useless test on the planet.
Emma: It's been so nice talking to, really enjoyable and so informative. It’s really, really
brought things into focus in a very succinct and efficient way.
At the end of these podcasts, we give you the chance to give us your three top tips, like
desert island where you can only share three messages.
Liz: So remember, you should behave the way you behaved at any other time when you
saw a child in A&E, and your behaviour should not change just because of differences in
reporting of a bug in the media. Whether that is group A strep or something else, the
child needs an assessment to see if they're septic. They need reassurance if they don't
need antibiotics, and they need good safety netting on the way home.
Emma: Christo, do you want some top tips as well? You're looking very cheerful this
morning!
Christo: I think my take home messages from discussing group A strep is that there is a
difference between being colonised with group A strep and having group A strep
infection. Working based on swabs alone can sometimes be difficult and so you'd have to
take the child in front of you, rely on messages you get from parents or carers about how
worried they are about their child.
When it comes to treatment, ignoring patients with invasive group A strep who need
rapid, prompt, broad spectrum antibiotics, and treatment for most of the manifestations
of group A strep might reduce them to duration by a couple of days but comes with the
potential risk of side effects and so you have to make a balanced decision for each patient
in front of you.
Emma: Perfect! I think I’m going to give myself three top tips because I like the last word.
First of all, don't give antibiotics unless you really need to. If you need to give antibiotics I
want to give a huge plug to the UK Paediatric Antimicrobial Stewardship group who have
really good guidelines for prescribing antibiotics in different situations.
If you are going to give antibiotics, can this be done by swallowing pills? Please look at our
pills following podcasts and kids medz information. If this child is over five, why haven’t
they learnt this skill for life?
And last of all, this is for everybody, always safety netting. Safety netting is vital, you only
see a child at one point in time. How are the parents going to recognise if they get worse
and what do they do? I give a huge plug to the healthier together national network.
Enormous large work by Sanjay Patel and Wessex. But it's all the way across the country.
South Yorkshire has a brilliant site, so in northeast Cumberland also. So do you have the
local healthier together website where you can directly text the parent the right
information at the right time?
So, it just leaves me to say a huge thanks, Liz. Absolute pleasure. We might even ask you
again!
Liz: Thanks so much. I really enjoyed myself. Thank you.
[music]
This podcast is a collaboration between Odland, medical education and the Royal
College of Paediatrics and Child Health. You can find more creative learning resources and a wealth of information on the important work of RCPCH on www.rcpch.ac.uk or #ChoosePaediatrics.
[music ends]
Emma: The views, thoughts and opinions expressed in this podcast relates only to the
speaker and not necessarily to their employer, organisation, the Royal College of
Paediatrics and Child Health, or any other group or individual. -
EPISODE 6: Social media – what do paediatricians need to know? (released 23 April 2024)
This month on The Paeds Round, Emma and Christo are joined by our multi-talented podcast producer and dermatology registrar, Dr Jonny Guckian, who runs the medical education site, Odland, and has held numerous social media-facing roles. In this episode we discuss everything social media, including public health information and how to use these apps in a professional capacity. How to protect yourself as a paediatrician? What are the benefits and pitfalls of social media? And where to look for guidance? And a whole lot more
[music, with snippets]
Jonny: We see a real absence of aggressive, well thought out strategies, dealing with
social media or public health information.Christo: I think it's really important that you draw a boundary between what you use
social media for in a professional sense and what you use it for in a personal sense.Emma: You wouldn’t do it when you’re speaking to people, so why do it on the internet?
[music ends]Emma: Hello, welcome to The Paeds Round, the regular podcast of the Royal College of
Paediatrics and Child Health. I’m Emma Lim, a consultant paediatrician at the Great North
Children's Hospital and I'm your host as we educate you on real and pressing paediatric
problems. In this podcast, we discuss and debate educational issues with experts and
always round off with clinical pearls. So let's get going on our rounds!
Social media, of all the things that you never know and wish you did know. It's my great
pleasure to welcome Jonny Guckian, Jonny has been with you for a long time but you've
never known about it because he always hides behind the mix desk and hasn't really
come out. And I've thought, having done two podcasts where he never spoke, that we
ought to give him the opportunity to come out of his hiding hole and talk to us for real so
welcome, Jonny.Christo: And in fact, who better to speak about social media than Johnny, who has been
involved in more social media facing roles than we can name.Emma: And welcome to Christo, my sidekick! And it's a really good thing that we invited
him here today because actually I completely forgotten I was supposed to be doing this
podcast! So half an hour ago. He texts me as I'm driving along in the car and goes ‘Am I
seeing you later?’ And I'm like ‘Why? Are we going out? Were we supposed to be having a
drink or something?’. And he was like ‘The podcast Emma! The podcast!’. So thank
goodness that you are here to keep me on track Christo, really great to see you.
Now today, we want to take you through something about how social media operates.
And I think that this is a great topic, because I think it's something that we just don't think
about often enough. And certainly we think about it in a very black and white way. When
actually it's all grey. I have a dark side, and I tend as a paediatrician to be a little wary of
social media, because I tend to think of it in quite a negative way. Probably because I'm
too old, so I'm not used to using it so much. And probably because I'm always moaning at
my children put their phones down. So, what's your point of view?Jonny: Thanks for having me, guys. I think all this talk of me following around the listeners
so far of these different series, and you having a dark side mix, this all sound a little bit
more creepy than it actually is! I promise we're not all that creepy!
My take on social media, and I'm asked this a lot in various different bits and pieces I do
on social media, is that some people think that social media is bad and has a dark side,
and some people say that social media has a light side or it's all good. And it's very
polarising, it's an extremely polarising medium. Think about it. You must have an extreme
opinion to rise above the parapet. But actually, my take from the various bits of work that
I've done on social media is that social media is a place for people to gather. It is a social
entity, a social platform, or a collection of social platforms. Therefore, it is just like people, it
isn't good or bad. It's a mix. But I think in this podcast will be quite useful to talk about
some of the bad stuff, so you can avoid it. And then some of the good stuff. So hopefully,
we can leave you all with a bit of a positive spin and some practical guidance on how you
can make the most of these platforms.Emma: I think that's a really good point. I think there is no bad and no good. It's actually
complex. Let's start at the beginning. The beginning is always health and safety for me.
What do you need to know or what do paediatricians need to know to keep themselves
safe? And to keep young people and children safe on the internet?Jonny: I think there's different ways that you can look at this. From one point of view, you
can look at your professional responsibilities, i.e. the responsibilities of being a doctor or
being a paediatrician on social media. Your second question is difficult, how to protect
children. I think that is more of a societal and a systemic responsibility, which could be
brought back to the platforms themselves. Because there's lots of implications for
algorithms and child protection measures which can be put into place. But I think talking
about the professional responsibilities and the ways you can protect yourself on social
media as a doctor will be a helpful place to start.
I'd say first of all, it's about following the duties of a doctor, but just applying that to social
media. So I would link everyone who is vaguely interested in this to the GMC’s (General
Medical Council) new ethics hub (https://www.gmc-uk.org/professional-standards/ethicalhub). Which has a whole section on social media.Emma: I am so interested in this. You know me, I am a member of a number of different
groups on social media, but it never fails to astound me that people often put a lot of
clinical information on, let’s say for example, ‘Oh, look at my child. They have a sore throat
and their tongue looks like a strawberry tongue. What would you do?’. ‘I'm sitting in the
emergency department and I have been told that this is a virus but I'm really worried’.
And then there are like 300 responses from people who are not paediatricians, who've
never seen that child and person, telling that person what to do!Christo: And is that not one of the risks? That we like to think that we work in a manner
that is based on evidence, and part of that comes from our good standing within society
as healthcare professionals - but social media removes the ability to quality control, not
just what you read, but also what you say? How do we deal with that?Emma: Well Christo, it's like being accosted at the school gate, but on a monster level. In
the same way that I never tell people I'm a doctor, because then they'll show me all their
rashes! So, in the same way that if I'm at the school gate, I try and behave like a parent,
not as a doctor, because if I tell people I'm a doctor, then they show me their rashes. But
actually, it's not the right place to do a consultation, it's not safe and it's not proper. And I
guess that's the way I think about it, what do you reckon Jonny?Jonny: So, it’s a good thing you mentioned rashes, because we haven't mentioned so far
that I'm a dermatology registrar. And so therefore, there's not a lot of dermatology
presence, at least on UK social media, or at least on Twitter, which is the platform I use
most frequently. A little bit different on Instagram. And therefore, when I'm on there, I get
asked a lot of clinical questions related to dermatology. Now, some of those are just
asking me to drop my skincare recommendations, for which I have none, sorry. And what
there's a lot of private messages I get, which are unsolicited pictures of rashes or people
saying ‘What is this? What do you think about this? My Granny's friend’s dog’s cousin has
this’. And I would say, twice a week at least, this happens. And, I mean, it's interesting and
I try to point people in the right direction for where they should seek support. But
essentially, you should not use social media to provide clinical advice. And even if you're
going to vaguely approach giving general tips about concepts, you should give a
disclaimer and say this is not clinical advice. But maybe if I if I was dealing with a general
case of X, Y, Z, here is where I might find the guidelines for X,Y,Z. Be sensible.Emma: That's a pearl of wisdom. Although I really like the idea of you as the L'Oreal
ambassador, with your skincare routine!Jonny: I think it would be Cerave to be honest rather than L'Oreal. Though I think they're
owned by L’Oreal! They’re not paying me for this by the way, so I won’t plug them too
much!Christo: It’s the dermatology cartel owning both the things that dry your skin out and the
thing that makes it wet again!Emma: I’m going to tell you a secret, this is really funny. I'm slightly older now, but
everybody says ‘Oh your skin looks great, you look so young age!’. And the secret is my
entire family has had eczema for a billion years, because we’re really, really atopic and I
cover myself with whatever emollient a child has twice the day! It doesn't really matter
which is, over the years I’ve used things like Hydromol, Aqueous cream, everything. And it
seems to work just as well as any expensive thing over the counter that's made up of
mushed placenta and pearls.Christo: And we should probably state the disclaimer that this is not clinical advice!
Emma: Are you trying to say that it didn’t work for you?
Jonny: Shall we talk about social media again?
Emma: That idea that you should not give advice, you should always use a disclaimer, and
in general point people towards reputable sites. Three such simple, such obvious tips, I
love, it is really obvious. You wouldn't do it when you were speaking to people. So why do
it on the internet?
So, we talked about professional responsibilities. What about safety in your responsibility
to children and young people on the internet? What would you say in this situation?Jonny: I think it's really challenging. And I think there could potentially be a lot of benefits
for some older children being on some kind of social media platform, which is well
protected and supported. Because we live in an age where digital literacy is essential. And
we know that learners, for example at school and university, use social media to access
various forms of information and assimilate information. However, there are numerous
potential risks, across a variety of different challenges from when it comes to exploitation
and grooming, to the pure, simple risk of overuse of social media. Are we breeding
butterfly minds? With a lack of attention span, as we often potentially hear as a risk. Or
then there’s financial risks, etc.
And I think, as I said before, a lot of that comes down to the responsibility of the platforms
themselves. Because you hear a lot of horrible stories about YouTube, for example, as a
prime example, YouTube is driven by algorithms. So, you stick on a video, and it
recommends another video for you. And in adults there have long been claims and
reported evidence regarding people becoming radicalised, through far right content on
social media or on YouTube, going down the rabbit hole. There has been lots
documented, by QAnon for example, with regard to that. There are parallels for children
and there are countless videos out there for kids on YouTube. You know, people put
YouTube on for their kids all the time, and not necessarily all that content is age
appropriate or screened. And so there are numerous risks with regards to that across the
various domains I mentioned.Emma: That’s brilliant. I mean, there were so many points in that and like you say there is
so much to say. So just going back to financial risks, massive, I think that’s really
underestimated. It happened to me. So, I looked on my email, and then it just says ‘You’ve
been successful! You bid £260 for a blender’. And I was a bit surprised because I would
never spend £260 on a blender, but it was around the time when my daughter was
making a lot of smoothies and I went straight to her. There’s always one in the family! So I
went straight to number three, and I said ‘Where the hell has that blender come from?’. ‘It
wasn’t me! It wasn’t me!’ Of course, all the children are far more internet savvy than I am,
she’d gone on, she made a bid on a certain site and she’d been successful. So, she bought
herself a very expensive blender, and luckily I was able to email the person to say she’s
underage and I did not give her permission and they were kind enough to sell it to the
next bidder. But I think people really underestimate what their children are able to do.Christo: I think going back to your point, Jonny about the algorithms that dictate what
content appears on our screens. Do you think some of this is to do with how interactive
you are back to the content that you’re viewing? So, if you were to leave a child
unattended for the number of hours, then you have no idea as to what videos might
come up on YouTube or on other platforms such as TikTok.Jonny: We all leave a digital footprint, and algorithms do lead us down rabbit holes. That
can happen from the most innocent parties, from a clinical example, not patients I’ve
seen directly, but have read about in the literature. Within dermatology, there is a
condition called dermatitis artefacta, which is a psychodermatology condition where
patients will usually cause trauma to themselves, leaving scarring and this is often in
visible sites and has been linked to problems with stress and mental health problems.
Now there are various trends on TikTok, which essentially encourage a kind of pseudo
dermatitis artefacta picture, where there are things like deodorant challenges for people
spraying their faces, or their hands, or their arms. And kids are kids, they go out of control
and sometimes patients who might be vulnerable to these kind of more dermatitis
artefacta, pyschodermatology conditions, or psychological conditions may be more at risk
of taking it too far. And that’s just one example of potentially many.Christo: Going back to your comments earlier about the roles of a doctor. Do you think
that as clinicians we have a degree of responsibility to try and intervene when we’ve seen
things like this?Emma: I think this is such a great question because it goes under the line of active
intervention rather than passively accepting what you see. And you see so much on the
internet. So what’s your take on this Jonny?Jonny: So, you can split this into your personal responsibility versus systemic
institutional/the profession wide responsibility. I would parallel the personal responsibility
with, let’s say, you’re walking down the street and you’re on a bus for example, and the
person in front of you has a dodgy mole on their neck. Do you intervene? Now, some
people would say yes, obviously, some people would say, absolutely not and they’d been
mortified, it’s a bit like putting your hand up if they call for a doctor on a plane! Well, from
a social media point of view. I think that if we are presented with misinformation directly
to us, we should have a responsibility to point out that it is not correct or direct to the
appropriate guidelines. I don’t need to go into that in more detail because we all dealt
with this in COVID.Emma: I think that’s a great example. I think personal responsibility on the Internet can
be quite challenging. In my experience, I’ve actually contacted, what’s the name of it?
Who’s in charge of a website? What do you call them? The webmaster?Jonny: No, no. A domain owner.
Emma: On occasion, I have contacted the domain owner or hosts, when I have seen cases
of young people where I felt that their clinical details were being overshared without their
consent. And I have asked them to take down and stop certain threads. And actually,
every single time I’ve done it, they’ve always complied.Jonny: You do hear stories, and actually I read a patient who had a lung transplant and
was able to identify her own lungs, or might have been another organ but think of I think
I think it was lungs, identify her own lungs from a picture that was shared by a
histopathologist because of a photo she’d been shown previously. So, she wrote to that
institution and said, ‘Why are my lungs online?’ I don’t think she’d given consent for it. So,
no matter what it is, it can go back to you so just be’careful. Yo’'d like I said you leave a
digital footfall.Emma: Christo, would you stop the man with the mole?
Christo: I think it depends on the setting, and my ability, sadly, to recognise a mole that is
very dodgy is probably fairly poor compared to Jonny.Emma: Do you stop the man with the mole Jonny?
Jonny: Oh yeah, definitely. Any opportunity to show off!
Emma: So, Jonny, we can’t possibly have a podcast about social media without
mentioning fake news. What can you tell us about fake news and social media?Jonny: We’re all at risk. There was a study in the last two years which said that fake news
travels six times as fast on social media, compared to true news, and big information or
news stories are 70% more likely to be retweeted. So, it is endemic at the moment, and we
need to be vigilant. It crosses all specialties. But within paeds there is plenty out there.Emma: I think this is so true, and I think it’s partly our fault. And I think that we don’t use
social media enough. Say for example, if you Google vaccination, 8 of your top 10 lists will
be reasons why vaccinations are hideously bad for you and dangerous, and there’s only
one or two there are actually really good. But actually, we know vaccinations are a good
thing, but we don’t use it enough. We don’t put out enough information and parents
can’t find good, trustworthy information because we don’t make it our business.Jonny: So this goes back to what Christo was asking earlier about whether we have a
responsibility on social media. So, it’s not just about us stopping the person with the mole,
it’s our institutions being braver, and being more agile on social media. At the moment,
there is a risk of being too risk averse, so we see a real absence of aggressive, well thought
out strategies, dealing with social media, for public health information. Our institutions, all
the colleges, should be really across this and promoting careful, well informed
information where patients are, so not just with clinicians, not just on Twitter where the
clinicians are, but they should be going to Facebook groups. They should be going to
Reddit, and they should be involving patients and patient stakeholders in doing so.Emma: I’m so glad you said that Jonny because I’ve just spent literally the last year of my
life working on the northeast North Cumberland Healthier Together website, which was a
fantastic website set up by Sanjay Patel initially in Wessex. And the whole idea behind it
was that primary care, so GPs, physiotherapists, urgent care centres, secondary care, and
parents and families, all wanted one place to find information. And also that the
information was open and transparent, so that you could see what the doctors could see
and the doctors could see the patient information.Jonny: And the benefit there is that with social media, you can reach populations which
previously may have been more challenging to reach, whether that is across racial lines,
or ethnic lines, or socioeconomic class, for example. And this is applicable with, yes, public
health information, but also with recruitment to trials, and involvement in research. Social
media is being used in that domain quite a bit as well. And that hopefully will help rectify
historical disparities with those who are recruited to clinical research.Emma: Yeah, I totally agree. I mean, one of the things we really concentrated on is
making sure that you could use it simply from your phone, because everybody has a
phone. You need to think about making that one content count, so that you could say to
them ‘Here’s the information about sore throats.’ ‘But here’s the information about what
to do if you have a fever.’ ‘Here’s what group A strep really is.’ ‘Here’s what to worry about.’
You don’t just need to worry about having a sore throat and a strawberry tongue, you
need to think about sepsis, you need to think about pneumonia, you need to think about
whether you actually need antibiotics or whether this is a virus which is going to get
better by itself. And I think that’s where the idea of giving one piece of information, but
allowing them to find out all the rest is so invaluable.Christo: And following on this thread, we’ve moved from perhaps the darker side of social
media to some of the real positives that can bring to clinical practice. And I just wanted to
get your idea, Jonny, about free open access medical education.Jonny: Yeah, I’m a big FOAMed fan. This was a movement, it can only really be described
as a movement, which really came at the advent of social media about over a decade ago.
Free open access medical education (FOAMed). It’s essentially sharing of any online
medical education related content for CPD (Continuing Professional Development). It
started off as a real electrifying movement of modernising the spread of informative
content, and as social media has evolved over the last decade, has become perhaps less
accurate all the time, perhaps less reliable all the time, but exponentially larger. And it
really is taking off because it takes advantage of this connectivity of social media. The fact
that you can have a medical student connecting with a world expert on the click of a few
buttons is just incredible, and unheard of in society at large. So that is powerful. But then
as we mentioned before, there are concerns about the spreading of misinformation
alongside the good stuff. So, it’s just the case of applying the same critical appraisal skills
that you might use in your clinical practice.Christo: I think it’s really important that we take what you say on board, Jonny, and use
the same skills that we would use in assessing a manuscript or paper, or even a piece of
clinical information in front of us when assessing a patient to this, because it seems that a
lot of the issues with this information, the core information that’s out there is the lack of
our ability to critically appraise it and remove the bad stuff.Emma: Absolutely. So think who wrote it? Do you know that they’re reputable? When did
they write it? Is there a time scale? Has it been reviewed? And what is the background
over the whole site? Is a site that you trust?
Jonny: What is interesting about how the again, I don’t like talking about generations, but
the majority of let’s say younger learners within the medical education world, they are
doing this naturally, it is a new digital skill which they have adopted and mastered way
ahead of those who have come before them. I did my Masters in medical education about
a year and a half ago, and I looked at the quality of learning that happens in social media.
One of the findings, I’m still reading this up so spoiler alert, but one of the findings was
that learning often happens in networks, where you get a community of students or
learners come together and they find this large piece of content, and they all nibble away
like piranhas, and then they take it and they process it and then they compare it to other
resources, they critically appraise it, they talk to each other about it. And they turn this
large piece of content, which may have not been entirely useful into lots of useful bite
sizes, which have been cross referenced. And I call that process cognitive hacking.Emma: Fascinating Jonny, I think this is so true. It’s really interesting, I look at my children
who come back from school and they go ‘Oh, that was a rubbish day. This teacher was
very boring’, or ‘Somebody talked in the class, I didn’t learn anything’. And they’ll go to
their room and read by themselves, they will go and find the content that they missed,
and they will make it up by themselves. And what I think is fascinating is that it’s a very
active process, and therefore you learn it in a much more in-depth way than if you just
skimmed it and if you were just given the information sitting in a lecture hall like we all
did. Well, maybe not you Christo because you’re so much younger than me.Christo: As a caveat, I think I’m only about a year younger than Jonny.
But I think the point about being active in learning is what differentiates being able to
just kind of consume that information and to those people who kind of take the next step
forward.Jonny: So it’s not even just a case of being active and passive, there’s more to it than that.
If you want to look at the quality of learning, you should use a framework to be able to
quantify it as such or judge it. And the framework that I tend to use was Bloom’s
taxonomy of learning, which for those who are listeners who may have heard of, it starts
off with knowledge then working through understanding and analysis, evaluation,
synthesis, etc. And what is happening there when your kids are going are going online
and looking up things, they are basically critiquing the information, the knowledge that
has been provided, they have understood it, but they recognise the limitations, and they
are going online to analyse it and evaluate it. And some people on social media, then go
and synthesise new content and create new content.
And that’s where it goes back to the very definition of social media, which we haven’t
really discussed yet, because it’s complicated, but I would define social media as a
platform, which gives you the ability to curate or create content or community. And it has
to be multi directional, so a podcast is not social media. And it can be in the public
domain or in private. So, by that definition, you’ve got Facebook, Instagram and Twitter as
your publics, and then you’ve got Messenger, WhatsApp, for example as your privates.
And there’s plenty of options which cross those boundaries.Emma: And I think that’s really interesting, because we’ve talked a lot about content,
we’ve focused on content, but community is just as vital. And I think that people forget
about this.
So, I’m on Twitter like you, and one of the best things that’s happened to me on Twitter is
that I’ve met people that I would never necessarily meet in my day to day life. So
amazingly, I have an academic group with a pharmacist in Liverpool John Moores
University, and I work in Population Health Science Institute in Newcastle University, and
I’m a doctor, so we would never normally cross paths. We’ve actually published a paper
together, and we’re on our second or third bit of work, and that came out purely because
we had a common interest and we met in an online community.Christo: I think a really powerful example of another community that has done so much
for medical education is the movement of the #tipsfornewdocs hashtag that comes
round it seems with increasing frequency, but mainly at the end of July, start of August
when newly minted F1 are about to start. And I think it’s really great seeing the whole
spectrum of doctors who are maybe a year into qualification all the way through to
consultants with decades of experience, joining together to provide useful advice for
people who are quite nervous about starting and really forming a community that people
can go back to with further questions. I think that’s a really, really great thing that
happens.Emma: And since we’re promoting all these other sites, I forgot to say that me and my
pharmacist are working on the Kidzmed project. If you haven’t listened to our podcasts
about Kidzmed, which is how to teach children to swallow pills you are seriously behind
the time. So you better hurry up and go there!Jonny: Emma, you made a great point about reaching people you’ve never met. And
Christo, you made a similar point. This is because these are communities of practice. They
just look different online compared to in the real-world space. And you’re able to reach
out to new people, and that’s happening all the time, as medical students, for example,
are finding professional role models and mentors and therefore, reforming their
professional identity on social media, rather than just relying it on the workplace. Again,
that can be really cool, because you can reach potentially more positive role models and
you’re not restricted to who you’ve got as your consultant for example, which sometimes
can be variable. So, it’s so expansive.Emma: Thank you very much, Jonny, Christo! It’s been a pleasure as always, and now you
know what comes next, it’s our hot tips. Johnny seems to think all his tips are hot, but let’s
see. I wrote down here we have ’23 hot tips, but I think we’ve only got time for three’. SoJonny, give us three!
Jonny: Three practical things that you can do on social media. I’ll pick Twitter as an
example. So, if you go to a conference, tweet at the conference, you will make entirely
new professional networks. You’ll meet people you’ve never met previously who might be
too shy to speak at the conference. So, when you go to a conference, find the hashtag
tweet at it. That’s number one.
Number two is find Tweetorials, or engage with Tweetorials, or even create Tweetorials.
Tweetorials are longer pieces of information split up into individual 280-character tweets,
with a few gifs thrown in. It's essentially the concept of chunking and checking, and
putting complex information into short bursts. It's cool and interesting.
And finally, have online live Twitter discussions. These can be case based discussions or
debates about educational issues. There are a few examples which I would encourage you
to look at, including hashtag MedEd forum which is run by one of my organisations the
Association for the Study of Medical Education (ASME), or there are other clinical ones like
Twitter finals, revision grip, twit, F R G. And these are live, in the moment, case based
discussions. So, one of the examples that I like to give of proper success on social media
learning is with one of our hashtag med forum discussions about reflection. And on there,
we had a debate about the definition of reflection and that was between final year
medical students and the GMC’s Director of Education and standards. And where else
could you get that that disruption of hierarchy, and proper, what I call, pyramid ed?Emma: Christo, what are your hot tips?
Christo: Much like Emma, I tend to use social media in more of a passive, taking
information on rather than giving information out. So, I think it's really important that you
find a network that shows you information that you want to see frequently. And the perils
of the algorithm that Jonny discussed earlier also work in your favour this way, if you
interact with certain content, you will see more of it. So, you will see great Tweetorials by
people who do this frequently.
Secondly, I think it's really important that you draw a boundary between what you use
social media for in a professional sense and what you use it for in a personal sense. And
that can sometimes become a bit blurred, particularly when you're interacting with
people who you're working with, but also who often you are friendly with. But I think
that's really important to try and avoid some of the risks that Jonny mentioned, in terms
of crossing professional boundaries.
And I think the third thing is that I think we probably need to capture some of the really
useful information in a way that is a bit more permanent than just a Twitter like or
retweet. And that might be your own curated list of bookmarks or favourites, or it might
just be sending it on to another third-party service that allows you to store things, such as
Evernote or Notion, but I think it's really important that you can aggregate all of this kind
of really useful stuff in one place.Emma: Okay, thank you. I think that it is been amazing to talk about it. I think that the
things you can do, and the things you can achieve is so much more if you actually get
involved. For me, it has been a real journey. I never would have thought that, number one
I'd make podcasts. I never thought that I would be able to offer virtual work experience,
which I do with sixth formers to broaden access for people whose parents haven't been to
university or aren't involved in the medical profession. And my advice to everybody is to
have a go, try, don't forget to be critical, and have fun. Enjoy it. That's what it's there for.
As always, I'd like to say a huge thank you to all my speakers. And to remind you that we'll
be seeing you next month at The Paeds Round.[music]
This podcast is a collaboration between Odland medical education and the Royal
College of Paediatrics and Child Health. You can find more creative learning resources and a wealth of information on the important work of RCPCH on www.rcpch.ac.uk or #ChoosePaediatrics.
RCPCH on www.rcpch.ac.uk or #ChoosePaediatrics.[music ends]
Emma: The views, thoughts and opinions expressed in this podcast relates only to the
speaker and not necessarily to their employer, organisation, the Royal College of
Paediatrics and Child Health, or any other group or individual -
EPISODE 7: Healthier Together - supporting families with high-quality health information (released 29 May 2024)
The Healthier Together programme provides clear and accurate health information for parents, young people and pregnant women. It's a website, but there's also an underlying ethos to ensure health professionals are consistent in what we communicate with families.
Dr Sanjay Patel, paediatric infectious diseases and immunology consultant, joins hosts Dr Emma Lin and Dr Christo Tsilifis to discuss how Healthier Together can benefit families, especially from underserved communities. Plus top tips on how you can get the most out of the programme.Healthier Together: https://www.what0-18.nhs.uk
[music, with snippets]
Sanjay: The Healthier Together programme is not just a website. It's an ethos about how we take those professionals on a journey with us.
Emma: And it's taking away that awful worry that you're missing the serious illness.
Sanjay: This isn't about illness this is about maintaining health. This is about advocating for prevention and early interventions.
[music ends]
Emma: Hello, welcome to The Paeds Round. The Paeds Round is a regular podcast from the Royal College of Paediatrics and Child Health, and we touch on important topics in paediatrics, and we aim to bring you up to date and talk about relevant educational points for your practice. In this episode of the Paeds Round, my name is Emma Lim and I'm a paediatric consultant in the north of England in Newcastle upon Tyne, and I'm here with my trusty sidekick Christo Tsilifis. Do you want to say hi Christo?
Christo: Hi, my name is Christo and I'm a paediatric trainee working with Emma at Newcastle.
Emma: And it's my very great pleasure to have the fabulous guests with me today. It's one of my dearest and oldest friends Sanjay Patel.
Sanjay: I'm a paediatric infectious diseases consultant based out in Southampton, and Emma and I have known each other for about 15 or 20 years having worked together in London many years ago.
Emma: So, Sanjay and I have been working on something that I am really passionate about, and it's called Healthier Together. And for me, I think the secret to this is I really believe that knowledge is power and that sharing information and sharing health information in an equal way, so that everybody gets to know as much as possible, is the key to this. But at first sight Healthier Together is a website about health information for children and babies, maternity, and young people. Sanjay, how would you describe Healthier Together?
Sanjay: That's a really good question, Emma. And I think at first sight people do think it's just a website. And yeah, I called the programme the Healthier Together programme as opposed to the Healthier Together website because actually, what it's trying to do is empower parents and young people and pregnant women. And the reason we set out on this journey over 10 years ago, was just a simple observation that a lot of parents bring their children to the attention of a healthcare professionals because they're worried about their child. When you look at kind of rates of pathology in children compared to say the frail and elderly, you know, a lot of our management is managing anxiety and obviously within it are a small number of desperately unwell children who do need to be seen quickly and they often come to our attention eventually don't they Emma in our role as paeds ID consultants? So, I think that was the original observation. And then we could look into the literature about why that sort of health seeking behaviour has occurred or is occurring, a lot of it has to do with confidence. And confidence is such a fragile thing, as we all know, as clinicians, you know, in order to be a good clinician, it's all about feeling confident, and it's exactly the same for parents. I think clearly, society has changed over the last 10/15 20/30 years. And parents are the first to admit that they just don't really know when their child's poorly, when they're unwell enough to need attention and when they're really, really poorly to need to go to hospital. And when we look at all the data that we have, you know, there are so many children being brought to ED and primary care and I think that's what we're trying to address, consistent messages.
Emma: I absolutely agree. And I had this really interesting conversation with one of our healthcare associates who worked in the community. And we were training everybody to use the Healthier Together project, and she said, I'm one of those people. I'm really anxious. I'm a serial emergency department attendant, because I sit at home, and I worry and worry. I can't trust myself and I need to go and find somebody else's opinion. He said since I've had access to this website, since I can cross check with my own worries, I've actually stopped going to them. So, for me, that's the key to this. It's that parental anxiety, it's empowering parents, and it's taking away that awful worry that you're missing the serious illness. And you and I know that actually of all the children we see the ones who are serious bacterial infections are like 1%, 1-5%. So, there's a very, very few.
Sanjay: So that's a fascinating story, isn't it Emma? About an individual whose health seeking behaviour has been so radically transformed by access to these resources. And when we've looked at this at scale, and we've looked at it across Hampshire, the Isle of Wight, we've seen similar trends for primary care presentations and for ED presentations. I think for me, one of the aspects of health seeking behaviour is the negative impact we can have as professionals, we generally think that we bring added value all of the time by how we communicate with parents. But I think when you look at how complex our urgent care system is, if parents are faced with inconsistency at the different points in that system, and if they see a GP or a practice nurse who tells them one thing, and then they go on the NHS UK website to get something else, and then they call up one more one and they're told God you need to take the child to ED, it's impossible for them to trust their instincts. And that's why the Healthier Together programme, not just a website, it's an ethos about how we take those professionals on a journey with us to ensure that we are consistent in what we communicate with parents because I think that that's going to be the game changer in terms of parental confidence.
Emma: Absolutely. I think that's so important. This idea about consistency. I see it all the time with different advice about weaning, different advice about cow's milk protein allergy. And I think when you go onto the website, there's two things, first of all you can see an area for parents, you can see an area for young people, so they don't necessarily want the same information as their parents. And you can see the professional's information and it is completely transparent. So that a parent can go look at the professional's information if they want to. And lots of parents do a lot of digging around on the Internet. And they do like to see, I often say to them if you're the sort of person who likes to read lots on the Internet, have a look at our professional site, see what they should be looking at, see why they think you should go various places because it's all transparent. And the other new addition to the Healthier Together programme is an app for your phone. And the great thing about an app is, first of all, it takes up some of the unnecessary information, so if you put in your details for how old your child is, you only look at the bit that is relevant for that child. If for example your child is, let's say coughing, you can then put in the symptoms like coughing and you will be taken to the page on coughing. It will ask you some questions and the questions will then rank your child's symptoms into the red, amber, green categories. So red is obviously bad, red is you need to go straight to the emergency department. And the amber category is for like grey zone, and that is where you might need some health information or advice from another professional. That could be from your GP, it could be from 111 and there will automatically be links to your GP and your GP could then email back some advice to you. If you don't have any red or amber flags as it were, it doesn't mean that your child is well, but it does mean that your child is safe to stay at home and there is some simple self-care advice. For example, taking paracetamol, not wasting money on cough medicine, which is one of my bugbears. So, Sanjay, tell us a bit more about how the app works.
Sanjay: Yeah, the app is the newest addition to the Healthier Together programme. So, if we think about one arm of the programme being the website, that's clearly quite static information, that's one directional in terms of we can put content on the website and people read it. We obviously base lots of our training of professionals of the content on the professional site. And so almost the key to embedding the Healthier Together programme anywhere is to ensure that all of those professionals, from our voluntary sector colleagues to our health visiting colleagues, to primary care staff, to ED doctors, etc, that we're all consistent. But then the newest bit is the app, and the app really takes into account functionality. You know, we're also used to using tech digital technology, we use it for banking, we use it for everything now that. The app is more intuitive in terms of displaying the core information the parents want and that's the red, amber, green content. But in addition, it's functional in terms of integration with primary care and NHS 111, potentially. So, in Hampshire or the Isle of White, if a child in working hours has amber features, the app will send a message via the app to the GP practice. The GP practice will review that information the same day and communicate with the parents. Out of hours it links up with NHS 111, and so you get a similar functionality.
Emma: I know also Sanjay that you have this master plan where from like sort of conception to 19, you'll be linked to Healthier Together. So down South you've actually done a lot of work embedding the maternity app into this. How does that work?
Sanjay: Well, we all know that improving pregnancy has such an impact on childhood outcomes. And we have a really captive audience with pregnant women. As anyone would know, when they're pregnant with their first child, you're desperate for information. And so, we've worked really hard with our midwifery colleagues. And this work has been recognised by the World College of Midwifery, in terms of their digital awards that they awarded the app earlier this year. And it provides very similar functionality to the paediatric app, that when a pregnant person is worried during pregnancy, they can access resources easily and they can integrate with the maternity desks that we have in Hampshire. And so, it really means you get the right information in a timely fashion. And looking at the data we have the maternity app, most of the requests and information seeking by pregnant women results in reassurance and no need to progress up to further discussions.
Emma: So, for example, you're pregnant with your first baby, you might be worried about less foetal movements you can go on to a page on the app, check out that it's okay. Get a response from a trusted professional so a midwife or your GP and then be reassured, and that would save people from actually making unnecessary visits. And you've got some evidence to show that the app has actually reduced visits or reduced attendances, is that right?
Sanjay: That's right Emma. We've got evidence to show that it's reduced visits to GP practices, and that's the data we're getting from our GP colleagues across Hampshire and the Isle of Wight. And we're just getting feedback from pregnant women that, you know, for many of the things that worried them, similarly to parents, that they find the content very reassuring and easy to access. And I think the real strength of the maternity app actually is that not only do they create a profile for themselves, but as soon as their baby's born, they create a profile for their baby and other children in the family. So, it's a very powerful way of having parents creating profiles for their children. So, I envisage in the next five years, every child in Hampshire or the Isle of White will have a profile on the app, because every pregnant woman in the past year has created a profile for herself.
Emma: There's one other thing that I really want to talk about. I think that you and I know the kind of people who look on websites and apps are often well off people, educated people, they're hunting for more information, they've got a laptop, so it's second nature for them to look up health advice and be able to judge what is good and what is not good. But how does Healthier Together help the underserved communities? How is it that to provide a leveller for health inequality?
Sanjay: I think that's the million-dollar question Emma. And I think we spent a lot of time thinking about that as part of the Healthier Together programme, not just with our sites in Hampshire and the Isle of Wight, but with many of the other 15/16 ICS that have on boarded with the programme. I think it goes back to the initial discussion we had about Healthier Together not being just a website, but being an ethos, being a way that we can integrate care. The pendulum swung so much during COVID towards digital offers, and I think we're increasingly realising that that's not the answer, you can't do everything digitally, and we can't deliver healthcare entirely digitally. We have a myriad of extraordinary people that deliver health care, from volunteers to help visitors to midwives to primary care staff. And actually, in my view, Healthier Together is just a platform to support those individuals. And so, it's not about having access to a website. It's how those individuals can be empowered to better support those families, because those are the professionals and volunteers that go out to support the most vulnerable families. And a thought I've had recently following discussions with the Department for Education with NHS England, is the siloed working that we're forced to work in, we work for the NHS, so many of our thoughts relate to NHS pressures, but when you speak to colleagues from the Department of Education, their pressures are to do with school attendance, and school preparedness. And when you actually think of the children that you've described, you know, who are these extremely vulnerable children? They're the same families, the same children. It's the same child that's not attending school, that has potentially got safeguarding issues, that is potentially presenting to primary care or ED multiple times. And so I think we need to change our approach to delivery of care away from siloed working to patient centred and family centred approaches, and I think that's where Healthier Together can really win, I think offers a platform that teachers can buy into, that social care staff including local authority staff, public health staff, health visitors, they can all buy into and healthcare professionals can buy into. And so that's where I see the vision of the Healthier Together programmes supporting the most vulnerable families and society.
Emma: Yeah, and I think that's something that we've not really talked about, that it's not just specialists like ourselves or GPs who've done so much work in building this site. But it's actually how this site is used out in the community. So, we have a Champions programme, because I think you're right, people don't want digital information all the time. They want the information from somebody they trust, and somebody you trust is usually somebody in the community, who understands what it's like to live and work in that community. So up in the Northeast, we've developed a Champions programme, where we had special training for people in the community. Some of these were non-governmental organisations, parent groups, schools, and they would all come and get a bit of information and then they would go back to the community, and they would then champion the Healthier Together projects to their community. It's very interesting you picked school attendance, we had really good feedback from one of the schools. We have a really great page which says when your child can go to school, so if you have diarrhoea, you have to stay off for 48 hours. If you have nits, it's bad, but it doesn't mean you can't go to school. And they had some children who weren't attending quite a lot with things like a little cold. And they sent them the page and they said every time they're sick, we will be looking against this page. And the parents actually really found it very reassuring and that's child's attendance improved. So that's a very real example of how information on the site ended up with better school attendance for a child.
Sanjay: I think your point is very well made, Emma. What we've realised, all of us as healthcare professionals or just as members of society that that care for children, is that schools are hugely protective. And so, although we perceive school attendance as a kind of outside of our sphere, we know that when children don't attend school, they lose their most important, protective mechanism, especially for them for their emotional well-being and mental health. And so those same children, if we don't focus on school attendants, will end up coming onto our wards with eating disorders and self-harm and altered behaviour, it's not a them problem. It's not an DFE problem. It's anyone who wishes to advocate for children and support children needs to recognise that need to work together. And so I think the model you've described of the social prescribers or health and wellbeing champions in community settings is exactly the right model to go through and it's something we're working up with The Well Centre, which is a charity in South London, that model to support young people and I think that's the model we should be advocating for across the country.
Emma: Absolutely, there are quite a few great examples. So I think in Liverpool in Ian Sinah and Alice Lee, had parents centre hubs where they use the same kind of information to teach the local community, so they've taught people in the local community about bronchiolitis and they had bronchiolitis champions and they showed that they could safely reduce emergency department attendances and increase everybody's knowledge in the community for such a simple common condition. So, I think that it's really important that, I guess that relationship where Healthier Together is actually like the glue between tertiary primary health care, communities, schools all these other things.
Sanjay: I was reflecting on the name of our programme just at the weekend you know, as I said, we develop the programme 12 years ago and the focus originally common illnesses in children, especially children aged under five because they make up a huge amount of primary care and ED activity. But increasingly, I recognise that almost the luck with which we chose the title of our programme really reflects what we're trying to achieve. It's all about Healthier Together. I think both of those terms, this isn't about illness. This is about maintaining health. This is about advocating for prevention and early interventions, and together, reflects entirely the integration and how we have to work with all of those extraordinary people that support children in our society.
Christo: I think that's really interesting, Sanjay, because taking the second part of the name of the programmes so the Together, you've talked quite a bit about information going sort of from us as healthcare professionals out into the community. Do you have any mechanisms by which you're getting feedback from parents, from schools, from other people who are involved, about what to develop? Whether any content needs changing or updating?
Sanjay: I think that's the key to the success of the programme, actually, Christo. I think that it's only if people feel that this is their initiative, do they buy into it. And so, I think we've called it a social innovation. I can't even remember the term we've used on the website, but it's very much advocating for this is us working together to support our local community. And there are two bits to that. There's that local bit, because one could always perceive Healthier Together as a big national programme, and the vision has never been to do that. You know, this has to reflect local services and it's got to listen to local young people, local pregnant women, local parents, local professionals, and that's what we strived to do throughout.
Emma: We went out to a Sunderland youth group to do a design sprint, because we have different parts of the website. So, Sanjay has talked about the maternity and the child section, and we've got a young people section. But young people never look at websites. They just don't and we're all aware of this. So, we developed this design sprint, and we went up to Sunderland, and we spent the whole day with Professor Greta Defeyter and Professor Joyce Lee, and a whole group of youngsters in Sunderland and we asked them, how would you co produce a young person's section for Healthier Together? And it was absolutely amazing. It was gobsmacking they had so many ideas. So, I'll just give you a little bit of feedback. For example, they said no, we don't look on websites. We only look on Instagram or TikTok, so you've got to get yourself a TikTok account. We actually think you should be Dr. M and that you should have like a weekly kind of like update where you just chat, they said we just want 15 seconds of a little bite and then we might go towards that. The other thing that was interesting is they absolutely believe and trust the NHS. When they were asked, they all said they would go to an NHS website, and they would look up health information there. And the NHS websites are really dry, and I think quite complex. I think ours is much better. So, there is a precedent, they will look for health information if they're signposted to it. But I'm always completely gobsmacked by the way that young people actually have an enormous amount of energy and drive, and real intelligence about how we design these things.
Sanjay: Do you know I was going to reflect on something similar but reflecting to professionals. I think if you give people the opportunity to be heard, and I think if you give people the opportunity to try things and to innovate, they don't cease to amaze me. I have trainees that write to me constantly saying, could we develop this page for the website? Could we do this project related to Healthier Together? And if you ask me, what am I most proud about Healthier Together? It wouldn't be that we've rolled out to half the country and that you know the Royal College of Paediatrics is hugely advocating for it to be rolled out to the rest of the country. What I'm most proud of is it offers people a platform to be heard and to try new things and it improves morale of staff. I think morale is single handedly the most precious commodity that we have in health and social care and from our voluntary sector colleagues, and if this programme has any impact on morale, we should be most proud of.
Emma: I think that's so true, Sanjay, I think it's morale and it's listening because there's no way one or two people can know everything. And it's the surprising, unusual things that people come up with. So, for example, we have the same experience, a trainee came up and said, I'm going to make some videos for you. I said Oh, that's great. What are they? They said, we're making videos for families of children that have tracheotomies, breathing tubes. When they fall out, how do you put them back in when they get blocked, what do you do? It's really hard to read about that. You just need a video to show you what to do. That's what all the cooking shows and everybody else does. So, they're building an entire segment on how to care for your tracheotomy tube. Specifically for parents of children on this website. So yeah, it's been open hearing what people want to do.
Sanjay: To me your description of trainees developing that content, you know, it is such an important part of the vision of the programme because so much of our work is about sharing good practice and not reinventing the wheel. And what we've achieved through having 151/6 different Healthier Together sites is that we're all able to share the best stuff. And so, I know that you and your colleagues have developed fabulous resources. You've done some of the work on testicular pain, in partnership with others. We've unashamedly then taken that and put it on our website. Our colleagues from West Yorkshire have done some extraordinary work on neurodiversity. And just last week, I added that to our website, and I think that's what's brilliant about the programme is it allows us collectively across the country to share our talents and to people and harness that energy, so that it's shared at a really wide scale.
Emma: So, I just wanted to ask Christo something, what's your favourite function on the Healthier Together website, project, platform?
Christo: I think practically the way that you can try and get the information on the pages to patients. So, I suppose I'm thinking of two scenarios. One when you're seeing a family, in say children's A&E, and you think there's some really good information and rather than having to print it or use email or something like that, there's a simple button where you can text it to a family member's phone, they get a link. It's not linked to your mobile phone or to your email address at all, so it's kind of anonymous from the point of view of the practitioner. And but I think more useful than that or even more useful than that is the kind of inbuilt translation because I think that's one of the challenges when we're seeing families in A&E. And we know that these families, the ones for who English isn't the first language, where we do them a disservice. It takes a lot more of our time, and we miss things and there is nuance that is lost. And I think if we can find a way of making that communication a bit easier, then I think everyone benefits from it.
Emma: Christo, you had two points, but they were both brilliant. So yeah, absolutely. The texting, there's a yellow button at the top it's a yellow box, you press on it, and it immediately sends a text of that page to the person in front of you. So, first of all, you know they got it. They can't lose it. It's on their phone. And remember, every time you meet people, they only remember about 30% of what you've said. And that's if you're lucky. So yeah, I use that all the time. I think that's really important. Your second point was so important. I mean one of our big drives is to be inclusive. So, we have Recite Me on the website so it will automatically translate, and it will read out the information on the page. And I think this is vital, because actually it's not that easy to read, and particularly when you're stressed. And we've also had a real drive to actually make it simpler, so we've started to include easy read pages, because actually sometimes you need something really simple, and you don't want all the detail. The national literacy level is around eight years of age, you need to think about the Sun newspaper and frankly, that's what you should be aiming at that level of information. Because when you're stressed, when you're worried, you don't need to read too much, you just need to read the important things. Sanjay, I think we're almost at the end of the things I need to talk about. So, Christo had his two favourite things, I'm going to ask you what are your three top tips for Healthier Together?
Sanjay: I think firstly, give getting it in your region. So, I think advocacy is the first thing I'd suggest for all of you and many of you listening to this podcast will have Healthier Together in your region. As I said it covers about half the country. We're trying hard nationally to find the support to roll out to every single ICS in the country. But I think there's a big difference between having the website and actually having an impact on families in your region. And that's why advocating for it, that's why using it, that's why sharing it with all of those colleagues across health and social care to support young people, and finding a way to listen to them so becomes your initiative I think is the first step. The second bit is probably something for the paediatricians listening on this webinar, in that we probably more so than ever need to advocate for families. I think that the financial crisis affecting this country has meant that more and more attention has moved towards the most costly bits of health care, which is often the frail and the elderly and has moved away from paediatrics. I find it harder now to advocate for children and young people than at any point in the last 12 years. And I do think that programmes such as Healthier Together, that are evidence based, are definitely grounded within frontline professionals that have got a huge impact, not only on health and on Urgent Care activity, but on school attendance, on safeguarding, on addressing some of the social determinants of health. We need to advocate for them. And we do that by advocating with our local commissioners, nationally with NHS England, and above that and some of the work we're doing is now advocating that governmental level in partnership with the Department for Education, Department for Health and Social Care, Institute of Health Visiting to really push the paediatric agenda and I think we've all got a responsibility to do that. And thirdly, it's probably collect data. So, in order to maintain buy in, and to continue innovating, we need data to show the impact. We're awash with data in the NHS and yet we're so data poor in terms of the time and energy and access we have to those data, but I would really, really suggest that people try and get hold of that data and look at the impact of Healthier Together and look at where your hotspots are for needing to address issues. And use your data to innovate. Use it as a way of working with your primary care colleagues, working with your voluntary sector colleagues, because actually the new models of care, which almost frontline clinicians have to drive, you know this isn't going to come from NHS England. This is going to come from us, people that desperately care about children and spend our days and lives looking after. So, use it as an opportunity to collaborate and to innovate and to bring about new models of care and new ways of work.
Emma: Amazing. I mean, obviously this is kind of like preaching to the converted, but I think Healthier Together is incredible. It's evidence based, it's easy to use, it's efficient, it's effective. And I think our message to you, to everybody is use it, share it, personalise it, collect data for us and for everybody, and innovate with us. If you're not using it, if it's not in your region, just drop us a line. We absolutely want to spread it everywhere. If you are using it, fantastic! You're already one of our champions. So, congratulations to you. And thank you very much, Sanjay. That was really lovely to see you on a Monday morning.
[music]
This podcast is a collaboration between Odland, medical education and the Royal College of Paediatrics and Child Health. You can find more creative learning resources and a wealth of information on the important work of RCPCH on www.rcpch.ac.uk or #ChoosePaediatrics.
[music ends]
Emma: The views, thoughts and opinions expressed in this podcast relates only to the speaker and not necessarily to their employer, organisation, the Royal College of Paediatrics and Child Health, or any other group or individual.
-
Episode 8: Measles in 2024: what paediatricians need to know
With measles hitting the headlines recently, The Paeds Round is delighted to welcome back Dr Liz Whittaker, who joins Emma and Christo to fill in the gaps surrounding a condition which has laid dormant for decades due to the success of vaccinations and is now on the rise again. To address some of the knowledge gaps, the panel go over questions such as what is measles? How serious is it? How infectious is it? And what do you do about it? How do you tell if a child with a fever or rash has measles? What are its long-term implications?
Dr Liz Whittaker is Senior Clinical Lecturer in paediatric infectious diseases and immunology. She divides her time between Imperial College London and the Department of Paediatric Infectious Diseases and Immunology, St. Marys Hospital, London where she is a Consultant.
[music, with snippets]
Emma: Try and use tissues, throw them away, cough on your arm and wash your hands! I can't say this often enough.
Liz: Did you know that 90% of unvaccinated contacts will get infected?
And so, I think people you know worry about the acute phase, but it's the long-term impact that's really devastating.Emma: So, I think key point here is what you said earlier, is take a good history, make sure you've identified them, and then get advice from your paediatric infectious disease team or the HPSO.
[music ends]
Emma: Liz, it's very nice to see you again! Who knew that I would see you so soon? So, my name is Emma Lim, I'm a consultant paediatrician at the Great North Children's Hospital. And we're here on the Paeds Round, talking to Liz Whittaker from London, who we've actually already talked to on our Group A Strep podcast, but we've asked her to come back again because we liked her so much before, to talk about measle! Liz, would you like to introduce yourself?
Liz: Thanks, Emma. I'm Liz Whittaker. I'm a paeds ID consultant in St Mary's Hospital in Paddington, and I'm also an academic working at Imperial College London, and I have an interest in all things infection and immune related. And apparently, I'm becoming a bit of an expert in fever and a rash, who know?
Emma: The reason that we wanted to do this today is because everybody is getting very worried and excited about measles. And one of the problems is that because the vaccine is so effective, for so long, people aren't used to seeing it. They don't have much knowledge about it, and we seem to have lost that kind of knowledge about what measles is, how serious it is, how infectious it is and what to do about it. So, we're just here to fill in those gaps today.
So Liz, I'm just going to ask you some questions. The first thing I want to talk about is we had a really straightforward case. Our paediatric emergency department is always full of children with fevers and rashes, and the other week, we had children with fevers and rashes, and one of them turned out to have measles. So, my first question is, how can you tell if a child with a fever or a rash has measles or something that's not measles?Liz: I think that’s an excellent question. And the problem is, it's probably not that obvious. They don't come in necessarily, with the slime on their head. The differential for a child with fever and rash is obviously very broad. Somebody I think Damian Roland, friend of ours, came up with the catchy phrase, which is ‘fever, rash, and the three C’s’ and the
three Cs are coryza, cough and conjunctivitis. Now that also pretty much covers adenovirus and few other things like that. So that's not necessarily going to be the most useful guideline. What really makes you think about measles is an epidemiological link, and the link there is usually that they're unvaccinated, or possibly partially vaccinated, but usually unvaccinated. That they've had a contact with a known case of measles or another unvaccinated child with a similar illness, that they've travelled to a high-risk area, in the Birmingham, the West Midlands at the moment. But it could also be parts of Africa, Asia, or Eastern Europe. That they are in a nursery with lots of other children who have also had measles, so known contact. So, these are your main questions that you want to ask to kind of make you think, right, I need to get this child out of the meeting room and into somewhere where they're not going to pass on very generously this very infectious virus.Emma: Perfect. Thank you. And I think that the public has forgotten what measles is like as well. And so, you like and I have worked abroad, measles is a really nasty illness. It is not like chicken pox. It is not like a cold. And so, children with measles, when you say they have fever and a ration three C's, it starts like a cold. They have really nasty, sore red eyes, and this distinctive cough, but what's really obvious is they are much more unwell at this point than other children. Is there anything else?
Liz: And miserable. I completely agree, Emma. I think these children are sick and miserable, and I know we use that word in the context of Kawasaki, which is another really important differential for these children and why they need careful assessment. But children with measles, they feel utterly awful, and they behave like they feel utterly awful, whereas your average child with roseola or parva virus or other kind of common fever and rash patterns don't feel quite so unwell. And I guess the thing that discerns them, then,
from perhaps scarlet fever, is going to be the cough and the eyes, the two of the C’s may not be there in scarlet fever. That is another important differential. And as Emma was outlining, there is a pattern in how this comes about, in terms of three or four days of coughing, cold like illness, before developing a very distinctive pattern of rash, which parents may or may not be able to describe, starting behind the ears, the hairline running to the face and the rest of the body. And then over four to five days, becoming very confluent, become red, particularly on the face, and then it spreads and clears down through the rest of the body. And they may have the magical Koplik’s spots that every paediatrician aspires to see before they finish their career. And I've only seen them once, because generally the patients present after they've gone. But if you see them, you should definitely take a picture and put it in your teaching portfolio. So, the fever, rash and three C's and the three Cs are coryza, cough and conjunctivitis.Emma: Brilliant. So, we've said we've got this really sick, miserable, rashy child there with measles. And I guess the next question you're faced with is, when should you admit children? So, what happens to children with measles? What are the criteria for admission? Because actually, in our case, the child wasn't that sick, and we sent them to the safest place, which is back home.
Liz: So most of these children will be managed in the community. So, we say that one in seven children will develop complication. But a complication can be something like Otitis media, which is probably the most common thing, or it can be more severe things like pneumonia and convulsions and encephalitis and things like that. And so, your usual red flags you'd be looking for in the ED or in primary care or any setting, are tachypnoea, fever that's lasting longer than you'd expect, lethargy, abnormal movements, poor oral intake, are the reasons for admission as usual. And then the other thing just to be aware of is that younger children are more vulnerable, and so we say the under twos, but absolutely the under ones, we would have a lower threshold for admitting. And I guess if there isn't a clear you know, you're not exactly sure what's going on, these children should have bloods. So not every child with fever and a rash needs bloods, but if you're thinking, could this be Kawasaki, is it measles? That would be a reasonable time to do some inflammatory markers, because generally with measles, they don't tend to have really high nutrical counts, CRPS and low albumin like you would see in Kawasaki, and they tend to have quite low inflammatory markers, even though they're so unwell. And then the other thing that they can get is secondary bacterial infections. And that’s the other reason that you might want to do blood in a particularly unwell child, is just to make sure you're not missing something that needs antibiotics as part of the management.
Emma: Brilliant. Yeah, I absolutely agree. I think, you know, people forget. They can get diarrhoea, they can get dehydrated, they might just need fluids. I think the other diagnostic conundrum is that children with measles get quite a high temperature, and then they have a fit. And then your problem is, is this a febrile convulsion, or do they have encephalitis? And that's another time you might want to admit them. You might want to do some tests, and then you're thinking about lumbar punctures, possibly doing some scans of their brain. And I think that people do get confused with the difference between acute encephalitis and SSPE. So, I'm going to ask you to go through febrile convulsions, encephalitis and SSPE, which is Subacute sclerosing panencephalitis.
Liz: This is really difficult, but this is what we do with paediatricians. The child in front of you has this snapshot here, and you have to make a decision about what you're going to do, and the safest thing may be to admit these children. And looking at admission rates in the UK, they are probably higher than needs be, but often with very short admissions. And I think that's because the safest thing to do maybe to bring somebody in for 24 hours for observation. Because if this is a febrile convulsion, which is common in this age group between six months and six years, then obviously they bounce back and recover quite quickly and will have relatively normal bloods and won't be lethargic and encephalitis in the recovery period. But if it is encephalitis which we don't want to miss, because there may be specific treatments we want to give. Or certainly, they may end up becoming very unwell and ending up in intensive care, then being in hospital is the safest place if they have that progression. Subacute sclerosing panencephalitis, which we all know way more than we should have given how uncommon it is, doesn’t actually happen in the acute phase. This happens later down the line and wouldn't be part of the acute illness. And it is vaccine preventable and that is the thing that is so tragic about the low vaccine rates in children at the moment. And it occurs in about one in 10,000 people, and we've all learned how to recognise this on an EG so that we can pass our membership exams. But I think actually we need a clever neurologist to remind us of it when the child presents outside the context of febrile.
Emma: What are the incidents of encephalitis? How would you expect somebody to recognise encephalitis, as opposed to ordinary seizure with a fever?
Liz: So, encephalitis, so convulsions happen, as you said, relatively often, in about point five per cent. And encephalitis, we think, is in about one in 250 or between one and 250 and one in 1000 so it is relatively common, to be honest, I think that's why I would say that was a relatively common for an infection. It’s just that the infection is rare in our setting. And children with encephalitis may or may not have seizures, which may or may not be focal or generalised. But their level of consciousness is subdued, and so they would be, often very lethargic. And I think you do need to remember that lethargy can be a symptom of encephalitis, I think people will be like, ‘Oh, they're just sleeping a lot’, and I’m
like that's not normal, children should be waking up to feed, and they may sleep more than usual when they're unwell, but they should wake up and be completely normal in between. And I think it's really important to be able to make that assessment. I think parents struggle with that sometimes, but that you as a health professional should be able to tell that they're not waking up, sitting up, having a drink, being inappropriately interactive, and then that's when we worry about encephalitis.Emma: But for me, that is actually quite a common complication, and this, for me, is one of the reasons that I would really want my child immunised, because I think this is actually much more common than in ordinary viruses that we see in the community.
Liz: Absolutely, and you know encephalitis can have long, lasting impacts. And they may be severe, so these children may develop seizure disorders or other obvious neurology, but they can also be subtle in terms of neurodevelopmental and behavioural and learning difficulty impacts. And so, I think people you know, worry about the acute phase, but it's the long-term impact that's really devastating.
Emma: Absolutely. So, we've talked about the child who came to the emergency department, our criteria for admitting them, some of the complications, but we haven't really talked about how we definitively know if this child has measles or not. So, let's talk a bit about investigations.
Liz: I think actually, it's so confusing, because a lot of the national guidance talks about the Health Protection Team sending oral food spots, which they do, but most of that guidance isn't actually for a hospital setting. So, if you have a patient in front of you in hospital, and particularly if you're admitting them, then you need to send a diagnostic test through your hospital laboratory. And that will usually be an oral fluid test, so it's great you don't have to try and aim for the tonsils. They can just suck on the swab, and it needs to go into a viral fluid medium. And that will vary depending on where you work, but it's really good to go and find out what that is. And I can't tell you what every hospital does, and some hospitals are in house testing. Most hospitals are sending it to an external lab for testing. The turnaround isn't actually as rapid as it might be, for example, for a rapid test for flu or RSV, and so you will often have to manage this on suspicion whilst you wait for that diagnostic test. I think even if you're sending them home, it is helpful for the Health Protection Team if you could send a diagnostic test before they go, because otherwise they post out samples to the family, who then have to post it back, and we know that that's an unreliable system, so they don't get full surveillance data. So just even from a surveillance perspective, and then contact tracing, it's really helpful, if you don't mind doing that. Thank you. So that oral fluid test is usually for PCR, for the measles virus. It's a molecular diagnostic test looking for the genetic material of measles. They will also often do oral serology for IgM and IgG, which is less specific, but a very high IgM sometimes comes back quicker than the PCR and can also be really helpful from a diagnostic perspective.
Emma: Fantastic. And I think you've got to remember, this is a child with a rash, and often it's not as obvious as it sounds like when we're talking. So really, what you're going to be doing is taking some swabs, and you're going to be looking for flu, adenovirus, RSV. Maybe you'll do your normal viral panel, and then you'll do this extra swab for measles. And you might be doing some blood tests, and those would be standard routine full blood counts, renal and liver function. And you might also be thinking about streptococcus, so you might be doing a bacterial swab for that or thinking about an ASOT. So, at this point, it's just remembering that measles is around, and you need to add in an extra swab.
Liz: Exactly. And I guess the other thing to be aware of in a very sick, young infant, if you're not sure, do call your regional paeds ID team. We love chatting about children like this to give you advice and support if you're unclear. And actually, the list of investigations on your Kawasaki guideline will cover most of things that we would like you to send out a quick turning point if you’re in A&E looking for something quickly.
Emma: So, we've talked about this child and our child wasn't very sick. We know that in most cases, viral infections get themselves better. But should we talk about what we can do to look after or treat children with measles,
Liz: Yeah, and it is actually mostly supportive care. Som you've mentioned diarrhoea, really, really common to get diarrhoea in measles, and so input, output, weights, fluid management, the usual things that you would do for that, making sure they're not tachycardic, etc. NG fluids are always preference for me, but that will vary from side to side if you can do it. Managing the fever and then looking for secondary bacterial infections and giving antibiotics as appropriate. In terms of specific treatments, we don't have great antivirals for this, and you will hear people talk about ribavirin, we wouldn't recommend this routinely for patients with measles. And the other thing to be aware of is people who, particularly if you've worked overseas, like Em and I have you, you may have doled out vitamin A to children in a measles outbreak in another setting. That's actually not appropriate in our setting, because the children in a refugee camp, for example, have other risk factors for severe disease, including malnutrition and vitamin deficiencies. And so that's when vitamin A has been shown to have proven benefit. And there may be some children who are severely unwell in an intensive care or in a hospital, for whom vitamin A is appropriate, but for most children with meetings, we aren't recommending vitamin A. And then finally, for patients who are immunocompromised, there may be a role for intravenous immunoglobulin. This would obviously be on a case-by-case discussion with your virologist and paeds ID teams and pharmacy,
Emma: Perfect. So, it's management like usual, no extra vitamins, but obviously we're always promoting everybody to have a healthy diet and vitamins, I would say vitamins are better taken in vegetables rather than pill form. And just being aware, you know what to look out for if they deteriorate. So, remember, if you're sending children home, be very clear with parents. Give them good safety netting. Make sure they know where and when to come back. There's always information on Healthier Together, which is the website, which is now almost national and has a centre in London. So, you can text parents direct advice about measles and about fever.
So, our patient was well, we gave them straightforward advice. We sent them home, but they obviously, they got their measles from somewhere, and they going to give it to somebody else. So, we have to think about contacts. So, what kind of advice? What do we need to do at that point when we think we have a suspected measles, because we might not have it come down at that point.Liz: So, did you know that 90% of unvaccinated contacts will get infected? Measles is so infectious, and a contact is pretty much anybody. So, it's anybody in the household, anybody you've had face to face contact with, and anybody who was in the room with you for 15 minutes or more. So that's a really low threshold for calling them a contact. It's a very infectious virus. But the most important thing, whether you're admitting the face to sending them home, is ascertain whether it's anybody who's highly vulnerable at home, and that would include pregnant people, infants under one year, who are both at risk of severe disease and are likely to be unvaccinated, and then anybody who's immunocompromised. And so, we'd really suggest that you ask families who is in their household and who they've spent time with, who might fall into those categories. And the good news is, we're not expecting you to do any contact tracing that you can then highlight that to the health team, because if they're in the middle of an outbreak, they get lots of referrals, and if you let them know that high risk person, they can prioritise that family.
Emma: So, if I'm sitting in a GP practice and I see somebody, I think this child might have measles, but they're relatively well. I would do a swab, an oral swab, I would give them some general advice about fevers, and then I would have to do some contact tracing, or better still, I could contact the Health Protection Agency. So how would I do that?
Liz: So, the Health Protection Team are unique to your locality, so there isn't one number for the country, but if you Google Health Protection Team UK, HSA, you will get a little box to put your postcode, and it will tell you how to contact your health protection team. At the moment, we're asking everyone to phone the Health Protection Team, because the numbers are not so high at the minute. And just to be clear, there is an outbreak, but it's not terrible, so it's manageable. If things get busier, it will probably become email contact Health Protection Team, but when you put your postcode in, they will know how busy their team is and will give you the appropriate recommendation to contact them, including a direct number.
Emma: So, you don't actually have to do anything other than ring this number and they will do it for you.
Liz: Yes, but you will make an immediate friend if you have the information to have, they are going to want to know. So, it's probably worth gathering back together before you call them. You will, initially probably speak to an admin operator rather than an actual health protection doctor, who will take details, including the name and address and contact details of the family and what your suspicious disease is, because they obviously take notifications for lots of things, but if you can then tell them who's in the household that you're worried, so there’s about pregnant lady who's 39 weeks, or there's somebody who's been on chemotherapy for six months, or there's twins under one, then actually that's really helpful for them in terms of prioritising their work.
Emma: Amazing. That's great. So, in our case, we had to do contact tracing for the whole of the emergency department, so all the people who were sitting in the room with a child with a fever and a rash. And so, this brings us on to a really interesting discussion. So, in our waiting room we ha, obviously, five children under one. We had some children who were waiting to have, who were having treatments and leukaemia and had come in with a fever, and we had staff members who were older who hadn't been vaccinated. So, Liz, let's think about what happens to all those contacts and what they need to have to keep them safe and stop them catching measles.
Liz: So, I’m a nerd so I love this! This type of thing, it’s like some kind of weird exam question where I get very excited. So, we know the highest risk groups are pregnant women, because they are at higher risk of severe disease, also stillbirth and premature labour. We know that under ones are at high risk of severe disease, so complications such as encephalitis which has been mentioned, are more common in that age group, and they haven't been offered a vaccine yet so are more susceptible. And then immunocompromised I'll come to in a minute, because it's a bit more complicated. So, for pregnant women, you don't need to do anything in a hospital setting, but the Health Protection Team will arrange for them to have human normal immunoglobulin in the community to boost their immune system. Actually, what they'll probably do first is get their booking bills checked and see if they have IgG, because sometimes people think they haven't been vaccinated and they have, and you have a few days to work this out, so that's what they will actually do. For child under one if they're under six months, we just give them human immunoglobulin. If they're six to nine months, it depends on the level of contact, they may either get human immunoglobulin, or if it's not a very close contact, we'd offer them a very early MMR. And if they're between nine months and a year, we give them an MMR. I don't expect you to remember that. It's on page 49 of the national guidelines if you want to go and have a look for reference. But the key thing to know is that if they get an MMR under a year of age, it doesn't count. And the reason for this, I think, quite interesting, and it's the reason why we designed a vaccine schedule, is that there may be maternal immunoglobulin around and the vaccine might not take properly. So, we will assume that vaccine has some benefit at that time as part of the protection, but we would want them to still have two doses at the normal time that vaccines are offered, which is the really key learning points there.Emma: So, if we're thinking about contacts, pregnant women will have human immunoglobulin in the community. Children under one, you need to think about whether they need treatment, but particularly under six months. So, they might get immunoglobulin under six months. The older ones might get an early MMR, which is a bonus MMR, and they still carry on with their normal vaccination schedule. And now we've got a tricky one. So, what about the child who is having leukaemia treatment, who's come in because they've got a fever?
Liz: This is really interesting, because humoral immunity, or your antibodies, are actually the protective mechanism here. So, things that you might have learned in terms of protection for other things are different when it comes to this immunocompromised. And there's two groups, group A, who might still have antibody, and therefore you don't need to worry about and group B, who don't have antibody, and you have to worry about.
Group B all gets IVID or immunoglobulin, and that will be given in a hospital setting, and through the specialist teams in pharmacy and Health Protection would call the paediatric team to arrange that. And for group A then you do talk to the Health Protection Team and do a risk assessment with them. So, this responsibility doesn't lie with you, but you may be involved in a conversation or discussion about it. And so, any child who has leukaemia or nephrotic syndrome on steroids or has had a transplant in the last year, or any kind of community modulation therapy is best check. Many of them may not need any post exposure prophylaxis, but we don't want to miss ones that do.Emma: Yes, and I think it's really interesting because they're a really big group now. So, you have to think about all the children on monoclonal therapy, children with severe inflammatory bowel disease, all the children with things like juvenile idiopathic arthritis. So, I think the key point here is what you said earlier, is take a good history, make sure you've identified them, and then get the advice from your paediatric infectious disease team, or the HPSA.
Liz: The other thing to know, though, is that the child who had two per kilo of pred for their asthma for three days doesn't fall into that immunosuppressive category. You have to have a reasonable amount of immunomodulatory therapy to be at risk. And so those are children that we wouldn't really worry about. If they were unvaccinated and made contact, we would probably just give them an MMR. It’s anybody beyond that that would be a worry.
Emma: Yes, that's one of those questions that we get all the time. So short courses of prednisolone, that's like less than a week, or one of courses of dexamethasone for croup, they do not count as immunosuppressive therapy. We've decided. We've rung the Health Protection Agency. We've sorted out the pregnant ladies and the immunocompromised children sitting in our emergency department. But Liz what about all the staff? Because they were going in and out of the same room where the child with measles has, so what happens to staff?
Liz: Yeah, so I think this is something that worries a lot of people, because particularly for the more mature members of staff who might predate the introduction of measles vaccine, or in particular, the non-normal healthcare staff. So, if you're a receptionist or an admin person, you might have a different occupational health pathway. So, I don't know if you know, but your measles serology was likely to have been checked when you started work with occupational health, and so you should be able to access that, and that should be universal, but I know that sometimes things are missed. And there was a really nice table in the national measles guideline, which has the years the vaccines were introduced, and when we think people would have had natural immunity from infection in it. And so, I had a single needle vaccine, so try and guess my age from that. I didn't get an MMR, I got rubella when I was an older teenager. And the other question that comes up on this is, ‘If I know my rubella status. Does that mean I'm definitely protected from measles?’ And the answer to that is no, because we used to give the rubella vaccine separately from measles. So, most healthcare staff should know their status.
The safest thing to do, if you're not sure, is just have a dose of the MMR and it's a live attenuated virus vaccine. And if you have immunity, your immune system will just wipe it out. If you don't have immunity, it will give you immunity. And it's really beneficial to have it. And so generally speaking, if you're not sure, that's the thing to do, but most people should have access to their information. If you have someone who you know is not protected through choice or circumstance, then they should not be looking after these children, and they should be kept away from them where possible and encouraged to do what they can to protect themselves, including. PPE.Emma: Thank you, Liz. Yes, originally you got a measles vaccine, then you've got measles rubella, and then eventually MMR. And I may have been in that category. We actually had somebody who actually remembers measles and getting measles. So, we have got people older than me, but only just and we did exactly what you said, and our occupational health team came down and gave everybody vaccinations, both at the time and opportunistically afterwards. So, I've just had my MMR, very recently. I had lots of aches and pains, exactly as you'd expect, but I won't get measles!
But I think the other thing that you alluded to, which is really important is, being really careful and protecting yourself from measles. So, about PPE and the need to have fit testing and wear masks, which seems to have completely gone out of fashion now. But I always wear a mask because when I'm in the emergency department, I am constantly seeing children with fever, rash and cough, and I have no idea what they have at the time I see them. So, what are your thoughts on this?Liz: I don't want to get a cold, so I'm happy to wear a mask around infectious children, whether I also don't want to get anything more serious. So, I didn't find the trend of wearing masks that onerous. However, just to be clear, the national guidance for PPE for me is also to wear an FFP3 three with eye protection, a gown, and gloves. And this may seem over the top when you know that you're vaccinated, but it has two roles. One is to protect you, just in case your vaccine didn't work, very unlikely, but you don't want to get
sick. And also, they might have something else which is worse. So, it's always good to be overprotective, rather than under protected. And then finally, you might still get a very mild version of measles and then become infectious and then continue the onward transmission of this outbreak. So the main role that you have as a paediatrician is to try and break transmission, and that is either through early identification and isolation, so preventing all these people in the waiting room being exposed by picking up a child, that you can prevent from becoming unwell through the post exposure prophylaxis. But also, by not becoming part of the entire transmission cycle yourself by wearing PPE.Emma: We always have to mention try and use tissues. Throw them away, cough in your arm and wash your hands I can't say this often enough. And you've got another hot tip for preventing measles or screening it early, don't you?
Liz: Yeah, so what we're suggesting, and I'm very unpopular with some people for suggesting this, is that we are really just on it in terms of those children and getting them into the side room quickly so that Emma and her colleagues don't have to phone 29 families who were in the waiting room and were exposed.
So, I'm not suggesting that every child with a fever and a rash has to go into a side room. That's just completely impractical. However, if you have a poster up signposting parents to things that they might want to consider, including, is your child vaccinated? Have you travelled to an area where there's lots of measles? And if you ask your triage staff or your reception staff to just ask those questions of children who present with a fever and a rash, are they vaccinated, or have they been in contact with some measles? You might be able to swiftly get them out of the waiting area and prevent having to do that extended contact tracing exercise. And it's a really simple thing to do. It's two extra questions for your reception staff and a poster, and it might just save a lot of time and effort, potentially a severely unwell, immunocompromised person.Emma: We probably should have asked this at the beginning, but I guess we just got into the clinical side of it very quickly. But why is there so much measles around now, what's happened to change things?
Liz: So, this is a really interesting story, and there have been measles outbreaks in the last 10 years, so in 2013 and in 2019. And then there's been a rise in cases over the last year because of global outbreaks in Asia and Africa, and because of poor vaccine coverage, which started in the pandemic and has kind of continued. And so, in the UK, our vaccine coverage just isn't as good as we'd like it to be. And so, the dose uptake in two-year-olds for the first dose was 89% and we really need that to be 95% and for two doses at 85%. And actually, where I work in London, it's as low as 60% in some areas. And this is a real worry, to be honest, and the reasons for that are multifactorial.
And you know, there are a subgroup of people who are still concerned about autism in the MMR, which is probably the most over investigated outcome of any vaccine that's ever been looked at. And I can confidently, hand, in fact, say that hundreds of 1000s of children have been analysed. The data from hundreds of 1000s of children show that there isn't link between autism. But actually, it's more than that, and there's a convenience and an access issue for many families, particularly for that second dose, where it can be really tricky to get out of your zero hours contract on a Thursday afternoon which is the only time your GP practice offers it. There may be a language barrier, there may be a cultural barrier. So, for some groups, it's just not acceptable in their communities. There are worries about pork in the MMR vaccine, and we have a really great pork free MMR vaccine called priorix, which is available in most areas. So, make sure that people are aware, they can get a pork free vaccine. And then the final thing is that, you know, all of the negativity about Covid vaccines has just shaken people's confidence in any vaccines, and so they're just all a little bit worried about vaccines in general. And I think we have a role as paediatricians to know a lot about vaccines so that we can confidently talk about them with patients and not judge them if they're not vaccinated. There are many reasons why people don't get vaccinated, and usually, if you just say, what is it you're specifically worried about? Can I point you to a really good resource like the NHS website or the Oxford Vaccine Group website? Many families go and read them and are quite happy to take the vaccines. They just needed somebody they trusted to be positive about going to give them accurate information, rather than whatever nonsense is on TikTok and Instagram, etc.Emma: I think it is a number of reasons that are really important. So, there was a slip in vaccination rates during the Covid pandemic because people just couldn't get there, and we haven't really caught that up. There is immigration from areas where there is less vaccination. So, we see a lot of people from Eastern Europe, for example, or from Russia or Ukraine, who just can't get hold of vaccines. And there is still some hesitancy about using vaccines, although, as we say, there's very, very clear evidence that there is no link to autism.
Liz: And so, one of the things that you know, if you're interested in a QI project, or something like that, that you could explore is whether there's any opportunity to do opportunistic vaccines where you work. So, UKHSA have a catchy MECC, which is, ‘make every contact count’. The idea there is that every time you see a patient to check their vaccinations, and if not, either offer to vaccinate them or signpost them to where they can get a vaccine easily. But we should be trying to do what we can, particularly in areas where vaccine coverage is low, such as London, West Midlands, to make sure that we're catching as many people, whether in front of us, as we can.
Emma: Yeah, actually in the Northeast, the vaccine level is really good for the first MMR, but not quite so good second dose, but it is better than other areas, which is one thing that we can be happy about. Opportunistic vaccination doesn't need to be difficult. So often if you see somebody on the ward just before they're about to discharge them. You can offer them vaccines. If they're coming to clinic for another reason and you happen to notice they don't have vaccines, that's another opportunity. And I think it's important to think about hard-to- reach communities. So, we're doing some really interesting work with the food banks and schools. So, I think that you need to look at your area and know what's happening in your area and how you can ensure that everybody gets the opportunity to be immunised, because it's a lifesaver. Literally.
[music starts]
This podcast is a collaboration between Odland, medical education and the Royal College of Paediatrics and Child Health. You can find more creative learning resources and a wealth of information on the important work of RCPCH on www.rcpch.ac.uk or #ChoosePaediatrics.
Emma: The views, thoughts and opinions expressed in this podcast relates only to the speaker and not necessarily to their employer, organisation, the Royal College of Paediatrics and Child Health, or any other group or individual.
[music ends]
-
Episode 9: What you can do for sustainable healthcare
The NHS has a large carbon footprint. So how can we as child health professionals help lower the environmental impact of delivering healthcare? Today’s guest on The Paeds Round, Dr Emily Parker, RCPCH Clinical Fellow and paediatric doctor in Newcastle speaks with host Dr Emma Lim on how we can all make a difference.
Emily and Emma discuss the surprisingly high carbon footprint of liquid medicines, how to optimise asthma care to reduce medication use and the benefits of dry powder inhalers over metered-dose inhalers. They also look at how to advocate for better air pollution management, which help prevent diseases like asthma.
Dr Emily Parker is RCPCH Clinical Fellow with the Clean Air Fund Partnership and a Paediatric Junior Doctor at the Great North Children’s Hospital in Newcastle.
[music, with snippets]
Emily: The problem feels really big, but don't let that stop you from starting somewhere
Emma: When something is so big, it's hard to see where your place within it lies and what you can do. And I think it's really surprising to me that, like almost a quarter of the NHS carbon footprint is just medication.
Emily: The problem with carbon foot printing is it often encourages us to focus on products and not think so much about diseases and how to care patients better.
[music ends]
Emma: Hello and welcome to the Paeds Round, your official podcast from the Royal College of Paediatrics and Child Health. My name is Emma Lim, and I'm a consultant paediatrician at the Great North Children's Hospital.
And on today's podcast, we will be discussing why sustainable healthcare is an issue, and why we all need to be not just interested but engaged in it. I'll be talking to my guest today, who is Dr Emily Parker, who recently completed a sustainability fellowship at the Great North Children's Hospital and is now the Royal College of Paediatrics and Child Health clinical fellow with the Clean Air Fund partnership. So welcome Emily. What a lot of titles and do you want to introduce yourself in a more friendly way?
Emily: Hi Emma. Thank you so much for having me on the podcast. I'm really excited to be here. I don't hold all those titles. They're just jobs I've done, but I seem to be the eternal fellow because of the interests that I have outside of medicine. So, these jobs have enabled me to carry on practicing as a doctor, while pursuing my interest in sustainability,
Emma: We ought to get the conflict of interest out early on. I have to say that I was your supervisor in the year that you were a sustainability fellow at the Great North Children's Hospital, and which was a project that was inspired by Dr Mike McKean, who is the current vice president of the RCPCH, and also you were supported by the Centre for Sustainable Healthcare.
Emily: Yeah, yeah. It was great to be supervised by you, Emma and amazing that Mike managed to get that project through our charity funding and Newcastle hospitals.
Emma: And actually, I do credit you with making me so much more aware of ways that I could make a difference. Because I think it's very easy to get sucked into the day to day running of the hospital and looking after your patients, and not having time to think about these really important, bigger issues.
Emily: That’s really interesting that you hadn't thought about previously. I think I share that as well, actually, that it was the sustainability fellowship that has really inspired me to apply my understanding of the environment and its importance to my work as a doctor. So, it's a journey that we've been on together as well, to some extent.
Emma: That's nice. That makes me feel part of it. And I think one of the big targets you always talk to me about was the NHS Net Zero strategy. Do you want to explain a bit about this?
Emily: Yeah, so the NHS was the first healthcare system to enshrine its net zero policy into law, and that happened under Health and Care Act in 2022 and there is a greener NHS organisation that sits within NHS England that's responsible for implementing Net Zero. And that covers the entire system of the NHS. So, it includes buildings, transport, energy, and then all of the things that happen within the clinical pathways that we do, so the medications we prescribe and the machines we use, and then all of the administrative side as well. So, it's a huge area of work to try and reduce the environmental impact of that system.
Emma: And I think when something is so big, it's hard to see where your place within it lies and what you can do. But one of the things that you explained to me is that medicines and medicine prescribing is a huge part of the carbon footprint of the NHS.
Emily: Yeah, so medicines. So, there's a really interesting graphic that Greener NHS has produced, and even if you just Google Net Zero NHS, you'll find this graphic. It's green and blue, and it's a pie chart that shows different parts of the system and their contribution to the carbon footprint. And medicines on that graphic, take up 20% of the carbon footprint, medicines and chemicals. And then there's a separate part for inhalers and anaesthetic gasses, which is another 5%
Emma: And so, I guess that was one of our projects where we thought about the difference between prescribing pills and prescribing liquids, and the effect that that could have on that 20% of the carbon footprint. So, tell us about that.
Emily: Yeah, so we were thinking a little bit about what we can do as clinicians and where our areas of influence lie, and you'd already undertaken this really interesting teaching program helping children to learn swallow tablets called KidzMed, which I think members of the College might already know of because it's being promoted through the College. And one of the areas of KidzMed that hadn't really been looked at in detail was the impact on the environment, but we had a kind of hunch that there might be some significant differences between tablets and liquids, partly because the cost of them is already so different, and that suggests that the processing might be quite different chemically. So, we wanted to try and investigate that. So, I undertook a project looking into it.
Emma: Go on then, are you going to tell us the results? What happened?
Emily: So, we started off looking at the most obvious thing to us, which is the packaging. And I think the process of this project was quite interesting for all of the team to look at, because it represents a common error that we all make when we think about sustainability, which is to focus on waste and the stuff that we can see ourselves throwing away. So I started by weighing the packaging out and working out how much carbon each piece of packaging represented, and we found that there was already quite a big difference between tablets and liquids based on the packaging. That liquid bottles, with all their packaging were about three times the carbon footprint of the small packs of tablets, which, if you think about what's in them, you can imagine that that might be the case. But then actually what happened after that was that we combined our project with YewMaker’s results.
Emma: Well, it's a perfect time to talk about this, because YewMaker is a company which has just very recently published the online formulary, so that in exactly the same way as if you use the BNF, you can look up the price of different drugs. You can now use the YewMaker formulary, to look up the different carbon footprint of drugs. And this is all the brainchild of Dr Nazneen Rahman, who got in touch with us.
Emily: Yeah, she got in touch via Twitter. You just reminded me of that. That was how we collaborated with her, and we can thank the College for that, because I think she got in touch with me or you on Twitter after we presented our initial findings at the College, and we'd maybe tagged her in something or something like that, so it's a good story! But she basically was very kind and shared some of her results with us about the carbon footprint of amoxicillin, so the molecule that goes into the drug of amoxicillin, which is the drug that we chose to look at for our packaging. And we were astounded when we looked at the results that she had compared with our packaging carbon footprint. And I think we had to recheck it about 10 times because we couldn't believe that it was so much more than the carbon footprint of the packaging. So, what I was talking about earlier is this story of focusing on the things you can see and forgetting about the things you can't see. And actually, once we looked into the things we couldn't see, we realized that it was much more important to care about drugs wastage than to think too much about the packaging when we're talking about carbon footprint, if that makes sense.
Emma: Thank you, Emily. And I think it's really surprising to me that like almost the quarter of the NHS carbon footprint is just medication, and that means we've got to think so much more about how we prescribe. So, we wanted to look at this in a real-world scenario. And we looked at the example of prescribing a course of amoxicillin child with a sore throat and tell me what you found out just looking at that real world example.
Emily: So, it was really interesting starting this project off, because we tried to find any research that compares liquids and tablets and looks at the carbon footprint. And I think there was one study that was done in India looking at paracetamol, but it was done on a huge scale, and it wasn't actually done by clinicians. So, we were the first clinical team to try and do this that we're aware of. And what was really fascinating to me doing this research is that you initially focus on the packaging, because that's the waste that you can see. But when we applied this clinically, what we found was that tablets allow you to prescribe very specific numbers and to adapt that to the course that you're prescribing. Whereas bottles are extremely difficult to divide up and we can't do it. So, when you prescribe a course of amoxicillin with bottles, you have to prescribe three bottles for the child that we looked at in our example. So that's 10 doses in the first and second bottle that she would take over a 21-dose course, and then for the final dose, she needs a whole bottle just for that final dose. And you probably would find that maybe the parents would pour nine doses in the final bottle down the sink or give it to a friend who probably hasn't been prescribed it.
Emma: So that's really fascinating. I think this is a really common problem that we prescribe liquid medication, and we don't really know what people do with the bit that's left over. So, you were saying that quite a lot might be left over. And I think another of my trainees looked at that and found on average, with six different types of antibiotics, that half the bottles were left over at the end of the course. And that leftover medicine, like you said, either gets tipped down the sink, which obviously is putting antibiotics into the water, increasing the risk of antimicrobial resistance, or it sits around on the shelf and then somebody decides to use it because it might just help somebody else who's ill, or the child again, so that's inappropriate use, and again, risks antimicrobial resistance. Or they return it to pharmacy. But quite honestly, I have four children, and I've never returned anything to pharmacy, and the only time I tried it was the EpiPens, and they refused to take them.
So, we've talked about the wastage of that medicine compared to giving pill doses. Could you put any figures on that in terms of carbon footprint and money?
Emily: Our project focused on the carbon footprint, and what we found was that in a 21-dose course of 250 milligram doses of amoxicillin, the final bottle, you waste nine doses, and those nine doses are equivalent to about 6.6 kilograms of carbon, and that's the equivalent of driving a small car 99 miles, which would get you from Newcastle to Edinburgh. And that's just one course of antibiotics for one child.
Emma: Yeah. And overall, we found that liquids were, on average, 40 times more expensive than pills for the same dose. So, there's a huge difference in cost, and we were just looking at antibiotics. So, what would your recommendations be then? Knowing what you know now, how has that changed your practice?
Emily: I think it made me think a lot about the communication between doctors and pharmacists, because I imagine that pharmacists are very well aware of how much is wasted in the final bottle and have been for a long time. So, we probably really need to facilitate a conversation when we're prescribing that allows pharmacists to come back to us and say, ‘Are you sure you want that last bottle? The patient's only going to be using one dose of it’. And I guess we also probably need some help from our Infection Control colleagues, of which you’re one, Emma, so maybe you can provide some guidance on how we might dose antibiotics if there is just such a small amount needed from the final bottle of liquid.
Emma: Yeah, thank you. And I did a really nice project with Joe Pickles, who is one of our medical students, and he looked at the antibiotics, and he found, on average, 50% of 100 mil bottle is wasted for every course of antibiotics. And that financial cost is £2 per course. And as I said, the liquids cost a lot more. And we had a couple of recommendations. First of all, as you say, work with your pharmacist, and the most obvious thing was to use an IT solution. So just to put the pills as your first choice when you prescribe, most people are using electronic prescribing. Most people click on the thing that's on the top. So, make the first-choice pills. The second thing that we thought about is just thinking whether it makes a huge difference, whether you can have 20 doses rather than 21 which we know wouldn't make any difference. But that has to be a system change. And we considered talking to the people who make the guidelines. So, thinking about contacting the British Paediatric Allergy and Immunology Group to see if we could change national guidelines. So that's a system level change.
But also, some really simple things, like some bottles like flucloxacillin, actually not flucloxacillin as it’s so disgusting. Nobody should ever prescribe flucloxacillin liquids. It should only be prescribed as tablets, because it tastes so bad. So, I'll take a different example. We're talking about amoxicillin, which comes in two strengths. So, it comes in 125 milligrams per mil and 250 milligrams per mil. So, if you chose the strongest strength for younger children, you might manage to use less bottles. So that was a really simple thing.
And finally, to engage with industry and get them to give us antibiotic liquids, because you do have to use it as very young children in bottles with smaller amounts in. So, azithromycin is a really good example when they have 15 mils and 30 mil bottles, not just 100 mil bottles. So that reduces your waste a lot.
Emily: I think the really important message to get across there is all these complicated solutions are unnecessary if we can teach children to swallow tablets from a very young age. And using KidzMed that solves all of those messy, kind of difficult aspects of changing the prescribing of bottles and changing the strength of solutions, which would be important. But when children can learn to swallow tablets, we then have a box with 21 tablets that fulfils the course, and there's no wastage, and the parents can't give it to them in two weeks’ time when they think they're unwell again, and it doesn't sit around in the cupboard or go down the drain.
Emma: No, I completely agree, and I'm constantly surprised and depressed by how many children don't know how to do it. So, I was on call last week, and there was eight-year-olds and 12-year-olds who couldn't swallow pills. And I think that we know that we can teach children from the age of four, and one of the system level changes we're looking at is seeing whether we can get children to learn this skill through school, because it's exactly the same as learning to ride a bike. It's a life skill. It's something that we all need to learn. And so, we're working with a group of pharmacists in Liverpool in Alder Hey Hospital to see if we can do a much bigger project to introduce it into the school curriculum, which would be something I'm really keen on.
However, obviously, it's not all about pills, although, you know I'm passionate about that! And you talked about inhalers and anaesthetic gasses being 5% just by themselves of the NHS carbon footprint. And I know there is a huge amount of work about inhalers, so talk to me about our choices of inhalers, how we dispose of inhalers, what we're going to do with all these inhalers and asthma medication?
Emily: Okay, so there's been a big focus on inhalers in NHS Net Zero strategy, and that's because they're considered to be a carbon hotspot, which means that it's, I guess, a small part of the system, but a huge part of the carbon footprint. The reason why inhalers, metered-dose inhalers, have such a big carbon footprint is because they contain gasses which are very potent greenhouse gasses. So, in order to deliver medication to the patient's lungs, these gasses get released and they are environmentally not good. So, there's been a big drive to try and use dry powder inhalers instead of metered-dose inhalers, because the dry powder inhalers have a different way of delivering the drug, and that's through the patient breath power sucking the powder into the lungs.
Emma: So that's a really important point. It's better to use dry powder inhalers than metered-dose inhalers, because then you're not having the extra gasses and cannisters within it.
Emily: Yeah. They don't contain these potent greenhouse gasses at all, they just contain the powder.
Emma: So, this is really important. We're talking about asthma medications and the different choices you can make and how dry powder inhalers are better than metered dose inhalers, but they all use quite a lot of quite a lot of plastic and metals. So how do we try and reuse, recycle and maybe later on, we'll talk about reducing the use of them altogether.
Emily: Well, it's a big question. I think all inhalers are quite complicated to recycle. Dry powder inhalers are actually a bit more complicated to recycle than metered-dose inhalers because they're a more complicated design using different plastics, metered-dose inhalers, you can remove the canister, recycle the plastic, and then capture the gas left in the canister, and it can be processed and sold for non-medical uses, as these gasses are actually quite valuable. But it's quite a complex system that is needed to do that. And there are some programs that exist, run by Grundon. And actually, there was a really good presentation at the Royal College of Paediatrics Conference that talked about inhaler recycling project that's been undertaken in London, and that was by one of the members of the Climate Change Working Group.
Emma: So that's really interesting, and I think that's a really important thing, that we sometimes do have to prescribe metered-dose inhalers, and that we really need to be better about trying to recycle them and using these new systems and developing them within our hospital.
So that's great. We've talked about how much more important it is to recycle metered-dose inhalers, but actually what we really need to think about is how to optimise asthma care, and how will we go about that?
Emily: I'm really glad you asked me this question Emma because I think the problem with carbon foot printing is it often encourages us to focus on products and not think so much about diseases and how to care for patients better. So, when we think about inhalers, I think it's really helpful for us to actually think about what diseases are we trying to treat, and how can we make these patients live better lives and have less disease.
So, one of the things we can do is within asthma care, we can make sure that patients are taking their steroid inhalers and are appropriately prescribed steroid inhalers. And I think in paediatrics, that can be quite difficult, because we have lots of children coming through, young children with viral induced wheeze who get given a blue inhaler, and they go home, and they probably end up staying on it with their GP, who repeats the prescription. But they haven't really been given good advice about when to take it and when not to take it. They've just been given a reducing course when they leave hospital. So, I think one of the things we can do as paediatricians is think really carefully about those children and how they get followed up. Do we see them all when they're five and decide whether they've got asthma or not, and if they haven't, do we just stop inhalers? And then make sure that those who have asthma do get steroid inhalers and have their disease really well controlled. So that's step one. But I think we can go a little bit further.
Emma: I think this is a really good point that actually the best way of reducing the amount of asthma medication you use is by having really well controlled disease. So, if you think about really well controlled asthma, you're taking your regular medication, and you're not taking so much of those short acting beta agonists.
But the other thing to think about that you touched on is, all the children where they haven't necessarily had a diagnosis of asthma and how they get followed up and how their care is really focused on. So, I think that's a new area that we're much more aware of. And I know that on Beat Asthma, there are new guidelines for viral induced wheeze in children when they're too young or they don't have a full diagnosis of asthma, so very, very important.
But if we think beyond that, so we've talked about the drugs used for asthma, we've talked about good asthma care, but we haven't yet got to the root of the problem, which is, how do we stop people getting asthma? What can we do in a greater sense, other than giving medication?
Emily: Yeah. And I think that’s especially interesting from a sustainability perspective if we take this approach of looking at the disease rather than looking at the products of healthcare. So, we don’t look at the product being the inhaler, but we actually look at the patient and their disease. Asthma kind of represents an environmental illness, and it encourages us to really think about how the environment affects patients. And that’s what’s really lead me on to the next role that I took after my sustainability fellowship, which is what I’m doing now. Because when I was looking at inhalers and finding it quite difficult to think about how to implement these changes, especially in paediatrics, where prescribing dry powder inhalers can be challenging with young children. I started to think more about what can we actually do, and I almost got a bit frustrated thinking about these products. Because all the causes of asthma, or a lot of the causes of asthma, are actually preventable. And we can do so much more to try and stop people from getting asthma. When I started to read the evidence, I was shocked that we knew that air pollution was causing asthma since the 50s and 60s really.
Emma: So, I think that’s a really, really interesting point that you bring up, that almost all diseases, while they have a genetic susceptibility which you may not be able to change, there are also environmental triggers. And this is true in so many diseases, but what you’re talking about in asthma is the huge part that air pollution plays in making this a disease of our current climate.
Emily: So, I guess that’s made me into a bit of a public health paediatric doctor because it’s really enthused me on how we solve the problem of the NHS carbon footprint on a slightly bigger scale. And I think it’s made me think about this image that you can see of pie chart and Net Zero, and how that image doesn't really talk about patients. And I think we really need to be keeping our clinical hat on and keeping our patients in mind when we're trying to solve this problem, rather than just thinking, ‘Oh, we mustn't waste’. When we think about the how, we need to think about making people well and basically making our role not needed anymore, or at least only needed in very extreme circumstances, and that we have a healthy population.
Emma: Yeah, really interesting. So, I guess there's a parallel between fast food and obesity. So, you're talking about clean air and asthma, and not just asthma, all respiratory diseases. What kind of things can you do to promote clean air or to help your patients?
Emily: So, we're actually working very hard on this at the moment in the College trying to develop some really good advice specifically aimed at paediatricians, at children and at their families, in how to make changes that are going to reduce exposure to air pollution, but also potentially reduce contributions to air pollution.
But there are things you can do, so simple things like when you're walking to school with your child, that you put them on the side of the street that's furthest away from the cars, and that you choose routes that go on the back streets, so not on the main roads. Children are very vulnerable to air pollution because of their height, so they're often almost at the level of a car exhaust, and also because of how they breathe, their metabolism is different. They breathe faster, and they take in more pollutants per volume, per body mass, than adults. So, actually their cells are being more exposed to the pollution.
And then I guess closing your windows on high pollution days is another piece of advice you can give to patients, and those who really suffer from severe asthma there is advice that they shouldn't be outside exercising on high pollution days. But I find these pieces of advice difficult, because what we're asking people to do is avoid nice things potentially, and I think we need to be doing more to try and reduce pollution. So potentially, even within a hospital system, as a clinician, you might be able to influence your trust to help with things like active travel, to stop cars idling outside the hospital, and to implement the Clean Air hospital framework, which is something you can look up that was developed by Global Action Plan, and gives a number of points that hospitals can follow to make their hospital better for air pollution.
Emma: I'm really glad you have such big ambitions. And I guess that's really interesting, that you moved from a small thing, which is just describing something differently, to trying to change like government and high-level policy on what happens.
I think in practical terms, it is important. One of the really kind of demoralising things that was happening in our hospital was, our outpatient department faces right out onto the street, and it's exactly where all the smokers go to smoke. So, they come out of the hospital, and they all congregate just outside the children's outpatients to smoke. So, they had a whole program of trying to remove them or move them to a different place. They've done a lot. First of all, they put all this advertising campaign, and it was really clever, because they put lots of pictures of children holding signs saying, ‘Don't smoke I'm just inside’, which actually was, I think, quite impactful. They also put a fruit and vegetable stool very close to the outside of hospital, so it's not really a place you would try and smoke, and everybody's watching you. So, whilst they haven't reduced the smoking, they have moved it away from the children's outpatient area, which I think is very positive. And I think that everybody can be thinking about things like this in terms of what happens outside the hospital.
Emily: Yeah. And to add to that, one of the things I noticed in Newcastle is that the Children's Hospital is right by the main road, and when they implemented the clean air zone in Newcastle, the parameter road of the clean air zone goes past the hospital, which I presume means that all the polluting vehicles who can't drive through the clean air zone could potentially use the road that goes past the hospital as their route to avoid the clean air zone. And I wish that I had been on the ball with this and got some air pollution monitors so that I could have shown pre and post levels of air pollution and argued that it was a bad policy decision to make the cars drive past Children's Hospital.
Emma: That's fantastic, Emily. I mean, we've talked about so many big topics, from making every dose you prescribe count, thinking about how you prescribe, both in terms of pills versus liquids and in numbers of doses. Thinking about whether you actually even need to prescribe that antibiotic, thinking about asthma care, and good disease control, as well as how you recycle and reuse your inhalers.
And then, on a sort of system level, thinking about advocacy and the importance of just being healthy and making our surrounding healthy. So, promoting clean air, being ambitious, thinking about not just solutions like walking on different routes and closing the windows, which is, as you say, going around the problem, but tackling the problem head on by trying to reduce pollutants, reduce cars, stop smoking. So, these are really, really big problems. So, I'm going to ask you the most difficult thing, which is to give us your top tips.
Emily: So, three top tips for clinicians in paediatrics who want to do something about sustainable healthcare. The first tip would be to think about where your power is. So, think about your spheres of influence. And there's a really interesting diagram that shows personal sphere, work sphere, organisational sphere, and they get bigger and bigger. So, what's your biggest sphere? Aim for that level if you can.
My second tip would be that the problem feels really big, but don't let that stop you from starting somewhere. So even if that means that you decide in the morning huddle that you're going to have some kind of sustainability related piece of information that is shared by the group of clinicians that morning. That's the start, and once you start, you'll feel more positive about the future.
Emma: I love your idea about the spheres of influence. And obviously the Paeds Round our podcast is a huge sphere of influence. We would ask everybody to listen and share the Paeds Round, because that will make your sphere of influence bigger and share learning. And I would also say to other people, particularly other people who are passionate about sustainability, come and find me, ask me, and I'm happy to do more and share their learning.
I think that your point about taking baby steps is really important. Small things matter, and we do one minute learning. So, every time I do a handover, at the end of handover, I try to do one minute learning. And it might just be something like you say, actually think about air pollution, it's really important. Listen to this podcast! So, I think that these things make people think about what's important, and you’ve still got one last top tip.
Emily: You can have it!
Emma: My last top tip is obviously prescribe pills, not liquid! And teach all children over the age of four how to swallow pills, because it's a life skill that matters.
Emily: That's a great tip. You can have it.
Emma: It's been a real pleasure to have you. And thank you very much. I'm sure we'd love to speak to you, maybe in a year's time when you've fulfilled some of your huge ambitions, or to talk to some of your colleagues as well! So, thank you very much Emily Parker.
Emily: Thank you, Emma.
[music starts]
This podcast is a collaboration between Odland, medical education and the Royal College of Paediatrics and Child Health. You can find more creative learning resources and a wealth of information on the important work of RCPCH on www.rcpch.ac.uk or #ChoosePaediatrics.Emma: The views, thoughts and opinions expressed in this podcast relates only to the speaker and not necessarily to their employer, organisation, the Royal College of Paediatrics and Child Health, or any other group or individual.
[music ends]
-
EPISODE 10: Protecting infants with the maternal vaccine for RSV
Respiratory syncytial virus (RSV) is very common and can cause disease ranging from mild upper respiratory tract infections to bronchiolitis, pneumonia or even death. In the UK, intensive care wards in the winter are extremely busy and 20,000 to 30,000 children are hospitalised with RSV each year. This is a disease that causes a huge burden in infants both in the UK and globally.
Dr Simon Drysdale, a consultant in paediatric infectious disease, joins our hosts Dr Emma Lim and Dr Chisto Tsilifis to discuss the maternal RSV vaccine, which has been rolled out across the UK, plus advances in research and other recently licensed vaccines.
RCPCH had a significant role in ensuring the RSV immunisation programme was introduced in the UK following publication of the JCVI's recommendation to develop one. In March 2024, we published an open letter signed by over 2,000 members urging the UK Government to implement a full RSV immunisation programme for both infants and adults across the UK. Our letter generated media coverage and UK parliamentary attention with MPs and Peers supporting our calls. As a result of our campaign, we welcomed announcements from all four UK governments confirming the rollout of new RSV programmes for infant protection from August 2024 in Scotland, and September for Northern Ireland, Wales and England.
Dr Simon Drysdale is Consultant Paediatric Infectious Diseases Specialist at Oxford Children’s Hospital and a Senior Lecturer in Vaccinology at the University of Oxford.
[Music starts]
Simon: Around 100,000 infants a year die globally due to RSV, of which the vast majority are in low and middle-income countries. But in the last few years, obviously, there's been major breakthroughs. The vaccine seems to work in a real world setting as well as it did in the clinical trials.
[Music ends]
Emma: Welcome to the Paeds round, and we're recording a new podcast this week on a topic that is very close to my heart, both as a general paediatrician and as an infectious disease specialist. And it's my great pleasure to have a real expert in the field, Simon Drysdale to come and chat to us. So, Simon, would you like to introduce yourself?
Simon: Thanks, Emma, thanks for inviting me. So, I'm Dr Simon Drysdale, a paediatric infectious diseases specialist at the Children's Hospital at Oxford, and a senior lecturer in vaccinology at the University of Oxford.
Emma: Perfect. And today, this is very appropriate, because as I was driving along, on the news, it said that we've had a really bad winter. All the beds are full. We've got a lot of RSV, or respiratory syncytial virus around. So why is RSV such a problem, and why do you think that we should have introduced vaccines for it?
Simon: Thanks. So, hopefully everyone will be aware RSV, or respiratory syncytial virus, is an extremely common virus. Every child gets infected within the first two to three years, and it causes disease ranging from mild upper respiratory tract infection through to more severe disease, such as bronchiolitis or pneumonia, or even in some cases, death. We know that, as you just alluded to, as general paediatricians we know during this time of the year, A&Es are completely full, the wards are full. Intensive Care Units are full. We end up having to cancel elective surgery, because there are no beds, and the overall healthcare sort of burden is massive.
And I mean, just to put some numbers on that, in the UK, somewhere between 20 and 30,000 infants are hospitalised each year, and that's around 1 to 2% of all babies born. And there's many hundreds of infants admitted to the intensive care unit, and there are hundreds of thousands of GP admissions. To put into the sort of slightly wider context, around 100,000 infants a year die globally due to RSV, of which the vast majority are in low and middle-income countries, and there are 10s of millions of infants with lower respiratory tract infections and those that end up in hospital. So, this is a disease that causes a huge burden in infants in the UK, but also globally.
Emma: Fantastic, yeah, and I think I have this theory. I have a theory that viruses are like a second-rate relation. Everybody is very focused on bacteria. We've got lots of choices of antibiotics and immunisations have typically focused on bacterial infections. But what we see in the population, as you describe, is this huge burden of viral disease now.
Simon: Yes, and you know, we've known for a long time that viruses have potentially caused the biggest burden of disease. They circulate regularly. Everybody gets RSV every couple of years, but it generally tends to be less severe once you get past infancy, until you get to older age groups. And so, we've been looking for a vaccine for RSV for many years, since the 1950s when it was first sort of identified. And there have been various sort of ups and downs over the various years of trying to develop a vaccine. But in the last few years, obviously there's been major breakthroughs.
And so, in the last two, two and a bit years, we've had three vaccines licensed for older adults, one licensed for pregnant women, aimed at protecting the infants, and also a long-acting monoclonal antibody called Nirsevimab, which has been licensed to protect infants, and of course, we've had Palivizumab, the sort of short acting monoclonal antibody, for many years. But the downside with that, was it required monthly injections and was very expensive, so it wasn't really suitable for most infants. So, there's been an explosion of preventative therapies for RSV in the last couple of years, and now we're in the process of trying to roll those out across the UK and other countries.
Emma: Really exciting. So as a paediatrician, I'm not interested in the three for older adults. Why did you target pregnant women to vaccinate them rather than vaccination that could be introduced within the routine schedule?
Simon: So, there's a few kinds of reasons for that. I mean both approaches are perfectly reasonable, and the monoclonal antibody is designed to be given essentially at birth and therefore provide protection from birth. And likewise, the maternal vaccine given to the pregnant individual, they mount a response to the vaccine, and then you get trans placental transfer of the antibody to the baby, and so, the baby is therefore protected directly from birth.
Emma: Your idea is that you would vaccinate a pregnant woman, they would mount a response, and that immune response would cross the placenta. And so, a baby is born immune. It's like hitting the ground running. So, from the moment they're born, they are immune to RSV, is that correct?
Simon: Yes, yes. And there are other examples, influenza vaccine for pregnant women, COVID vaccine and pertussis vaccine, particularly pertussis is a good example. The vaccine is given to the pregnant individual, not so much to protect them, but the antibody goes across, and therefore the baby is protected immediately when they're born, rather than having to wait for their first vaccine, which would be two months of age, for example.
Emma: And that's really important, because babies die in that first month from respiratory illnesses like RSV and whooping cough. So, tell me, this year in September we were due to roll out the maternal RSV vaccine?
Simon: Yeah, yes. So, the vaccine program started in the middle of August in Scotland and the start of September in the rest of the UK. Obviously, the decision to start the program was made relatively soon prior to that. So does mean everything's been done at a fairly fast pace. So therefore, probably, as expected, it's taken a little bit of a while for people to be familiar with it, to be familiar with what RSV is, because it's not the most well-known virus outside paediatric circles. The delivery of the vaccine through primary care and obstetric and midwifery services, again, takes time to build up and for staff and patients and pregnant women to be familiar with it. So, at present, around 100,000 pregnant women have been vaccinated so far. Clearly, there's scope for things to improve. But overall, it's not so surprising, for a new program that was started fairly quickly that there are some teething problems. But one would anticipate over the coming months and future seasons, and things will improve.
Emma: Okay? So really exciting. So, we started in August, it’s September, and you can get the vaccine from their GP or from their midwife. How far along in their pregnancy should they be to get this vaccine?
Simon: So, the vaccine is recommended from 28 weeks gestation right through to delivery. The advice is, the earlier or closer to 28 weeks that women receive the vaccine, the better chance there is to mount a response and therefore pass on as much antibody to the baby as possible and therefore provide the most protection. But even receiving it later in pregnancy is more beneficial than not receiving it at all.
Emma: So, let's say you're like me, and you work on a last-minute basis. When is the last effective time a woman can get vaccinated for RFC in her pregnancy?
Simon: So, the vaccine takes around two weeks to take effect, let's say. So, if the woman is vaccinated less than two weeks before the baby is born, then certainly the response is going to be less than ideal. So ideally you want to be vaccinated at least two weeks before the baby is born, but preferably more than that.
Emma: So, what are the pros and cons of vaccinating mothers rather than babies?
Simon: So, the advantages, if I start with those, it’s obviously one less vaccine for the baby who already has many vaccines in the first year or so of life. It's definite protection straight from birth. So, unlike the monoclonal antibody, where there may be a bit of time before the baby necessarily receives the injection, where they'll be vulnerable. We know that if mum has received the vaccine, the baby will be protected directly from birth. There's also the advantage that the pregnant woman will receive protection from the vaccine. So, whilst that's not a big burden of disease, it certainly has some advantages and perhaps may even reduce in some reduced transmission in households, although we don't know that for certain. Programmatically, it's a little bit easier. It's a year-round program, so pregnant women are vaccinated all year round, whereas a program for infants probably would be seasonal, which is a little bit trickier to do from an NHS perspective. And then the last thing is, it probably is cheaper to have the vaccine than the monoclonal antibody.
Emma: A vaccine protects mother and the baby and possibly reduces transmission for the whole family, and that you can give it any time of the year. But there must be some downsides. There are always downsides. So, what are those?
Simon: Yes, so as you've already alluded to, if the baby is born prematurely, then there's little protection, or potentially no protection for the baby. And of course, this is a fairly new program, so there'll need to be ongoing surveillance for any adverse outcomes that are rare.
Emma: Okay, but exciting times, and I know that you know, we're always a little bit behind on the vaccine front. So, there are other countries who are already using it. Has there been some exciting news from other countries, the United States of America, Australia or Argentina?
Simon: So last season, several countries started using the maternal vaccine. In particular, Argentina rolled out their program for the last RSV season, and they've recently published some real-world data showing efficacy that was similar to that found in the clinical trials. So that's reassuring that the vaccine seems to work in a real world setting as well as it did in the clinical trials.
Emma: So, I think that means there were less admissions, less admissions to hospital and to paediatric intensive care, and also there was a nice effect that older people were also protected, or there were less emissions in the elderly. Is that right?
Simon: So many countries also rolled out an older adult vaccine program, much as we have just started in the UK. So, there's again, good, real-world evidence from the US that there was significant protection for those older adults who received the vaccine. So again, encouraging that in a real-world setting, what they found was similar to what they found in the trials.
Emma: Alright, and so one of the other things that people ask, so we we've got this fantastic new vaccine, we know it's worked in other places, so we've got some real-world data that's really exciting. I guess one of the questions was, does it affect babies’ immune response to their routine vaccinations? So, if you had maternal priming, if you were already immune to an RSV and then you had your routine vaccines, which you have to mount an immune response to, is there any problems?
Simon: So, there's no evidence that infants born to mothers who've received maternal vaccines have any significant impact on their routine vaccines. And all pregnant women will pass on RSV antibodies to their baby, because they will have had RSV previously. So, the purpose of the vaccine is to boost that response up.
Emma: So, they’re going to give them antibodies anyway, but they're just going to give them better quality antibodies because of the vaccine.
Simon: Exactly, better quality and more of them.
Emma: Fabulous. So, is there any problem persuading mothers to get vaccinated, or what's your experience been of persuading pregnant mothers to get vaccines?
Simon: Well, I think the evidence suggests it's still pretty early, and there's no hard and fast evidence available at the moment, but as I alluded to, more than 100,000 women have received the vaccine so far, which suggests reasonable uptake. We're still waiting for the final figures on that, but I think it's been pretty well accepted overall.
Emma: Yeah, I think it's a really great idea, because you know that women are coming for healthcare, and this is a preventative health, so they've got to come to receive antenatal care, and so you're actually doing something preventative. So, I really like the idea about this.
We've talked about maternal vaccination, we've talked about the pros and cons. We've talked about why it’s good. We've talked about how it's worked well in other countries, and that we all should be doing it, but let's say there are a population of children who are very at risk of RSV, and once they're born, you can actually vaccinate them, and you were telling me there were two different monoclonal antibodies. So previously, we've used palivizumab, which is a short acting monoclonal antibody that only lasts for a month, so the poor children have to come back and be vaccinated every month. But there's something new, isn't there now? What's in the bag?
Simon: So, the new monoclonal is called Nirsevimab, so it's a long-acting monoclonal antibody, so one dose at the start of the season will cover for five or six months, and that's been licensed, but at present, is not currently available in the UK. It has been used in other countries, and there's good evidence of real-world effectiveness, but it's not available in the UK.
Emma: Is that just because we're slow or we're cheap or we can't afford it?
Simon: Either the vaccine or the monoclonal antibody would be cost effective, and so the recommendation from the Joint Committee of Vaccination Immunisation, around a year ago was that either product could be cost effective, and therefore the government put out a tender to companies, and ultimately it was the maternal vaccine that was taken up.
Emma: And I guess there's some benefits, because, as you suggested, the mothers get some immunity. So that's one thing, and the households and we do have a short acting monoclonal antibody. So, it's not as if we don't have anything. Is it likely to be something that we start using in the future?
Simon: So, for the highest risk babies, we have palivizumab, as you say, it’s the babies who are slightly lower risk, for example, those born moderately prematurely, who may not get maximal benefit from the maternal vaccine, who would benefit most from an alternative option. I think it's likely in the coming years that we will have Nirsevimab or another similar long acti monoclonal available for this cohort of infants. At the moment, Sanofi who make Nirsevimab, obviously, are trying to supply it to many countries across the globe, and so it's somewhat of a sort of supply and demand issue, that they can't supply it to everybody that needs it or wants it. So, the infants at highest risk are those with chronic lung disease of prematurity or bronchopulmonary dysplasia, those with significant congenital cardiac disease, and those with significant immune deficiency, for example, those with severe combined immune deficiency. And then there's also another group of slightly older children, those who are on long term ventilation. All this guidance is provided in The Green Book on Immunization, which you can easily Google.
Emma: Absolutely the green Bible. Use it often. We've talked about who's at highest risk, talking about short and long-acting monoclonal antibodies, but how do they work?
Simon: So, the antibodies work by getting to the mucosal surface in the nose and the lung and preventing the virus from binding to the cells on the respiratory tract. So, if the virus can't bind, it can't, therefore, get into the cells and cause inflammation and disease.
Emma: And the monoclonal antibody we have available at the moment is palivizumab, which is a short acting monoclonal antibody, and you said it lasted for about a month. So, what are the pros and cons of palivizumab?
Simon: So, for many years, the only preventative we've had is palivizumab, and we know that it is effective. It reduces the risk of severe RSV disease in high-risk infants by up to 80% and there's even a little bit of evidence that by preventing RSV disease, it prevents those infants having longer term respiratory problems. So, it certainly is a product that is useful for high-risk infants. But the major downside is it requires an injection every month over the RSV season, and it is extremely expensive.
Emma: Yeah, that doesn't sound ideal. So, there's a new, longer acting monoclonal antibody that's become available. It's another map I can never say them. So, this is?
Simon: Nirsevimab
Emma: So, tell me about the pros and cons of Nirsevimab.
Simon: So, Nirsevimab is a long-acting monoclonal antibody, so it lasts for essentially or provides protection for at least six months. So, the big advantage there, of course, is you give one dose at the start of an RSV season, and that protects the infant for the whole of the RSV season. So, therefore far fewer injections, far fewer trips back to hospital, and therefore also a reduction in the cost because you're giving so fewer doses and fewer healthcare attendances.
Emma: Fantastic, so it sounds good, but it's not yet available in the UK?
Simon: No, so unfortunately, it's not yet available in the UK. It has been available in other countries for the last season, and there's lots of data coming out showing in the sort of real-world setting, it's very effective, significantly reduces hospitalisation due to RSV and even reduces primary care attendances. So, it certainly works. It certainly is very effective, but as it's a new product, the company can only supply so much at the moment, whilst they're in the process of increasing supplies. So, it's not available to every country that would like it yet, including the UK, but we have a maternal vaccine, which provides protection for the vast majority of babies. So, at this point in time, we would only be looking to use Nirsevimab for a relatively small number of babies, anyway.
Emma: So fascinating. I feel like I know almost everything there is to know about RSV and vaccination now. So, will you give me your sort of three top tips, top learning points about RSV vaccination?
Simon: So, I think the main thing is, we've gone from a couple of years ago having one product that was only available for very high-risk infants to now having something that can protect essentially all babies and therefore make significant inroads into that huge burden of disease that I talked about at the beginning. And what we would like to think is that we will, you know, in the coming years, not have our paediatric wards and departments completely full of the children with RSV bronchiolitis. That will have significantly reduced that burden, which is good for the children, of course, and their families. It also means we can potentially prioritise other things from a healthcare perspective.
Emma: Fabulous. I mean, you're completely right. This is a serious disease; children are admitted to hospital for long periods of time. They're admitted to intensive care unit. We have no current effective treatment; it's only supportive care. So really, this is a game changer.
Simon: Yes, it's been a long time coming, but we seem to be heading to the point where we can massively reduce the burden of RSV, and so as you say, we're at probably a threshold where, you know, we can make serious inroads into that burden. And we mustn't also forget that, of course, the biggest burden is in countries that don't have access to the vaccine or the monoclonals at present, so many of the low and middle-income countries. So, whilst it's good for us that we can reduce our burden in the UK and other high-income countries, of course, the biggest areas of mortality are in other countries that at present don't have access, so we must try and improve that in the coming years too.
Emma: Absolutely, I think this global outlook on disease is so vital. Anyway, Simon, it's been a real pleasure to talk to you, I feel a sense of achievement, A, that we have a vaccine, and B, that we've got to the end of this interview.
Simon: Thank you very much. It's been a pleasure.
Emma: We can go crack open the champagne there, and hopefully, with all that time on my hands, because the emergency department will be empty like a ghost town.
Simon: That's the hope.
Emma: The RCPCH had a significant role in ensuring the RSV immunisation programme was introduced in the UK following publication of the JCVI's recommendation to develop one. In March 2024, the College published an open letter signed by over 2000 RCPCH members urging the government to implement a full RSV immunisation programme for both infants and adults across the UK. Our letter generated media coverage and UK parliamentary attention with MPs and Peers supporting our calls, which put pressure on the UK Government to respond. As a result of our campaign, we welcomed announcements from all four UK Governments confirming the rollout of new RSV programmes for infant protection from August 2024 in Scotland, and September for Scotland, Wales and England.
[music starts]
This podcast is produced by Odland education. The views, thoughts and opinions expressed in this podcast relate solely to the speaker and not necessarily to their employer, organisation, the Royal College of Paediatrics and Child Health, or any other groups or individual. You can find a wealth of information on the important work of the Royal College of Paediatrics and Child Health on rcpch.ac.uk, or #choosepaediatrics.
[music ends]
-
EPISODE 11: Get your teeth into this - Paediatric dental health
By the age of 8, one in three children show signs of tooth decay, and this can lead to broader health complications. So, what should paediatricians look out for?
Dr Greig Taylor, a paediatric dentist and clinical lecturer, joins Emma and the team to explore the state of children’s oral health. They delve into the causes of dental decay and preventative measures. And they highlight the particular needs of immunocompromised children and why children with diabetes face a heightened risk of oral infections.
Dr Greig Taylor is a Clinical Lecturer in Paediatric Dentistry at Newcastle University and a Specialist Paediatric Dentist at Newcastle-upon-Tyne Hospitals Trust.
[music, with snippets]
Greig: The main thing for me is, if this child has a dentist, first and foremost. Any sort of infection in their mouth, that they have could be significant in impacting their medical care. Pick it up, lick it to make sure there’s no contaminates on it, and stick it back in the mouth in the right position.
[music ends]
Emma: So welcome. This is very exciting to see today, Greig! And it's lovely for us to have some input from a real life dentist, because I think we’re very bad about thinking about teeth in children. Would you like to introduce yourself?
Greig: Hi, I'm Greig Taylor. I'm currently a clinical lecturer and specialist in paediatric dentistry, working in Newcastle University and Newcastle upon Tyne Hospitals trust.
Emma: That's brilliant. And if we were to get you to think about your top bad things in children's dental health, I'm guessing that caries and infections would be really high up on your list. So, what kind of things do you want to tell us about children and holes in their teeth?
Greig: Yes, so dental caries is one of the most frustrating disease entities, it’s the most common condition that causes children to have to be admitted to hospital for dental extractions. But ultimately, it's a preventable disease. There certainly measures both public health. Right through to chair side level of care, interventions, that can prevent this disease, but it still remains one of the most frustrating things to date. Particularly because the things that cause it are high sugars in their diet, lack of fluoride in terms of not applying them through tooth brushing, or not having engagement with things like community water fluoridation schemes. So yes, it's quite disappointing. I think that in a developed country, we still have children, aged eight, a third have dental decay a visible tooth in their mouth, and the impact that it has on these children is quite significant. Any of you who have had tooth ache before will know the consequence that are suffered by this, but also the impact of not having to attend school, potentially not being able to take part in activities can also be quite difficult for these children.
Emma: Greig, yeah, it's so frustrating because I think it's unbelievable, but the most common reason to have a general anaesthetic is for tooth extraction, out of all children's health problems.
Greig: That’s absolutely correct, Emma. More than double those children undergoing tonsillectomy or ENT procedures. But in addition to that, as it being a preventable disease, it also costs significant amounts of funds to the NHS for hospital admissions. Again, going back to this is a preventable condition.
Emma: Do you know how many bed days that is?
Greig: Off the top of my head? I really don't. But in terms of the number of children, if memory serves me correct, it's pushing 25-26,00 children per annum. It’s a significant number of children across the UK
Emma: That's outrageous. So, when you're thinking about children in the community, how many children have dental decay?
Greig: So, based on our most recent Child Dental Health survey, nationally, about one in three eight years old will have an obvious dental decay, and that figure slightly increases by the time they get to age 12 and 15. So, it's a significant problem that we face and see, and in some children, that might be one tooth, but in others it might be affecting all of their baby or sadly, adult teeth.
Emma: That’s shocking. So, you're saying a third of all children have holes in their teeth?
Greig: By the age of age 8 yeah, around that figure.
Emma: And what sort of impact does that have on kids?
Greig: The most common impact is dental pain, and associated features that may present as not being able to attend school, not eating or drinking properly, having sleep loss during the night, which has impacts on their daily life. But in addition, it also may progress into dental infections and the worst-case scenario, sepsis, requiring hospital admission and multiple antibiotic courses, if not emergency surgery.
Emma: So, if you were sitting in the paediatric emergency department, and a child comes in complaining of pain in their mouth or swelling around their mouth, what would you ask people to look out for? What would you ask paediatricians to look out for?
Greig: The main thing for me is, if this child has a dentist, first and foremost, because the majority of cases, they need to be signposted back to their primary care practitioner to go through the appropriate channels. But if they're not registered, and they have evidence of recurrent pain for several days that pain relief is not relieving, or they are having to have multiple courses of antibiotics, or have visible signs of a swelling or suggestions that they are potentially septic, then these patients obviously require urgent attention, whether that be through paediatric dental colleagues, referral to oral and maxillofacial colleagues, if you don’t have paediatric dental colleagues available or again, working alongside paediatricians who can liaise with the appropriate members of staff at their closest hospital.
Emma: Great. So, what you're saying is that it's a bit more complicated, if children have any signs of being unwell, if they've got fevers, if they've got obvious swellings, pain that's not getting better, had a course of antibiotics and not improving, they’re the ones that need to be assessed and followed through.
Greig: Yeah, you're absolutely right, Emma. These patients need to be signposted appropriately, and that will depend on whether they're effectively septic or not. But it's trying to triage those and make sure that these children don't just fall through the net and don't get care, because it will just continue to be problematic for them. And then if there are recurrent infections that can have an impact on their developing adult tooth or adult dentition as well. So, it's not just a problem for now, particularly young children, it’s a problem for the future as well.
Emma: Yeah, and I think that's one of the things that makes it frustrating, because we said, actually the treatment for this is prevention. So, talk to me about prevention. Give me three top tips for preventing holes in children.
Greig: It's really simple, Emma. The only way a hole develops on a tooth is if there's sugar given to the bacteria that sits in dental plaque. So, if you reduce the sugar intake and the frequency of that, it will certainly not then turn into holes in teeth. So, the biggest thing for me, and the three tips I would always advise is to minimize and reduce any sugar eat snacks or drinks to mealtimes and dinner times. The second tip is to ensure that fluoride toothpaste is used twice daily at least, and most importantly, in the evening and one other time during the day. It is often a misconception that it has to be morning and evenings, and sometimes that does not fit into routines of adults and families, but nighttime is most important to brush because of our dry mouth overnight, and therefore sugars can cause real problems. The third tip for me would be at best to try and attend a dental practice, which currently is particularly challenging, but that sort of recurrent emphasis of prevention and the chair side led prevention that dental professionals can provide is that kind of third area of strength that can really stop and hold this process.
Emma: Right so, let's just have a quick reminder. First of all, getting dentist. And remember dentists are free for children.
Greig: That's correct, yes. So, in the NHS in the current contract, which still provides dental care for all children up to the age of 18 for free. The current issue, though, is trying to access that NHS dentistry. There's a recovery plan within the NHS set up by the new government, which hopefully will start to show some signs of improvement, but certainly, if their children are not registered, then, as every contact should count, it's important to make sure that that message is consistent across healthcare professionals.
Emma: Perfect, and number two, you said brush your teeth twice a day. And that seems really obvious, but actually, we know through some work we've done, that getting toothpaste and toothbrushes is actually quite expensive, and if you're struggling to heat your house and just buying food, it's an extra expensive people can't afford. So there's a new program, which is toothbrushing in schools.
Greig: You are correct. I think for those who are fortunate in society, that can purchase fluoride toothpaste, it's great and the message should be simple for them. But for a lot of children who are currently living in a cost-of-living crisis, these are often the most affected children by dental caries as a disease of inequality. So therefore, it's compounding the fact that not only can they not necessarily eat the healthiest of foods or access oral hygiene products, but they’re also often in those who are in a higher situation where disease will just get even worse for these patients. So, there are certainly some new initiatives that are going through supervised toothbrushing schemes, that have been rolled out in areas within the Northeast already, but are expanding,
Emma: Okay, last of all, which is my absolute thing that drives me insane. In my world, children should only drink milk or water, and the number of children I see in clinic drinking fizzy drinks, sweet drinks and sweet snacks multiple times a day, it drives me absolutely insane.
Greig: You and me both. I think it's particularly frustrating because actually, lots of these products are extortionate in their price compared to what is cheaper in the alternative, milk and water. Sadly, though, I think that a lot of these children are targeted by a lot of these companies for these fizzy drinks, etc, and sometimes it's lack of education. It's easier to get a Diet Coke than it is to put the tap on, which is quite sad, but yeah, I sincerely hope that that is something I would like to change as well, in terms of making sure that milk and water is properly the main thing to drink. It's the safest thing to drink, and it's often the cheapest thing to drink.
Emma: Alright. So, we've talked about dental decay. We've talked about how to prevent dental decay. But there are children who have other medical conditions who really do need to see a specialist paediatric dentist. So, who, are the patients you really like to be referred so that a paediatrician sees them.
Greig: From a specialist’s input, you're absolutely correct, those patients that are likely to become immunocompromised because of impending treatment, transplant treatment, or those are a high risk of infective endocarditis. So, your immunology, oncology, renal, cardiac patients, all are absolutely key to ensure they have a specialist level input in their treatment planning, because any source of infection in their mouth that they have could be significant in impacting their medical care, and in some cases, be even more fatal. So, it's important that they are screened appropriately and checked by a specialist in paediatric dentistry.
Emma: So alright, so let's break that down. That's really important. You know that I see children who are about to have bone marrow transplants, we always get their teeth and gums checked. Because, as you say, in any child who is immunocompromised, so those who are having chemotherapy, those on certain drugs, primary immunodeficiency, they are more likely to get serious infections. And certainly, if they're if their immune is suppressed due to treatment they may get sepsis. And as you say, infection can be life threatening. We're also talking about children with cardiac problems and children with chronic renal disease, but one of the really big groups of children are children with diabetes. Do you have any special tips for children with diabetes?
Greig: It's often a difficult one because of the comorbidities that unpoorly controlled diabetics are often due to uncontrolled sugars, particularly, or having to deal with hypo-attacks, with things that aren't always great from a dental point of view, and there has to be a pragmatic sort of risk/benefit analysis for these patients, but I think it can become really demonstrable. And we see these patients in clinics who have widespread, not only dental disease, but periodontal infections. So, gum disease, there's a huge link between type one and type two diabetes and gum disease, or gum infections. So, the prevention is just as imperative for these patients as those who are acutely immunocompromised.
Emma: That's really interesting, I hadn’t thought about that. So, children with diabetes, they might be having hypoglycaemias and having to have multiple very, very sugary drinks. And of course, children with diabetes are at greater risk of infection. So, is there a quick thing, should they just brush their teeth after having sugary drink if they need them?
Greig: You may think that be the correct thing, but actually that makes it worse, because if you brush your teeth straight after having something sugary, your mouth is an even more vulnerable state. So actually, to balance the pH levels of the acidic nature that sugary foods cause, it's probably better to have something more neutralizing, like a glass of milk, a small piece of cheese, bit of bread, that will actually bring the pH level back up. If you brush straight away, the teeth are in a vulnerable state so you’ll actually you'll be brushing off more enamel, yes in small, microscopic amounts, but over enough time, it will continue to do that damage. So certainly, I'd be not advising patients to do that, to not brush straight away after having some sugary hits.
Emma: Interesting. So, after your sugary you have to eat cheese, bread or milk, neutralize the pH in your mouth, and then brush your teeth. So, is gum good?
Greig: Sugar free gum? Yes, Xylitol yes. But the gums that are, as I remember as a child, the Hubba Bubba, which is purely just sugar and has no effect other than just damaging your teeth, is not ideal. So yes, I would certainly say I would encourage children to have sugar feed gum at age appropriate. We're talking sort of 10 and above, if that makes sense, is when I would feel more comfortable to kind of encourage that.
Emma: Interesting. Okay, so we've talked about immunocompromised children. We've talked about children with diabetes. What about children with things like cerebral palsy and learning difficulties and autism? Because I think they're a really huge at-risk group.
Greig: Yeah, you're absolutely right. I think children with special education needs, but also learning difficulties, are particularly challenging. Their routine care often is not carried out in primary dental services. They tend to see within the community dental services, which is often most appropriate place for these children. I think in particular, those children who can’t advocate for themselves, or can’t advocate or provide their own oral hygiene and rely entirely on others. That's what it's really working with the parents to kind of make sure that you can get that tooth brushing instruction on board. It can be more challenging in some of these children, and that's where a specialist in paediatric dentistry can really come in to provide some more practical tips that are patient specific and tailored to that individual. Because not everything fits for those children, there has to be some sort of nuances that would be particularly pertinent for that individual family, and that's where the skill of that specialist comes in.
Emma: In a child who, for example, is non-verbal and doesn't want to open their mouth. What's the easiest way to brush their teeth?
Greig: The easiest way is really perseverance. And what I mean is that if you persevere long enough, and you try in a systematic fashion, in most cases, children generally will allow any toothbrush in there, and it might be built up over time with the dry toothbrush, the small toothbrush, the children’s toothbrush. There are also toothpastes which are non-foaming, so they're SLS free, they also have no flavour to them. And often we find with those children who have sensory issues, particularly of the autistic group, that is sometimes the biggest problem. Toothpastes are too spicy or they foam in their mouths. So, currently there's only one available toothpaste called Oranurse, which is on the market, which we recommend to all of our autistic patients, and indeed, those children who have additional learning needs, because it tends to just be accepted much more readily by these patients.
Emma: Okay, so that's really interesting. So, if you have a child with learning disabilities or autism spectrum disorder, when you think about breaking toothbrushes down to small steps, getting them used to a toothbrush, getting them used to a dry toothbrush, and using toothpaste that don’t have strong tastes and don’t foam, and the one you recommend is Oranurse.
Greig: That’s correct.
Emma: Perfect, that’s really interesting. There's one more thing that we get presented with that I never know what do, when children come in, because they knocked out their teeth, so they're holding the tooth. What do you do? And I'm going to break that down into milk teeth and adult teeth.
Greig: So, I will break my answer down into those. If it's a baby tooth, and we're talking in children under the age of six and a half years. If the baby tooth has come out, then you in theory don't need to put it back in. You shouldn't put it back in. It's not advisable to do so. However, it might be worthwhile checking with a specialist in paediatric dentistry potentially or even Maxfax to confirm that it is a primary tooth.
Emma: Yeah, that's so funny. I've got a really funny story, one of my friends is an orthopaedic surgeon, and his daughter was about, I don't know, she was perhaps seven. And his wife came running in, going, ‘Oh, she's knocked her tooth’, and they rushed to the emergency department with the tooth all wrapped up. Sat there for hours and hours. He was googling on his phone, and then he just went, you know, that tooth is supposed to fall out at this, and they’d just wasted their whole evening. So I think that’s really good advice. Under six, you said still don't worry. You can get it checked.
Greig: Yeah, I think if it's a, if it's a baby tooth and it falls out, do not worry. Indeed, give it to us. We know the tooth fairies.
Emma: Alright, so adult teeth, let’s talk about permanent teeth. If it falls out, what do you do?
Greig: If it falls out, the best thing to do is to put it back in as quick as possible. All of the evidence would suggest that long term success and outcomes are improved the quicker you get it back in. And it's really as simple as push it back in. We would encourage schoolteachers, educators to do that, as long as it's generally clean so there's no dirt on it, rinsed under with some sort of saline in a clinical situation, and push it back in and wait for a dentist or MaxFax to come and help hold it and splint it in that position. So, the kind of advice that we would often say is, pick it, lick it, stick it. That's kind of the simple public health measure. Pick it up, lick it to make sure that there's no growth contaminants on it, and stick it back in the mouth in the right position.
Emma: I love that. Pick it, lick it, stick it.
One last question, what happens if they knock the tooth out and it hasn't got the root or it's damaged? What to do there? It's like a hockey match. Somebody smashed you in the face.
Greig: So yes, again, it's all dependent on age development, how much the roots developed, but the guidance would still say that any adult tooth has been knocked out, stick it back in, because if it hasn't really formed, there's always a chance it will regenerate and continue to grow. Even if it's been out the mouth, a completely developed tooth, and it's been a long time, it's much better to be in there and holding the bone and holding that to make life a lot easier when they're older. So, I would always encourage any adult tooth that has been knocked out to be put back in. The only thing Emma that might be worth just considering though with the evulsion, replantation, is if the child is immunocompromised. So, if they are undergoing chemotherapy, oncology, then that would be the only situation I wouldn't put it back in.
Emma: Alright, so your one proviso is if they're immunocompromised, you don't necessarily stick the tooth straight in, you ring Greig first.
Greig: Ring one of us for advice and discussion.
Emma: Let’s have your three top tips for healthy teeth and children.
Greig: Tip number one, minimise sugary intakes and encourage that with all of your patients. Number two, get them to brush their teeth. Simple win, as we've already talked about. And three, encourage them to go to a dentist or engage in supervised toothbrushing programs and public health measures, if they're not access to the dentist. It's the majority of children who have dental disease, it is preventable, and it will make life a lot easier for them, for the NHS and the wider society, if we could get a hold of this problem, and start to reduce its impact.
Emma: Amazing. And three top tips for paediatricians referring patients. Who do you want to see?
Greig: We want to see patients who are likely to become immunocompromised or are already immunocompromised. They're massively important for us to reduce the risk of a dental disease infection. We also want to see patients of whom you're having difficulties with, if they're of special education or learning needs. We're more than happy to see those patients, and often the time for families would really welcome that input. Thirdly, the patients groups that we love to see are those who are maybe routine children going for general anaesthetic procedures, or in patients who are going for general anaesthetic procedures, who will also potentially have dental problems, and trying to minimize those by doing piggyback type procedures, is something that can be of real importance to the hospital, for waiting lists, but also to the patients. And having to not go through the trauma of multiple general anaesthetics and trying to do several things at once can be of much more benefit.
Emma: That’s really good tips. So, like, if you have a child who's going for a central line, think about whether they need a tooth check-up under their general anaesthetic.
Greig: Particularly those patients who maybe have got additional learning needs and we can't do a full examination, sometimes just being able to have a look in their mouth when they're under anaesthetic, not necessarily do treatment, but that examination can provide reassurance to the family that there are no problems, or there are no problems. Or actually it can provide reassurance there is some dental issues. We need to address it, and let's plan it, and make a plan appropriately to do so.
Emma: Amazing. Well, it’s been really fun talking to you. And I was going to say, you know how people say I'm really proud of running a marathon, or I'm really proud of raising loads of money. I'm really proud that I have got two of my children to 18 with no holes in their teeth. I consider that to be one of my greatest life achievements.
Greig: I commend you on that, Emma.
[music starts]
This podcast is produced by Odland Education. The views, thoughts and opinions expressed in this podcast relate solely to the speaker and not necessarily to their employer, organisation, the Royal College of Paediatrics and Child Health, or any other groups or individual. You can find a wealth of information on the important work of the Royal College of Paediatrics and Child Health on rcpch.ac.uk, or #choosepaediatrics.
[music ends]
-
EPISODE 12: Vax machines – preventing infectious disease
This time around we have a very special guest, the former Chair of the Joint Committee on Vaccination and Immunology, Professor Sir Andrew Pollard. He joins Emma and Christo to highlight the importance of prevention of infectious diseases and how this could change the future of child health and the NHS itself. The panel discusses population health in general, children with immunodeficiencies, vaccine uptake and vaccine hesitancy amongst much else.
Professor Sir Andrew Pollard is Professor of Infection and Immunity at the University of Oxford, Director of the Oxford Vaccine Group and was Chair of the Joint Committee on Vaccination and Immunisation (JCVI) for 12 years until June 2025.
[Music starts]
Andrew: Prevention is really where we should be spending more of our efforts in the years ahead to change not just child health, but the future of health for the NHS.
Emma: Children who are at higher risk, so children with immunodeficiencies, or parents of premature babies, actually could be the champions of vaccines, because it's so much more important for their children that everybody around them is vaccinated.
[music ends]
Emma: Hello, and welcome. So, I'm very excited to introduce our most eminent guest we've had on our podcast so far, Professor Sir Andrew Pollard, who is a paediatrician in infectious disease and immunology, and director of the Oxford Vaccine Group, and head of the Joint Committee on Vaccination and Immunisation (JCVI). So, good morning!
Andrew: Good morning. Thank you very much for having me on the podcast. I'm not sure about the eminence, but very kind of you to introduce me that way.
Emma: And as usual, I have Christo, who is our PhD student and trainee in immunology and infectious disease to keep me on the straight and narrow. Good morning. Christo!
Christo: Morning, Emma.
Emma: So, we had a whole list of questions and things we wanted to ask you, but the thing that struck me first, Professor, Sir Andrew Pollard, was tell me, how did you become so passionate about vaccination and immunisation? Because this has really been a life's work for you.
Andrew: Well, thanks very much for that. You can just call me Andy if you like, rather than have the lengthy title. I guess really the starting point is as a paediatrician, and we all see many children with infectious diseases. And as a medical student, I spent some time in West Africa on my elective, and you realise that the real burden of serious infectious disease is in the first few years of life, and particularly in the most resource poor parts of the world. And so really, my passion was about thinking how I could work in those settings as a paediatrician.
I did some research in West Africa on infectious diseases as a student and did an undergraduate degree in Immunology at Guy’s Hospital, and that really was such an exciting time. The T cell receptor (TCR) had only just been discovered, and so immunology felt like it was going through a rebirth, having written largely about understanding antibodies before then.
And so, moving into clinical practice as a junior doctor, I was really thinking about how to build on that interest in the immune system. And so, my focus was really on, how can you understand immunity, particularly in early childhood, where people haven't really been doing any studies because it's so difficult to do that on small volumes of blood, and the techniques available weren't very good at that time for working with small volumes. And I thought we had something unique to do to try and explore immune responses to diseases and infectious diseases in young children, and it struck me that actually, vaccines were quite a good tool to be able to stimulate the immune system and then try and understand the development of immune responses from birth through the first few years of life.
So that's really when I came to Oxford, nearly a quarter of a century ago, that I was really thinking about. It was all about the immune system and an intellectual curiosity about the development of immunity. And I guess it pretty rapidly dawned on me that vaccines actually are pretty good as well of stopping the diseases, that I've been looking after children who had them in the hospital. And so I really have, over most of the last 25 years, been much more focused on using that knowledge of the immune system to improve immunisation, improve child health by preventing disease, which has been incredibly exciting.
Emma: There's one word in that that really stands out to me, because I think we're so bad at preventing disease, we're so reactionary, we never think about what we can do before. So that focus on prevention is so important.
Andrew: I agree completely. Last year, I launched the Academy of Health Sciences Report on Child Health, which is really about the future of population health, and really, they're showing that what happens to the child in the first five years of life. And that is true of exposure to infectious diseases. It's true of the built environment, of pollution, all of those factors are really setting up the child's health for the future, whether or not they're going to be an adult who's obese with diabetes or with lung disease from a smoky environment or environmental pollution. The economic deprivation in early childhood that affects so much of life chances and changing that environment. A lot of which is not about health solutions but changing that environment in the first five years of life, has been shown through childhood to reduce the number of hospitalisations and improve exam results at the end of school. And some wonderful experiments in America showing reductions, also even in crime in inner cities, by nurturing better in the first five years.
It's just that prevention is really where we should be spending more of our efforts in the years ahead to change not just child health, but the future of health for the NHS,
Emma: Oh dear. My only problem is that you seem to have given us enough topics to go through at least two more podcasts. But yes, I agree.
Andy, what do you think are the big issues in paediatric vaccination and the schedule in the UK today?
Andrew: Well, I think just taking, first of all, a helicopter view about the future. I think one of the problems that we have, both in the UK, and in fact, globally, is technologies advancing very rapidly, which means that we can do more, but we've actually now got very few opportunities to, and indeed limbs, to stick more needles in. And I think that it's much more of a problem in the developing world, where there are still major infectious diseases that we don't have here, where new vaccines have to be introduced if we're going to have a big event. Let's take malaria, for example. That's extra visits for the child in some of the most resource limited settings, and a needle burner, but there are other vaccines that need to be added as well into those programs because they have such a threat of infections, and so that actually just adding more to the schedule without working out how to make new combinations is a real challenge for the future.
Emma: So that's really interesting. So, in fact, what you're talking about is how to be more efficient and effective and get more vaccines in but continue to have the same number of visits and as few actual physical jabs as you can.
Andrew: Absolutely, I think that is really what I'm sure the infant wants, but it's very much what parents want, and the vaccinators would like not to have to stick so many doses. We are in the UK in the next 12 months about to have a major change to the immunisation schedule for early childhood, as a result of one of the vaccines that we have had in our program, the Hib/MenC vaccine, which was given at 12 months of age that is no longer being produced by the vaccine company. And so we've had to rejig the program as a result of that, and there'll be lots of communications in the next 12 months about that, and we'll be changing the schedule. I think we'll almost certainly have better coverage as a result, and without any loss of protection in the population.
Emma: I’ve seen a lot more bacterial infections this year, more empyemas, serious, invasive bacterial infections, and that's come on the back of these huge flu pandemics, COVID pandemics. So, it just underlines the importance of what we're already doing, and doing that well, without any gaps.
Andrew: I think that's absolutely right, so that when you look at the problem with vaccination rates, that we see, and certainly the narrative that's in the media and from politicians is largely that this is the anti-vaccine problem. But the reality is that it is much more about access, and that this has been studied over the last 25 years, and we know very clearly that the main way that you can change vaccination rates is making it easier for parents to access immunisation services.
And I think that's harder than it used to be and it doesn't help if people are a little bit hesitant. Which of course is a rational behaviour. Now, if someone's coming your baby with a needle, it's rational to ask questions, but if you can't access the trusted health professional to ask those questions, then the vaccination may well not happen. So, there's the whole system around immunisation needs to have improved access.
Some of that is probably just making more appointments available. Some of it is around understanding the particular needs of individual communities. I mean, just as one example, there's one community that we're aware of in London who weren't coming forward for vaccination because they believed you had to pay for them. They couldn't afford it. Perhaps another example is if you know large family size, some communities have very large family size, and in those groups, then trying to get to the vaccine clinic with five children when the new baby comes is extremely difficult. I certainly couldn’t manage five children and a new baby on a bus.
Emma: Yes, I absolutely agree. I think that vaccine access and vaccine availability is a huge issue. And I think that the recent flu vaccine and the roll out in school where there weren't necessarily enough doses, and they didn't have chance to do a second round, is an example.
I think it's really important in the current cost of living climate crisis, to think about how difficult it is to get to places. So, when money is short, if you can't afford to feed your family, then that extra bus fare, the extra time it takes, becomes much more challenging.
Christo: You touched upon issues with production of vaccines, particularly with Hib/MenC, and I wondered was there anything that we learnt from the mass rollout of things like COVID vaccination in 2021 that could be used to try and circumvent some of these issues? Or do you think that this is going to be something that recurs where certain vaccines become harder to get, and so we are constantly having to shift the schedule to try and make sure there's adequate coverage?
Andrew: Well, I hope that won't be the case. I think market forces really determine which of the licensed vaccines remain available, and so for many of the newer vaccines, countries do pay quite a lot for them, so the market forces are likely to keep them available.
I think one of the problems with the older vaccines, the ones really which have been around for most of the last 60 years, since we have vaccination programs, are ones that we hardly pay anything for, and so there's much less incentive for some vaccines, for companies to keep producing them. And something like the Hib/MenC vaccine, we were one of the few countries that still had it in our program, and so we're a large market, but not as large as you need in order to sustain a whole manufacturing facility. At least, that's my guess as to why that happened.
Emma: Andy, I'm just going to take you back to something. You talked about vaccine hesitancy, and you said that part of the problem is that families just need the opportunity and the time to ask their questions, and it's a natural thing. What tips would you give paediatricians who are faced with parents who have worries, concerns, doubts about vaccines?
Andrew: Well, I think it's very important that the paediatricians are knowledgeable about vaccines and how they develop their safety record, because many of the questions are actually very easily dealt with just by some knowledge. And I mean, it's quite interesting. I'm sure, if you were to look in the clerking that your junior team do, they very often don't even ask about vaccines in their clerking and they may well even, if they've documented unvaccinated, have no plan in place for a discussion with the family or even perhaps to offer the doses in hospital. Given how important these vaccines are, they're lifesaving, we really should have it much more in the forefront of our minds to be engaged in that conversation.
And I think one of the things you find is if you have the conversations frequently with parents, you start to know what their concerns are, and you do have the answers, because that helps you make sure that you maintain your knowledge and you look up the information so that you're ready for the sorts of questions that do come up.
I think there's a there's a fundamental issue here, which goes back to other types of major public health interventions, and I think of two of the major ones in my lifetime, seat belts in cars and then the smoking ban, both of which had huge pressure against them when they came in. But for both of those now, if, if you're in a restaurant and someone lights a cigarette next to you, you're not going to be very happy about that, and they would almost certainly be told by everyone around them to stop. Similarly, if someone gets into your car and they don’t put a seat belt on, you won't drive off. And in fact, even if you said nothing, the car would start beeping at you. And we're not in a situation where our society says, ‘Actually, I'm not very about you not being vaccinated’, and we're quite comfortable with the idea that it's acceptable for people to be unvaccinated. If you reach a point where the majority of the population actually feel this is critical for the protection of their own child, but also to other people's children, that we have high immunisation, if there's such confidence in that, that we'd have a very different relationship with vaccination.
Emma: So, yeah, I think that's really true. Paediatricians need to be knowledgeable. They need to know about safety data. They need to listen to parents and have time to make these conversations. And I think that point you made, which is really interesting, that children who are at higher risk, so children with immunodeficiencies, or parents of premature babies, actually could be the champions of vaccines, because it's so much more important to their children that everybody around them is vaccinated.
Andrew: Absolutely, I fully agree. And you know, I can think of many cases over the years where a child has been severely ill or ended up dying or even with neurological damage as a result of infection that was vaccine preventable, and for those parents, this is the most awful scenario to be in where they've decided not to vaccinate, and then their child has had very significant injury or illness as a result.
Christo: You've mentioned some strategies for trying to deal with kind of concerns or hesitancy at an individual level, and I just wondered, with your JCVI hat on what sort of things, what strategies work for trying to improve vaccine literacy for the global population?
Andrew: A very good question. I was not actually part of JCVI’s remit to deal with that, much more on the science of vaccines and looking at the burden disease, which ones should be used. But this, this whole area of what we need to do as a society to change literacy, I think there's some quite interesting research from psychologists that if as a parent you turn up in the clinic for immunisation, and you haven't decided already that it's the right thing to do, when the practice nurse comes at your baby with a needle, the point then is usually the wrong decision is made. So, we need to be in a situation where people, by the time they're having children, already are confident about the importance of immunisation, and to my mind, you only do that by starting much earlier on in life, and probably as part of the curriculum in schools, and that isn't there. It's very difficult to change someone's mind, and as an adult, we all get very fixed views on what our belief systems are. So really, if we're going to change the way society thinks, we have to start much earlier.
There's also understanding at the grassroots in some communities what their particular concerns are. Some of that is a social media side of things. Some of it is informal networks that people have in their particular religious or ethnic communities where you really need to have champions there to provide safer communication.
Emma: You've talked about what the current schedule is like, you've talked about access and availability, and we've touched on hesitancy and how to deal with that. What's new? What's round the corner for vaccines?
Andrew: Well, I think for the UK, we've just heard one really important corner, which is the start of RSV vaccination, which is both maternal vaccine and also for the elderly. And I'm really excited over the next few months, we're going to see the first data on how well those programs have performed. I think we'll have the best data set from the elderly, because it was a large program which was rolled out before the season. Maternal vaccination, it may be that we have some preliminary data, but it's next year where we'll have the best data, where there'll be many more mothers who are vaccinated before their babies are born, which is obviously critical for the success of the program.
So, I think this is a really exciting turning point for all paediatricians. We just know how the wards are filled up with babies with bronchiolitis every winter. The total number in the UK is about 25 to 30,000 babies admitted over mostly a six-week period, which is why we're bulging at the edges during that period in the late autumn. And if that can be overcome in the way that the vaccines have promised to, paediatrics has transformed.
Emma: Yeah, absolutely, good point. Fortunately, we have Simon Drysdale with a whole podcast on nothing but RSV vaccination.
Andrew: And so just to add to that about what's coming next. There are some, I think, some really exciting potential developments. The leading cause of neonatal meningitis is Group B streptococcus, which paediatricians will be very familiar with. There is now a vaccine which covers Group B streptococci, which is in development. And really now the data is coming in for that. It's largely a regulatory decision about what amount of data gives them confidence the vaccine will be protective. We know it's safe, but it's just the extent to which it will be protective. And that could come within the next year or two, and then maybe JCVI will advise that that's used in the future.
And if you look across infectious diseases that have a lot of severe illness, deaths, admissions to hospital, then once you've got RSV under control, and you've got Group B streptococcus under control, there's actually not very many that either have that severe disease in reasonable numbers, or huge numbers of cases, like RSV, that is left. And you get into the point where you're starting to think, well, maybe we could tweak, say, an RSV vaccine, a little bit to add Human metapneumovirus (HMPV) or parainfluenza 3.
Those on their own almost certainly couldn’t be introduced, because they wouldn't be cost effective for the NHS, but if you add them to existing products, for the companies that make them more competitive, but it would actually add a little bit more protection to our childhood programs. So, I think that's the sort of direction of travel I would like to see, is that we can do better than we are at the moment, but RSV and group B strep have really been, for me, the top of the list of the ones I've for the last 10 years wanted to see happen. And I feel like we're on the cusp for Group B strep, and we are already there for RSV.
Emma: I love that idea of piggybacking vaccines on another so RSV and including new things like Human metapneumovirus, which we know is causing a huge problem in Australia for their current season.
Group B strep, so that's really exciting. And I think Christo, you're currently working in a neonatal unit, so maybe you want to just touch on the huge amount of work that group B strep causes to all these born, just born babies.
Christo: Thanks, Emma, because I think we see Group B strep a lot and worry about it a lot as paediatricians, but really, it's the obstetrics team and midwives that have a huge role in trying to pick up mothers at risk and which family should be offered intrapartum prophylaxis and so on. In terms of where the group B strep vaccine might fit, is this envisaged to be a maternal vaccine in the same way that RSV is, or is it a vaccine given to a to an infant?
Andrew: So the vaccine that's being developed is a maternal vaccine that would not only, I think, I hope, protect the infant from early onset Group B strep, but also late onset disease, and perhaps also mean that we can rethink all of those antibiotics that are being given in late pregnancy and on the postnatal wards to babies at risk. So I think it's hugely impactful and important vaccine to have in our program.
Emma: Yeah, I think that's such a big thing. I think we need to be thinking about our use of antibiotics, and in this instance, when we worry about Group B strep, sepsis and infections and little babies, we use a huge amount of antibiotics prophylactically, so the children aren't even unwell, and we're giving them 48 hours of antibiotics just on the off chance. So, this is an enormous opportunity to save and to improve our antimicrobial stewardship.
Andrew: Antibiotic resistance is a major problem in our hospitals, and I'm sure you're facing that in your centre, just as we are here in Oxford. And one of the great things about vaccines is that they can be directed against resistant bacteria, and we have pneumococcal vaccines, which reduce the resistant pneumococcal bacteria that cause infections.
But perhaps even more importantly, the vaccines against viruses like RSV and influenza reduce the number of inappropriate antibiotic prescriptions, because it's obviously very hard in the community to decide whether you're dealing with the virus or bacterial infection, and so many prescriptions happen that probably weren't needed. So, if you can reduce the viral infections, that may have at least as big, if not a bigger, impact on antimicrobial resistance and certainly antibiotic use.
Emma: So, we can add antimicrobial champion to the rest of your titles as well.
Andrew: It would be nice if you did add that to my title. But I think the most important thing here is that we don't capture very good data on the way that vaccines can prevent antibiotic use. The reason why that's important, obviously there's an importance for the message, but when we're calculating whether we can afford to pay for for vaccines now using treasury rules, one of the key things is cost effectiveness. And if you can reduce antibiotic usage and antimicrobial resistance and its costs, then that makes vaccines even more attractive to use.
Emma: So, you were saying, if we treat RSV and group B strep, there won't be many illnesses left. But one of the common illnesses I see a lot of and the effects afterwards is chickenpox or varicella, and so for many years, we've been thinking about a varicella vaccine, and we know that actually, Australia, America, other countries have it. So what's happening there?
Andrew: Well, that's a really good question, and it's been something at the forefront of my mind over the last 12 years of chair of JCVI, because as a paediatrician, in fact, for all the paediatricians on the panel, exactly as you say, the burden of complications of varicella is enormous. Apart from, obviously it’s an unpleasant childhood illness, but also the complications we all see, particularly associated with group A strep, secondary bacterial infection.
And the thing that really held things up was a view, which was based on some evidence, that if you vaccinate against chickenpox, that there will be less natural boosting of adults, so that over the course of the next 80 years or so, we'd have a big increase in Zoster in the elderly. And you might say, well, we're paediatricians, why should we care about that? And the reason is that the NHS would care, because a lot of money is spent on treating post herpetic neuralgia in the elderly, a huge amount. And so, if vaccinating children did push up Zoster rates, then actually the cost effectiveness, becomes a problem, it's no longer cost effective, it wouldn't make sense for taxpayers to pay for that.
So, there's been, over the last 12 years, discussions, review of data, and finally, the latest updates from the US, where they have 25 years of data, to show that with all of that time, you don't see an increase in Zoster in the elderly. And so, I think we're now confident that introducing a chickenpox vaccine will protect children, will reduce the complications, and we don't think we'll have any significant effect on Zoster in older adults, and therefore cost to the NHS. And so part of the changes to the vaccine schedule, which are going to come in the next 12 months or so, will include the addition of varicella vaccine, and I think for all of us have been at the front end, particularly as an infectious disease paediatrician, of seeing these cases, I'm really delighted that we've managed to get that finally over the line.
Emma: Yeah, absolutely cause for celebration. We've been waiting a long time. So that's really interesting to hear that the Joint Committee of Vaccination and Immunisation, so the JCVI, has finally got the data from 25 years of the experience in the United States of using varicella, that there is no increase in herpetic neuralgia in elderly population. And therefore, it is not only effective, but financially effective and efficient, and that it will become part of our new vaccination schedule. As we touched, on the severe bacterial infections, cellulitis, meningitis, group A strep, that all occur after chickenpox are a huge burden to not only families, but the health system. Perfect, I think that covers that.
Andrew: Absolutely. I should just make one comment, which is that we have in all Western countries seen an increase in Zoster in the elderly over many decades now. So, there is an increase. But what is clear is vaccinating children is not accelerating that increase. The causes of it are, to some extent, unknown.
Emma: Maybe we should start boosting adults then.
Andrew: Well, we are doing because that's what the Zoster Vaccine Program is that, now happens for older adults. So, we have a since 2013, there's been a Zoster program, and it's been switched to a new vaccine called Shingrix ® in the last couple of years, which is very exciting.
Emma: And then finally, going back to something that you talked about, I think your initial point when we talked about vaccine hesitancy, is that when parents see a nurse coming towards their child and their baby with a needle, they instinctively, sort of recoil. They don't want their child hurt. So, is there any work on new delivery systems or delivering vaccines without needles?
Andrew: Well, there's been quite a lot of work over very many years, and there are various systems, including patches and so on. I think one of the difficulties there is, none of those new technologies has really got into the mainstream so far. I mean, there are some which are being used for medicines, but in vaccination, they've not got over the line at this point. Part of that is just that we have a very successful vaccine program, and if you're a producer of those vaccines, to go to a different delivery system, actually means relicensing, and it's quite a big opportunity cost for the pharmaceutical companies, so they're not so keen to make those changes.
But I do find it slightly puzzling that no one has innovated with new vaccines to add those into these very, very crowded schedules. So, I think there's still work to do, but there's lots of people working in this space, so maybe in the future, we will just have tp slap the patch on and that will be the answer.
I think the second thing to say on this is that there's some really exciting developments about delayed release. So maybe with one needle, you might be able to start the immune response. Then, rather than giving a booster, there's a delayed release of the materials, so that you get a booster that happens from the original injection, but is delayed by a few months, or six months, or something like that. So those sorts of innovations, I think, are going to be game changing to help us with the crowded schedule and perhaps increase acceptability of vaccination.
Christo: That's really interesting. And I just wondered, we know that the nasal route is effective for certainly influenza vaccination. And I wondered, is there any work looking at mucosal immunity and whether any other pathogens could be targeted by what seems like a much more tolerable way of administering vaccine?
Andrew: Yeah. I mean, I think the nasal route for flu vaccines has been terrific for the childhood program. It's not as scary as a needle, and you can do large numbers very quickly, so it's an extremely efficient way of approaching that.
For something like RSV, there's been quite a bit of work on giving intranasal vaccine, live-attenuated vaccines, over quite some decades now. And I think the problem there has been either that they were so attenuated that they didn't protect, so very safe but didn't provide protection, or they were protective but not attenuated enough so that they actually caused some fever and snuffly noses. And so, I think that it's not straightforward, just saying ‘Let's just make a vaccine and give it by that route’.
The second thing I would say is that we really have a poor understanding still of the mucosal immune system, and even with the flu story, where we know that from a delivery point of view, that live-attenuated vaccine is great, there isn't particularly good evidence that it's better than the needle. I mean, it obviously is from a delivery point of view in terms of protection, there are great studies showing that vaccinating large cohorts of children in counties in the US, or in a Japanese experiment from the 1960s, that the needle works just as well in reducing flu in children, but also, importantly, the transmission to older adults.
Emma: So, thank you, Andy, and I think in all cases, we like to think about global health of children, not just the children in the UK. So, what kind of vaccine advances are available globally? Because sometimes it's money and availability that holds things back. So, what have you got to tell us about the global situation?
Andrew: Well, there is definitely a lot of work going on globally, the World Health Organisation (WHO) has been tracking developments of new vaccines that could be rolled out to try and improve health in low-income settings. And I've been working in South Asia for the last 20 years, both in the epidemiology of infectious diseases in early childhood, and also on trying to promote vaccines and testing the vaccines in those settings and supporting governments introducing them.
Perhaps for me, over the last 10 years or so, the most exciting has been around typhoid. Where we, first of all, showed that a typhoid vaccine was protective using a human challenge model. This is where, in Oxford, we deliberately infected people with typhoid by getting them to drink Salmonella Typhi as if they were drinking contaminated water in South Asia. And were able to show that those were vaccinated had good protection and that then supported the WHO decision to start rolling out the vaccine, and over the last three years, 60 million doses have been given to children in South Asia and in Africa.
And in the meantime, we've been doing studies to look at the effect in children in the real world, vaccinating 100,000 children since 2017 and then monitoring those using randomised trials as some had control vaccine, and we're able to show that 80% of typhoid was prevented in that huge clinical trial.
So, you know, I think that's been a real major part of what I've been doing over quite a few years now, and really exciting to see something we've worked on now being rolled out, and this next year, Bangladesh will roll out, and so the numbers of children protected against this disease will be absolutely enormous. Incredibly important, because this illness disrupts education, causes febrile illnesses in many people and a proportion are hospitalised, with millions of cases every year, and at least 100,000 children are succumbing to infection.
Emma: Yeah, that's really exciting news to know that there's a vaccine for typhoid, such a huge burden of disease in the global population. That obviously leads me to ask you, what happened to malaria and the malaria vaccine?
Andrew: Well, there are now two malaria vaccines that are produced that are being rolled out in Africa. One is from GSK, and one was developed by Oxford and is now manufactured by Serum Institute of India. And both of those vaccines are being deployed, and we hope over the next few years to see big reductions in the malaria burden. Obviously added to by the use of bed nets and the various insecticides that reduce the risk of transmission, plus intermittent treatment. There's lots of tools now that can start to improve protection in populations, and new generation malaria vaccines have been worked on as well, so we might have an even better protection in the future.
Emma: So, I think from what you say, the future looks bright. We've talked about new vaccines in the UK. We've talked about the RSV vaccine, group B strep vaccine that may be coming. We've talked about how the schedule is going to be rejigged and possibly a reduction in the number of visits and the number of needles that each child gets. And globally, looking at typhoid and malaria. So, it's an incredible body of work, and it's been fascinating talking to you today. So, thank you very much, Andy.
We always ask anybody who comes on our podcast, they can have three top tips. It's like desert island, three top tips you'd like to pass on. So, what are your three top tips?
Andrew: Well, I think my top tips are, get vaccinated. There's only one, yeah, get vaccinated and make sure that all of your patients are vaccinated as well
Emma: Absolutely fantastic. It's been a pleasure.
Andrew: Thank you very much for having me on the podcast.
[music starts]
This podcast is produced by Odland Education. The views, thoughts and opinions expressed in this podcast relate solely to the speaker and not necessarily to their employer, organisation, the Royal College of Paediatrics and Child Health, or any other groups or individual. You can find a wealth of information on the important work of the Royal College of Paediatrics and Child Health on rcpch.ac.uk, or #choosepaediatrics.
[music ends]
-
EPISODE 13: Drilling down into teeth
Children's oral health is in a crisis: it's the most common reason for children to visit a hospital and it’s not improving as quickly as we need.
Professor Peter Day, paediatric dentist and professor of children’s oral health, speaks with us around the stark facts on tooth decay – it affects 10% of three-year-olds and 48% of 15-year-olds – with impact on a child’s ability to sleep, eat, talk and go to school, and on the health service – and how community interventions can help. Plus, how supervised tooth brushing can provide economic as well as health benefits.
Professor Peter Day is a Paediatric Dentist (in Leeds and Bradford) and Professor of Children's Oral Health at the University of Leeds with interests and expertise in children's oral health research and dental trauma. He speaks with the podcast host and paediatrician, Dr Emma Lim.
[Music starts]
Peter: Children's oral health is in a crisis, and it's unfortunately not improving as much or as quickly as we would like.
So, the most common for children to come into hospital is for dental reasons, over twice as common as for ENT procedures.Emma: You learn to ride a bike, you learn to eat healthy. Why should you not learn how to brush your teeth?
[music ends]
Emma: Welcome. It's really exciting to see you and talk to you today, Peter. We're here for our Paeds Round podcast, and it's my pleasure to introduce you. So, my name is Emma Lim and I'm a paediatric consultant at the Great North Children's Hospital, and today I've got Peter Day in the studio with me. Welcome Peter.Peter: Hello, Emma. Thank you very much for inviting me. It's a great pleasure to be here.
Emma: And where are you from? What do you do?
Peter: So, Emma, I'm a paediatric dentist, which is great. I don't have to see anybody older than the age of 16/18, and I get to behave like a child in clinic and try and make coming to the dentist as acceptable to as many children as possible. As a paediatric dentist, we see a wide range of patients, all sorts of different medical conditions, disabilities, as well as some quite complex dental conditions, whether it be genetic, traumatic or for us, one of the main causes of our work is dental decay, which is one of the most prevalent conditions in children.
Emma: That's great. And I think you've been humble, because you're just acting like you're just a dentist, and I think that's not quite true, is it? Because I think you have a real academic bent and a passion to talk about the state of children's teeth. So, you also work as an academic, don't you?
Peter: So, I’m a paediatric dentist a couple of days a week, I work in community dental services in Bradford, where I have a cohort of children with disabilities, and very much, many of them go to special schools or mainstream schools with additional support. And then in my clinics in Leeds, it's more of a multidisciplinary clinic, looking after children who traumatise their teeth, and come off their bicycles and other complexities like that. And then academically, you know, the great thing about my job is that I have a lot of variety, so I've got a bit of teaching, a bit of research, and as you've mentioned, Emma, I work for University of Leeds as a professor of child health, child dental health sorry.
Emma: I thought you were suddenly going to make yourself a paediatrician there.
Peter: No, I'll leave that to you!
Emma: And we’re talking today because you wrote this incredible report last year, that actually everybody should read, which focused on children of the North. And the headline was that tooth decay has a direct impact on a child's quality of life, and we should be shocked at the poor condition of many of our children's teeth. So, what are the stats? What does that actually mean?
Peter: So, Emma, before I start, I would just like to say it was a team effort, and my colleague, Zoe Marshman, who's professor of dental public health in Sheffield and many colleagues got together in early February 2024. We had a really good day, you were there Emma, and we got to summarise child dental health and explore the preventive aspects of how we can improve the current situation.
You're totally right. Children's oral health is in a crisis and is unfortunately not improving as much as or as quickly as we would like.
Emma: ‘Children's oral health is in a crisis,’ that's a strong statement. What are your statistics to back up that?
Peter: Unfortunately, that's true. It is a crisis. If we look at different age groups, so 10% of three-year-olds have decay, by five it's up to a quarter of children, so one in four, and those are both related to primary teeth. But when we look at permanent teeth, at 12-year-olds, it's a third of children, and by 15-year-olds it's up to about 45%, so almost every other child has decay in their teeth by the age of 15.
Emma: Actually, that's terrible. That's shocking!
Peter: Unfortunately, it is. And it's not just counting, but it's the impact that decay has, and that's around, you know, child development, inabilities to sleep, to eat, to talk and to do everything, the normal things that children like doing, like going to school and playing. And its impact is not just on the child level, but on their wider family, society and obviously, health and education.
Emma: That is actually, really shocking. So we said every other child by the age of 15 has some form of tooth decay, as you said, there's the pain, there's the drugs that children take for pain, there's school days missed, and there's the impact on the whole family, so taking time off to get them to the dentist, all those other things, that's huge. If we drill down on that a little bit, you've talked about the impact on the child, but what is the impact on the health service?
Peter: So, the most common reason for children to come into hospital is for dental reasons, twice as common as for ENT procedures. And almost invariably, if they're coming into hospital, they're coming in for a general anaesthetic to have, almost always, teeth extracted, but sometimes dental treatment, so it might include fillings. The cost to the NHS is about £40 million for those admissions. There are over 27,000 children waiting on those waiting lists, with some children waiting up to 80 weeks to get to the top of that list. And often those are the disadvantaged children, often with significant morbidity and disability as a result of their weight and then obviously it can affect their medical conditions as well.
Emma: That is actually so shocking. So, you're telling me that the most common reason to have a general anaesthetic is for tooth extraction, for decay?
Peter: Correct Emma, for children aged five to nine years old, admission to hospital, which almost invariably is for extractions under general anaesthetic, is for dental reasons. It's over twice as common as for ENT procedures. And there are over 27,000 children waiting on that waiting list, costing the NHS over £40 million, just in that particular aspect of treatment, and some of our children are waiting over 80 weeks to be seen, and often those children are the most disadvantaged, many with additional disabilities as well.
Emma: I’m just speechless. I'm just thinking about that £40 million just to pull teeth now. I mean, what else could we do with that £40 million? Why aren’t we using it in preventative health? Because, if we are honest about this, this is a preventable problem.
Peter: Absolutely, almost all tooth decay is preventable. Sometimes enamel, can erupt through which is not as well formed. But we get the teeth that we get. You know, with goods, oral health behaviours, we can prevent that decay. Certainly, if we do get decay, then it's around early access to the dentist to identify it and treat it early before it gets complex, and you need to be ending up in hospital with dental extractions under general anaesthetic, etc.
Emma: Let’s say we were going to use that £40 million earlier in preventative health, what are our options? What are things we could do? I mean, I've got four children, right? But I'm a paediatrician, and it is like the law of the land you cannot leave the house in the morning until you brush your teeth. And I sat over my children and brushed their teeth till they were about seven. But I think I'm probably an outlier, so come on, what should people be doing? What are people doing?
Peter: So, Emma, as in our report, we had a number of key recommendations, but one of them was very supportive of the government's plans to supervise tooth brushing clubs. The approximate cost is around £10 million and that is targeted at the most deprived 20% of children, specifically focused on children aged three to six years old. So, this is nursery and early years of primary school. This is basically supervision, and often uses additional staff within schools, rather than teachers, to support that activity where children brush their own teeth, and that activity happens every day, at some point which is convenient to the school during that day. And for some children, that is the only time their teeth get brushed in the week. And so, five times a week is better than no times a week. And I think you're right, Emma, the behaviours that we do at home are absolutely critical to having healthy teeth and growing up with a healthy dentition and good dental health, but for some of our families, those behaviours are a struggle to embed and implement, and so supervised tooth brushing can be very effective.
Emma: Yeah. I mean, that's really fascinating, isn't it? I mean, we totally accept breakfast clubs, so children go to school and have breakfast clubs. So, my children will brush their teeth after eating, so that seems like a really normal thing to do. I think that one of the things that people don't realise is what poverty looks like and what resource poor areas are like to actually be in and to grow up in. So you and I have done some work with, for me the West End Food Bank in Newcastle, and you're obviously in Leeds, and we're meeting families who can't afford toothbrushes, who can't afford toothpaste, who can't afford clothes, who can't actually afford meal planning, and I think that's a really different space to what people are used to, and maybe what you're used to from your own background.
Peter: Very true, Emma. I work in Cllefly as part of my clinic, we have some wonderful local community groups and community kitchens, and support and food hubs, and as part of that provision, we work very hard to enable them to give out toothpaste and toothbrushes. The supervised toothbrushing programme, which is proposed by the government, involves not just toothbrushes at school, but potentially for them to take home during holidays and other times, so to encourage those behaviours in the home setting as well. And often the feedback from children and their parents is those activities do help to support and drive behaviours at home as well, and obviously you do need the tools, but toothbrushing requires a little bit of some other parenting skills, more than just the actual toothpaste and toothbrush, it's that ability to support and enable and plan for your child to brush their teeth as part of the daily activity.
Emma: Yeah, I think that's really true. I mean, I see school as a place where you're learning skills. Now, you learn a bike, you learn to eat healthy. Why should you not learn how to brush your teeth? So, I want to know two things, what is supervised tooth brushing, first off, and what’s the evidence it helps?
Peter: So supervised tooth brushing is undertaken by children aged three to six years old, in nursery and in school, often the toothpaste is applied to a tissue and a small pea sized amount, and each child has their own toothbrush. They have special racks, which are disinfect-able and cleanable, so it makes it as clean as possible. And the supervision is to ensure that the right child picks up their own toothbrush, that the child actually brushes their own teeth, often with an activity and a toothbrushing song to encourage that brushing for a couple of minutes. At the end of that, the child often spits out any excess residue into the tissue, and the toothbrushes are then washed under a tap and replaced in the hold, dried and replaced in the holder.
Emma: Oh, yeah. So, I found this really interesting. So, it's a pea sized amount of toothpaste, it goes on a tissue, they put it on their own toothbrush. They brush their teeth for a couple of minutes, spit it put no rinsing. I couldn't get my head around no rinsing! I spent my life rinsing my mouth. I didn't realise I wasn't supposed to rinse it off, and then cleaned and dried.
Peter: Emma, I was in clinic on Friday, and my dental nurse had a really good suggestion. When you put, and I'm sure you don't, when you put your face cream on, the last thing you want to do is then wash it off. And the same as with toothpaste, we want it to stay on the team and have that that impact.
Emma: Yeah, I love it. Love it, yeah. Why am I washing it all off. Alright, so we know what we're doing now, what is the evidence that watching somebody brushing their teeth makes a difference to their long-term oral health.
Peter: So, the evidence predominantly comes from Scotland, where they have a national program already. The evidence is that it reduces dental decay in young children. It reduces health inequalities, so those children who are most in need, have the most benefit. And it's cost effective in that it saves money. And they reckon from the calculations in Scotland, that within three years, it paid for itself in less costs to the health service as a result of the implementation of the supervised tooth brushing program.
Emma: So, you're telling me, in three years, supervised tooth brushing paid for itself by reducing dental decay?
Peter: That is the data from Scotland. There's a different health economics tool called Return on Investment, and over a five-year period, for every £1 you spent on it, you got £3 back.
Emma: Why don't we do this earlier?
Peter: And what's so exciting is it reduces health inequalities, which often are public health interventions, wider health inequalities, and in this setting, they reduce them. And probably the reason is, because some of our most disadvantaged children, they're getting to brush their teeth five times a week, which wouldn't happen otherwise.
Emma: Absolutely, just like school meals. So, really fascinating. And I think it's so true, because you teach a child and they actually go back and teach the family, and there's good evidence that happens with all sorts of different skills. So, yeah, I'm like, you know, we could stop now, you said it. I'm converted!
Alright. So, we've talked about supervised tooth brushing, we've talked about how simple it is, we've talked about how much it saves money. We've talked about the impact on children from the most resource poor areas, but there are other ways to reduce dental decay. And I know that toothbrushing, you know, that's your baby, isn't it, but there are other babies around there. You want to touch on those other children. Those other options.
Peter: So, Emma, you're quite correct. It's around reducing sugars and increasing getting fluoride on the teeth. If we focus on sugars, it's around reducing sugar consumption. And certainly, when we're looking at national interventions, the soft drinks industry level has had a significant impact on children's dental health.
Emma: Yeah, I'm passionate about this. This drives me insane.
Peter: So, there's some really nice research led by a lady called Dr Nina Rogers, and she summarised it very nicely, so I'm going to steal some of her descriptions. So, the WHO advice is that you should have 30 grams of sugar per day. But the reality is, in adolescence, it's probably more like 80 grams a day. And adults, it's around 50 grams a day. And to put that in context, for chocolate bar and others, chocolate bar is about 20 grams, and we know that sugar is in many, many different processed foods. The current tax is got two levans. Above eight grams per 100ml was a certain tax level, and then between five and eight grams per 100ml was the next tier and then below five grams, there was no tax. And what this helped was not only bringing in revenue, but industry reformatted and reformulated foods to reduce the sugar count.
Emma: I think the interesting thing about the sugar tax is, it's one of those things that people want to beat parents over the head with a stick. But the difficulty is thinking about why you make those choices. So, the people and the family buying processed food, are the families who can't afford fresh food. So, if we put it this way, my children drink milk, water, and once a day, if they're lucky, they drink half a glass of fruit juice, which I used to dilute with water when they were younger. And I actually don't give them fruit juice, but that's expensive. So fresh fruit juice is really expensive. Fresh fruit is really expensive, and processed drinks like Coke and fruit drinks that have all that hidden sugar in, are really cheap, so this is also about the choices you have when you don't have a lot of money,
Peter: You're totally right, Emma, and our recommendations were to reduce sugar, but that was to apply the soft drinks industry levy to other sugared sweetened beverages. So that includes the Fruit hoot, other products of the same ilk, as well as some milk-based sugared, such as milkshakes. So, we wanted to apply that to other sugared, sweetened and beverages, restrictions of food marketing and advertising and promotions, and restriction of sales of caffeinated energy drinks for the under 16s.
Emma: Yeah, I mean those energy drinks, the whole Prime craze where every child wanted really expensive energy drinks because of the sort of social media push. I found that really, really bizarre, and it really took off! My daughter lives in Singapore, and she says, while they don't snack on like sweets and crisps, they have high calorie energy drinks, all these boba teas, milkshakes, very fancy looking drinks. And I absolutely see this craze coming in here in the teenagers. I don't know how to stop it, if you've got any idea. This has become very political, putting a tax on sugar, and I still fail to see why. Because we tax alcohol. This is basically the alcohol addiction of children and young people.
Peter: Emma, I totally agree, and I think we need to, you know, look at the evidence that the soft drinks industry levy actually had an impact on oral health, in that it reduced the need for general anaesthetics for dental care. As, you know, as the work by Nina Rogers has shown. And so that's really important. I think also it's that we sometimes look at it as an adult, as opposed to a child. And if we can look at it from a child's point of view, having toothache is rotten and having a significant impact on their quality of life and their ability to go to school and have a good wider engagement with wider activities.
Emma: Yeah. Okay, so sugar is evil. We've agreed on that. In fact, we need to start disagreeing. There's too much agreement going on here!
Peter: Emma, at an individual level, we try and keep, certainly, the advice we give parents, very simple, and that's very much to say, pretty much all food, apart from water and milk, have sugar in. And therefore, it's trying to resist snacking, and trying to have your meals in three or four groups, and allow your teeth some time to recover afterwards, and that last hour before bedtime to avoid sugary foods and drinks and overnight, if the child wakes up or needs a drink in the middle night, then the safe drink is water,
Emma: Yeah, and this absolutely chimes with all the evidence on obesity that don't snack, have three meals, try not to eat processed foods, try not to eat sugars, drink water. I spend my life in clinic, telling everybody this message, drink water, drink milk, don't snack. I usually say, by this point the children look like they hate me, and everybody is like making faces at me, and I say to them, my children are allowed treats on Friday. Friday is the end of the week, it’s treat day. They can choose a treat on Friday. And they're like, do you mean just once a week? And I'm like, yeah that's the world we live in.
Right. So, sugar tax. I mean, I find it shocking that we haven't done this earlier. I find it shocking the impact of the soft drinks industry and if I'm being honest, and this will heavily be cut now, I find it shocking the influence they've had. And I'm just going to leave it there. We've just got time to touch on fluoridation. Why this is helpful? What's the evidence that can reduce dental decay?
Peter: Water fluoridation, new government legislation means that the powers around water fluoridation are now held centrally, and like sugar taxes, it is a central government decision. So, some parts of the country, fluoride occurs naturally in the water, and up to one part per million is where the evidence is to show it's effective and it reduces tooth decay. In other areas of the country, such as Birmingham and Newcastle, they are fluoridating the water to achieve what is already achieved in some of those natural areas. And there is strong evidence between those, between when you compare Newcastle and Birmingham and other parts of the country, of an improvement in children's oral dental health as a result of that fluoridation and less need for that dental care under general anaesthetic and less dental decay.
Emma: Fascinating. I didn't know that some places had enough fluoride in the water naturally, and basically, you're just supplementing it in the areas with low level fluoride. So, why is anybody ever making a fuss about fluoride? It's like the anti-vaxxers. I'm just going to say it. And this surprises me, if it's there naturally, what is all the fuss about? Because there's a kind of anti-fluoridation lobby that I view as similar to the anti-vaccination lobby that seems to get a lot of airtime and has little evidence. But tell me, tell me a little bit about this.
Peter: Emma, I agree with you, there is a recent government report out in the last few weeks, which again reassures and confirms the safety of water fluoridation both in the benefits of the dentition, but also the wider concerns which people raise, and the lack of evidence that this water fluoridation does any harm.
Emma: Great. Okay, so we've solved that one! You told me you wanted two minutes to talk about something more important than fluoridation.
Peter: So, these are mid-level community interventions where we're trying to integrate the child workforce to support oral health as they do many other public health messages, and that's working with key people like health visitors, family hubs, schools, and nurseries.
Emma: Absolutely, and I think that you're right, there has been a divide between what happens to the school and what happens in public health and what happens in hospitals and primary care, and actually, we’re all singing from the same hymn sheet. We've all got the same message, and we need to work together and pull together, and especially through something as simple and effective as cleaning children's teeth. So, Peter, one of the things that is a real issue with adults is people say they can't find the dentist, or they can't get on to a dentist, or they can't get on the waiting list for a dentist. So, tell me about dental access to children. Is it a problem?
Peter: Yes. We know, the latest figures show that only half of children go on a regular basis, and we need, as our report explains, to try and reorientate dental service to be more preventative focussed, but that importance of early access to enable us to diagnose early and treat early if there is decay, and, more importantly, support the families to integrate those oral health behaviours at home, because that's the most important behaviours are what's happening at home.
Emma: So, you’re telling me that 50% of children don't go to the dentist, but actually, visiting the dentist is free for children.
Peter: Emma, you're quite right. Dental access for children is free. And as a national society, British Society of Paediatric Dentistry, they would like to get that regularity of dental attendants, from their first birthday onwards so we can get those preventive habits in, and you go and have simple and easy visits, because there is no pathology, and it is a joyous visit for everybody, because it's positive and it's simple, and the child develops these good routines and supports the wider family.
Emma: And that's actually true. As I was telling you, I still have four children, and my life's achievement is that I managed to get my children well, they're not all yet 18, but so far up to the age of 18, none of them had a hole.
Peter: Emma, that's fantastic. And we know that, you know, for children across many areas of society, that is what we should be aiming towards, and many Scandinavian countries achieve it.
Emma: What is the problem? Because there aren't enough dentists, or it's too difficult to get to the dentist for children? Why? Why are they not going?
Peter: I think it's a number of things. I think access is a challenge, and obviously there's a whole wider piece of work around dental contracts and dental workforce. National funding for dentists is stagnant and hasn't risen as other areas of the NHS have.
Emma: You've told me that actually national funding is stagnant, but funding is now devolved to ICBs (integrated care boards), so it's up to your local area or region to decide how they want to provision dental health. So, what does that mean?
Peter: So, this is a really exciting opportunity, because it's got that local control, enabling the integrated care board to choose where it locates dental services, to improve access. And also, there's an example within the Yorkshire region, where it can prioritise access to certain vulnerable groups, such as those children with additional needs.
Emma: Fantastic. Okay, last off, when I was a child, and when we lived in New Zealand, we had school dentists, and the school dental bus came. It parked up for a week. Every child in the class went in. They had a nice time. They were supported by the teachers. They got their free dental care. It was all on site. It was so efficient. Can I just say, why don't we have school dentists again? School dental bus?
Peter: Emma, you've opened a large conversation there. So, working in Keighley with our app locally group, you know, schools have raised the question, like many other health services, why can't we bring health services into schools? And I think in some settings, certainly where access to local dentists is quite challenging or quite far away, then that might be a way forwards. But where a dentist is, say, co-located five doors down the road, and you've got a 10-surgery dentist, it is far more efficient and effective to deliver dentistry over 10 surgeries, than it is in one surgery with all the challenges around transport, sterilisation and everything else.
Emma: Sure. Okay, fascinating. I think I'll move back to New Zealand!
Peter: That said in schools, there are certainly opportunities around the preventative piece are very important and certainly should be delivered in schools, the dental services, some of the things that we're working with in Keighley is trying to get that relationship between schools, because what schools were finding was one of the many causes for children being off school is dental reasons, and that working between dental practices and schools and almost allowing schools to prioritise those children most in need because of their loss of education, to be able to access that dental service.
Emma: Fantastic. It's been a real pleasure talking to you today, and it's made me think a lot about oral health, the state of children's teeth, and what we can do about it. You have one minute to give us your top tips. So, what are your top tips?
Peter: So top tips for children's dental health are three things. One is brushing twice a day with fluoride toothpaste, limiting sugary foods and drinks, and water and milk are the only safe drinks and regular dental visits, are my three top tips. I can go into more details on all of them, but that's my headline figure.
Emma: That's brilliant, and I absolutely agree. And for me, I'd say, don't snack, don't rinse your face cream off or your toothpaste off, and drink water. And also, I love the idea that we should work with the ICBs, the integrated care boards and education to all be using these health messages and promoting such a simple preventative health issue as one group, because we all believe the same things. We spent too long agreeing today. So, we just ought to all work together.
Peter: And I think integration is the way forward, Emma and you know, as a child workforce, having a dentally healthy child population is as important as many other aspects and improves the child's quality of life.
[music starts]
This podcast is produced by Odland Education. The views, thoughts and opinions expressed in this podcast relate solely to the speaker and not necessarily to their employer, organisation, the Royal College of Paediatrics and Child Health, or any other groups or individual. You can find a wealth of information on the important work of the Royal College of Paediatrics and Child Health on rcpch.ac.uk, or #choosepaediatrics.
[music ends]
-
EPISODE 14: The guardians of the antibiotics
Antibiotics have a huge impact on delivering health care and reducing mortality – about a third of children in hospitals are taking these medicines - but the threat of antimicrobial resistance is real. Dr Sanjay Patel, a consultant in paediatric infectious diseases and immunology, talks to hosts Emma and Christo about its causes and how we can improve antimicrobial stewardship for the benefit of all patients.
Dr Sanjay Patel is a Consultant in Paediatric Infectious Diseases and Immunology at Southampton Children's Hospital
[Music starts]
Sanjay: We are going to run out of antibiotics if we're not careful, because you only have to steward something if it's a finite resource.
Emma: I think the thing that holds everybody back from not prescribing is fear.
Sanjay: So many of our paradigms are being challenged.
[music ends]
Emma: Good afternoon, and that's our countdown to our next episode of the Paeds Round. And it's my huge pleasure to welcome an old friend of mine, Sanjay Patel.
Sanjay, it's a pleasure to introduce you. And Sanjay is a paediatric infectious disease and immunology consultant working at Southampton's Children's Hospital in the UK. And actually, Sanjay, you are a kind of polymath. You are interested in so many different things, but particularly outpatient parental antimicrobial therapy (OPAT) and antimicrobial stewardship, which is what we're going to be talking about today. And Sanjay holds a title as the officer for stewardship and surveillance for the British Society of Antimicrobial Chemotherapy and chairs the Paediatric Network of the ESCMID study group for antimicrobial stewardship. So, I think that makes you really very well qualified to talk to us today. Welcome.
Sanjay: Thank you, Emma. It's great to be here. Lovely to see you again.
Emma: So, what we're talking about today is stewardship, and stewardship is such an interesting work because there's something about supervision, but it's also something about taking care or looking after something that's worth protecting. And I guess it's about responsible and careful use of antibiotic medications, to ensure their effective use for current and future generations. And I guess that's why in paediatrics, we find it so important, because it's children now and their future.
Tell me a bit about why you feel we should all care about antimicrobial stewardship.
Sanjay: Would you know, before I do that, I think the term stewardship, you raise this, it is an interesting word. It's really interesting, isn't it? It does rely on the fact that we are going to run out of antibiotics if we're not careful. Because you only have to steward something if it's a finite resource, you know, if it's an infinite resource, and you've got a cupboard that's got more and more and more antibiotics you can delve into, then you don't need to stewardship, steward them at all. So, we are talking about something that has beyond sanitation and access to clean water and vaccines having the greatest impact on the delivery of high-quality health care and reducing mortality out of any intervention we have. So, it's something that clearly we all love.
Christo: Thank you very much, Sanjay. So why does antimicrobial stewardship matter, particularly for us as paediatricians?
Sanjay: So, Christo it's really important for us, because we use a lot of antibiotics. And when we look at the data on children in hospitals, we see, and people will know from their own clinical experience, that about a third of children in hospital are on antibiotics. And then in addition, we have a proportion of children yo-yoing in and out of hospital, on intravenous ambulatory antibiotics. So, it's a big proportion of the children we look after.
Emma: Well, I think the one thing that we can take out for this is that antimicrobial stewardship is important. It's important for three different reasons. It's important because, actually it's thinking about your prescribing patterns, patient safety minimising side effects. Is thinking about, how do we prevent resistance? Are we thinking about this idea of protecting this resource and preserving the effectiveness of antibiotics?
Christo: And as you say, Sanjay, it's something that we use a lot of, so it's worth us taking the time to think about how we can do it properly, because it does form a big part of our working day.
Emma: So, if we take those points one at a time, let's think through the cornerstones of antimicrobial stewardship. Let's break it down into the three really important questions about antimicrobial stewardship: why, who and how we do it?
Sanjay: Yeah, I think that's right. I think that's a good way to break it down. I think the why, there are loads of reasons why, actually, first and foremost, relates to antimicrobial resistance. So, I think every clinician listening to this podcast will have noted that they're seeing more and more Rs along the microbiology results of children presenting with urinary tract infections and other infections, and that's because bacteria will naturally become resistant if exposed to antimicrobials, antibiotics, and so that's the main reason why we have to start thinking about antimicrobial stewardship.
Emma: Brilliant. I think that's such an important point that actually, when you give a child antibiotics, you might treat that infection, but you actually are just going to increase the number of bugs that are resistant to that antibiotic. So, it is an inevitable fact of using antibiotics that you get resistance.
Sanjay: Absolutely and clearly with everything, there's a risk benefit ratio. So, if you know that the child is going to benefit from antibiotics, and that benefit has to be a quantitative benefit, either in terms of mortality or the length of their symptoms or morbidity. So if we have evidence based approaches to knowing which cohort of children benefit from antibiotics, so if you've got a child with invasive group A strep or meningococcal disease, there is no way we're saying, don't give them antibiotics, but we are saying that for a child with mild pharyngitis or a lower respiratory tract infection that's likely to be a viral etiology, the harms for both the patient and the population outweigh the benefits
Emma: Absolutely.
Christo: So, apart from trying to prevent our patient in front of us getting colonised with resistant bacteria, are there any other benefits that we can think of for that patient rather than just thinking about the population?
Sanjay: Really good question, and you're right, this whole concept of population resistance is so abstract that I struggle with it, and I think all of us do to some extent. We look after individual patients as frontline clinicians. And those benefits are also that when children are starting on antibiotics, and probably if we're honest with ourselves, we know that they're invariably going to be intravenous antibiotics when they're first started. And that's what all the evidence shows hen we look at UK prescribing in hospital. Then those children are more likely to stay in hospital than if they’d been started on oral antibiotics or had an early switch. So, it impacts on their length of stay, which we know that that's so costly for so many families. I think that that tangible benefit or impact financially and, on the wellbeing, and happiness of that family is massive having children in hospital unnecessarily.
Emma: Sanjay, that's a brilliant point. You're absolutely correct. It is really expensive being in hospital for families, not just financially, but also lost work and finding childcare for other siblings who may remain at home. And so many families are now on zero hours contracts, so that has a huge impact. So, trying to keep children at home is really vital.
Going back to other points, I think this is a really growing area of knowledge and something that we didn't used to think about. But what is the impact of antibiotics on a child's normal microbiome? Because we know even from pregnancy, antibiotics affects children's microbiome.
Sanjay: Yeah, I think you're right. We don't totally know, but there are enough signals to suggest that we are having a long-term impact, in many ways, on children. And personally, I think the earlier they're exposed to antibiotics, the bigger that impact perhaps is. And so, I think this really speaks to that neonatal prescribing bit. So many neonates are getting antibiotics unnecessarily. You look at the rates of early and late onset sepsis, especially early onset sepsis, it's now down at one in 1000 less than that, nought point three in 1000 and yet, in some hospitals, 10 to 15% of all babies born in that hospital are starting from antibiotics. So, the answer is a big impact. We don't know all of the impact but definitely focus on neonates and try and reduce unnecessary exposure to antibiotics, because it is having an impact on their microbiome.
Emma: So, I guess that brings me round to if you are sitting there wanting to prescribe, do you have any tools or resources to help decide when to prescribe and when not to prescribe?
Sanjay: Yes. So, you raise a good point. I mean we need firstly, that decision point of when a child presents, what's their diagnosis, and it's always diagnosis, diagnosis, diagnosis. It's like when you're buying a house, it's location, location, location. And this is the same, if you start off with the wrong diagnosis, you end up on the wrong decision tree, treatment pathway, and harm will befall the child, which may be unnecessary exposure to antibiotics from another misdiagnosis. So, let's assume you've made a correct infection diagnosis.
Emma: I love that. I think you're so right. It's about diagnosis, diagnosis, diagnosis, and I guess the question then is, what we really need is better tests and better quick bedside or point of care tests?
Sanjay: Yes, it still comes down to clinical acumen as well. You know, I think some of this is people making the right diagnosis, your right tests and fancy novel tests will help, but they're not here now and we have patients in front of us now. So, there are courses people can attend, there's reading people can do, there are seniors that people can consult with. But diagnosis is important, once you've made the right diagnosis, my advice would be to look at the BSAC common infection pathways. We and in my role within BSAC, with lots of colleagues around the country, have developed some really straightforward pathways that you can follow that make you think about the differentials and walk you through investigations, assessing severity, management and treatment, and that you'd find online if you type in BSAC paediatric pathways into Google or any search engine, you'll come across the 12 or more that we've developed.
Emma: Thank you. Yeah, I think that's really important, because there's something about having consistency, getting everybody to do the same thing, making a diagnosis, and especially if you choose to make a diagnosis and not treat, is something that sits with us badly. We all want to do things. So sometimes it's about holding back about that risk, about waiting to see what will happen. And I think if you have a pathway to follow, a paediatric pathway that takes you through and weighs up all the evidence, that's really helpful. So, the British Society of Antimicrobial Chemotherapy, as you say, their paediatric network has a series of paediatric pathways. We also have regional pathways on Healthier Together which would work for your region. So professional pathways agreed within a local area between an ICB. So, I think that is a really helpful way to look at thinking about the diagnosis and deciding what is the evidence you really need to give antibiotics.
I think the thing that holds everybody back from not prescribing is fear, and it's always the fear of missing sepsis and serious bacterial infections. But actually, we know these are rare events, so serious bacterial infections, if you look at paediatric emergency departments, that's only 10 to 30% of children presenting with fever, and sepsis in that scenario is about 1%, so what do you think about fear, sepsis and antibiotics?
Sanjay: I think a lot about this because, as you say, the commonest reason children are started on broad spectrum IV antibiotics is that they're labelled with a diagnosis of sepsis when they walk in the front door, because they're either tachycardic or tachypnoeic. And our current kind of screening tools for sepsis, and even that term is a complicated term of very poor specificity, so a lot of false positives more importantly.
I think this goes back to the diagnosis, diagnosis, diagnosis discussion. I think that if one can make a diagnosis and have the time to make a diagnosis of the site of the infection, you go down an appropriate pathway, and we have more and more evidence for many conditions, including osteoarticular infections and pyelonephritis, that starting a child on oral antibiotics is just as effective as starting on IV antibiotics. However, to do that, you need some time, and so the approach taken by the Academy of Medical Royal Colleges is a permissive approach to sepsis, where, clearly, if you have overwhelming sepsis, you get antibiotics within 30 minutes. If you've got a suspicion of sepsis, there's no evidence to say that withholding antibiotics for two to three hours befalls any harm to the patient. Do that, do your investigations and work out if they have an invasive bacterial infection and where it is, and then follow the appropriate BSAC common infection pathway.
Emma: So, if we just think about that really important point, if a child is really unwell, low blood pressure, and they clearly have sepsis, yes, absolutely you need antibiotics within a short time frame, 30 to 60 minutes. But for the other children who you're just suspecting sepsis, you have time to do tests. You have time to think about what's wrong. You can give them antibiotics, but think, do they really need IVs? Do they need orals? The point of having them in hospital is you have them in a safe place where you can observe them and take time to make the right decision and not necessarily treat everybody with broad spectrum ceftriaxone.
Christo: Thanks, Andrew, that's clearly really important, and in terms of picking the right antibiotic when you think that you've got a child in front of you where you are seriously worried about sepsis. How do you go about that? What resources are there to help?
Sanjay: So, there are two approaches. One is what you do empirically when you don't have microbiological results, and the second is, what do you do once you get those microbiology results back. And so, to make a good choice about empirical antibiotics requires a lot of you know, a lot of knowledge, actually, about patient related factors, bug related factors and antibiotic related factors. And to make that process easier, we should be using guidance and guidelines, and we have excellent national guidance produced by an organization called UK PAS, which is the UK Paediatric Antimicrobial Stewardship Network. And under the guidance of Paddy McMaster and our colleagues in St George's, there are really good evidence based, expert supported guidance on all common infection phenotypes. So, I’d just look up UK PAS, or on EOLAS App. If you go into the space or organisation called UK PAS, you'll find that you'll have access to that guidance, and that reflects the sort of resistance patterns of organisms in the UK, etc.
However, every clinician has to also manage the child in front of them, and so if they've come from an area of high incidence and resistance, say they've come from a hospital in India, then you have to think, are they appropriate for following the guidelines? Or if you've got microbiology results about what they're colonised with, or what they have at the time, then the empirical guidance may not be appropriate.
Emma: Brilliant, so vital. It's really important, when you have a child in front of you, to take a history, to think about where they've been, to think about the site of the infection, source of the infection, and to read any old medical notes and look up all the old results to see if they're already colonised by a resistant bug.
I have to tell you, I'm a huge UK PAS. That's the UK Paediatric Antimicrobial Stewardship guidelines fan. I send everyone there because it's really clear and it's beautifully evidence based, like you just look at it, there's all the evidence. It gives you an antibiotic choice. It gives you a choice if you know that they have a penicillin allergy. It puts all the information in one place, and it gives you some idea about duration and dose, and I guess that brings me to thinking about appropriate doses and shortest duration.
Sanjay: So, we're lucky in this country because we've got the BNFC. And actually, the BNFC is our kind of Bible for prescribing in terms of dosing, not all antibiotics, especially some of our novel antibiotics, which aren't necessarily licensed in children are in there, which is why we have to work very closely with our pharmacy colleagues and within our networks, our regional networks or national networks. And that's where an organisation like UK PAS could be really helpful. In terms of duration, I think UK PAS guidance is excellent, because it tries to summarise and take account of the evidence that we have currently in terms of shortening antimicrobial courses. And many of you will remember a few years ago, 10 years ago, for a gram-negative bacteraemia you treat for 14 days, we now have excellent evidence from adult studies, which are now applied to children, that seven days of antibiotics is absolutely appropriate for those children.
The other big shift has been in IV to oral switches. So, we now recognise that oral antibiotics are just as good as IV, except if you have overwhelming sepsis where your gut doesn't really work and you don't absorb antibiotics well. If you don't have a gut or a working GI system, or if you've got a CNS infection, and that last one, you know, watch this space. That may change too. But for those three reasons we give IVs, I struggle to think of many other indications for IVs, and that includes neonates.
Emma: Thank you, Sanjay, that's absolutely brilliant. We need to be clear that actually the times when you need IV or intravenous antibiotics are when you have sepsis, where you need high levels of antibiotics in your blood quickly, you need IV antibiotics if you've got gut failure and you might not absorb and we've also thought about it in CNS, Central Nervous System infections, and I think that your point about all these guidelines are on UK PAS and they're also on EOLAS, this is a platform that holds hospital guidelines. So, you may have guidelines that are local to your area, and we keep all our guidelines on EOLAS for paediatrics, but also for other specialties. So, it's really great resource as well.
So, thinking about the children that do need IV antibiotics, when can you switch them from IV to oral? Because we really need to think about how quickly can we get them out of hospital? How quickly can we get them off IVs?
Sanjay: So, for most children, you can switch very quickly, actually. So, for most children, once they are clinically improving, once they're inflammatory markers, if you decide to recheck them are improving, then if they don't have one of those three categories, or if they don't have gut failure or meningitis, you can do an early switch to oral antibiotics.
I would be a little bit more careful with very young children under a month of age. But that said, there are some lovely data coming out of out of Holland and out of Denmark, showing that neonates treated with all antibiotics with confirmed early or later onset sepsis have outcomes that are identical to those treated with IV after initial periods of IV antibiotics. So, many of our paradigms are being challenged. There are obviously some children that need to be treated with prolonged courses of IV antibiotics. And I think if you need to do that, you need to do that within the safety of a well-managed, well clinically governed system and OPAT service, I'd call it, and that stands for outpatient parental antimicrobial therapy. And we've developed national guidance on the approaches and the systems you need in place to deliver high quality care to those children.
Emma: That's great advice. So, I think remember thinking about that IV to oral switch. Are they clinically improving? Have their inflammatory markers like CRP or Procalcitonin reduced? Are they older than a month of age? Those are the easy ones where we know they can switch. And have you got a definitive diagnosis? So, do you know which bugs that you're actually trying to treat?
And I think it's really important to remember that just because you're changing them to oral antibiotics, it doesn't mean that you're not taking great care of them and watching them carefully, watching their observations, their temperature, their improvement, as you say, that can be done as an outpatient.
So really, really fascinating. And I think the other thing is, is the savings are not just in bed days. These are in real financial savings. So, we know that IV antibiotics are more expensive. They take more resources, because you've got cannulas, you've got pain, you've got drawing up the drugs, all the other things that that takes and the nursing time. But even on another level, if you are prescribing antibiotics, you can prescribe the cheapest, best antibiotics. So often those are as pills. So, if we take the example of trimethoprim or Nitrofurantoin, really common drug, you can give the right number of days as pills. But if you use syrups in a bottle, you're often wasting the end of the bottle, because you'll use five doses and then the other five are just sitting in the bottle. Those wasted doses sometimes sit on the shelves to be used again or get tipped down the sink that pollutes our water course, or very rarely get returned to pharmacy. So, I think this idea about the financial impact of antibiotics when they're prescribed and used, as well as the environmental impact, is really, really important.
Sanjay: Yeah, do you know, Emma, there's another big impact, which is the ecological impact on the child and on the environment. Invariably, in this country, in the UK, when we prescribe IV antibiotics, we prescribe ceftriaxone, and when we benchmarked ourselves against a number of other European countries recently in the PERFORM study, we've shown that we love ceftriaxone, other countries, when they use IVs in children, they may go to narrow spectrum, but we love the convenience of a once a day antibiotic. If you prescribe all antibiotics, you will almost always be on a narrower spectrum antibiotic than ceftriaxone. And so, for the child, it reduces the evolution of resistant organisms in that child, but also when they pee and when antibiotics go into the surrounding ecosystem, there is a greater impact of patients on broad spectrum antibiotics around hospitals than if there are narrow spectrum orals. So that's from a resistance perspective. It also makes sense. It's better for the child, it's better for the environment. It's better from a green agenda perspective, which we're all taking very seriously, and it's cheaper.
Emma: Fantastic. Completely agree. I couldn't agree more, and the carbon footprint of antibiotics is huge. So, it's not about saving the cardboard and the glass of the bottle, the actual antibiotic footprint of the active drug is like 96% of everything. So, if you can save a dose, then you're saving resistance, you're saving the environment. You're saving the carbon footprint, you're saving money. So, it all goes back to your idea about think hard. Do you really need to prescribe this drug today? This time?
Christo: Clearly there are a whole host of benefits that come with embracing antimicrobial stewardship in day-to-day practice. But I just wondered if you have some tips on how we can actually do that in our normal working days?
Sanjay: Yeah, so many of the listeners to this podcast don't work in tertiary children's hospitals. I have colleagues within my team. I work with specialist nurses and antimicrobial pharmacists. But clearly that isn't the case in your average DGH in England or any of the devolved nations. And so we, and this is in my NHS England role as national political advisor for antimicrobial stewardship, we've been thinking about models we can use to try and improve how antimicrobials are used in hospitals up and down the country in DGHs, and that model has to use staff that are currently in place, so those staff are general paediatricians. They are pharmacists. They are nurses, often nurses that work in hospital, at home or ambulatory services. They are sometimes trust antimicrobial pharmacists who, in theory, cover all ages, but generally dedicate their time to adults and our microbiology colleagues, and so what we have successfully negotiated is for funding for four pilot sites, and this is going to start off in Bristol, Southampton, Evalina London and Sheffield, where we are going to empower infection teams across our regions. So, in my region, there are about 12 DGHs, include the Channel Islands and include the Isle of Wight. And we have identified a paediatrician, a microbiologist, pharmacist plus or minus, nurse plus or minus trust antimicrobial pharmacist to be involved in an education program so that we can share learning across all of us, and to benchmark prescribing, both in terms of the process of how antimicrobial stewardship is viewed within the hospital, and also how prescribing, how you benchmark against your similar hospitals in your region.
And so that's due to start in the coming couple of months, and I would love that sort of model to be rolled out across the country. And when we finish the evaluation and we show that it's reduced length of stay, it's reduced use of IV antibiotics, it's reduced cost, I have no doubt we'll be able to roll it out to every single region using the hub and spoke model.
Emma: Fantastic. I think that encapsulates all we want, we want antimicrobial stewardship champions. We want people to be thinking about this and about their prescribing habits. And really, my one ask to people is to collect data to see what you're doing now, so that Sanjay, when your fantastic model rolls out, you'll know what you're doing now, and then you'll be able to see, like, day by day, week by week, how to improve.
Sanjay, it's been absolutely brilliant talking to you. And like, there's so many pearls of wisdom, literally, and they're all rolling around at my feet now. And I just want to think which are the best bits. So, Christo, since you're my trusty sidekick, you've been listening to all of this. Which are the three best bits that you took out of it? What are the three learning points that you didn't think about that you've come away with today?
Christo: Firstly, Emma, I think it's really important that we get the right diagnosis. And Sanjay's point about diagnosis, diagnosis, diagnosis. And that leads on to the second thing that I've taken away from this, which is, once you have an idea as to what's going on, use the right resources to help you make decisions. So, looking at BSAC, looking at UKPAS, looking at local guidance, if it's different. And thirdly, it's been really helpful to focus on the situations where actually IV antibiotics do need to be used, so gut failure, sepsis, CNS infections, to help focus us on making a decision about when to when it's safe to switch to oral antibiotics as soon as possible to get kids out of hospital sooner.
Emma: And that only leaves me to say, Sanjay, thank you very much. It's been absolutely amazing talking to you. We've had a really great time, and I've learned so much. So as your last parting gift, what are your three top tips to our listeners?
Sanjay: My first top tip is to challenge paradigms. You know, I think we as paediatrician have loved IV antibiotics for a long time, and we need to reflect on that love and maybe use that love elsewhere. Because oral antibiotics are absolutely brilliant. And in fact, they have so many benefits for our patients that we've seen that with all the data, everything we believe that benefited from IV antibiotics, every RCT we've done has shown that orals are just as good if used, you know, the right dose, and it's palatable. So firstly, that's it, it is orals. Think about when you can use orals.
My second bit would be to not make antimicrobial resistance and stewardship a nebulous population thing. Bring it back to your patient. That's what we do. We look after individual patients and think about the benefits for your patient in terms of their microbiome, their side effects and getting them out of hospital, and also resistance in that child, especially if they've got complex comorbidities, which is increasingly the cohort of children we all look after.
And thirdly, make this a team effort. So, the team is your microbiology colleagues, especially your pharmacy colleagues. So, empower them with the UK HSA IV to oral switch tool. They should be challenging us. Our nurses should be challenging us, because they're the ones that have to give the IVs. They've got to spend half an hour drawing them up. We don't have enough nurses on the wards, you know make their lives a little bit nicer, and they're more likely to stay in their posts. Work with them, and they will support the work we're doing with antimicrobial stewardship.
Emma: Fabulous. Oral antibiotics are best, personal care for patients and teamwork, making nurses, pharmacists, resident doctors, everybody around you think about antimicrobial stewardship. So that's thank you very much to the whole team, to you, Sanjay, and please look at our resources below. You
[music starts]
This podcast is produced by Odland Education. The views, thoughts and opinions expressed in this podcast relate solely to the speaker and not necessarily to their employer, organisation, the Royal College of Paediatrics and Child Health, or any other groups or individual. You can find a wealth of information on the important work of the Royal College of Paediatrics and Child Health on rcpch.ac.uk, or #choosepaediatrics.
[music ends]
-
EPISODE 15: The Secrets of Sickle Cell
How can paediatricians offer patients with sickle cell disease the best possible care? How do we listen to children and young people, and their families, to help recognise and manage their painful crises?
On this month’s Paeds Round, Emma and the team are joined by Dr Subarna Chakravorty, a consultant haematologist, to discuss the NICE guidelines for sickle cell and thalassemia and the management of pain. The panel goes over how children of different ages experience pain differently, and why it’s important to bear in mind any co-morbidity issues and how can paediatricians offer patients with sickle cell the best possible care?
Dr Subarna Chakravorty is a Consultant Haematologist at King's College Hospital NHS Foundation Trust and Imperial College London. She has a special interest in non-malignant haematology and stem cell transplant for haemoglobinopathy and non-malignant diseases.
[Music starts]
Subarna: I mean, they are a very vulnerable group of patients. So really you have to believe the child or the family, who knows the child really well.
Emma: You need to be a sickle cell champion to these children.
[music ends]
Emma: I am very, very excited today, in November, in this horrible cold weather, to have a guest all the way from London to come and talk to us about one of the things that I think is really, really important and not talked about often enough, which is sickle cell disease. So, it's a huge welcome from me to you, Subarna, to come here and talk on the Paeds Round.
Subarna: Thank you. I greatly appreciate you asking me to come.
Emma: And just as a quick introduction, Subarna is fantastic expert. She is a paediatric haematologist. She works in London and has been working with sickle cell and Thalassemia for over 20 years and is the chair of the Hemoglobinopathy Reference group for NHS, England. So, who's better to talk about this than you?
You have nothing to say after that introduction! Okay, well, one of the things that I think is really useful for everybody listening is just to give us a little round up of the current sickle cell guidelines and the state of services for children with sickle cell in the UK. One of the things that strikes me is actually the NICE guidelines, so are actually quite old, so they're from 2012, so is that something that you think that we should think about, and what has happened since then?
Subarna: Yes, so the NICE guidelines specifically looks at the management of pain in sickle cell disease in the emergency department. And as you say quite rightly, it was published in 2012 and we haven't really had any updates since then. So that's not for the want of trying, though. In 2023 we went back with NICE to look at whether there was any new and emerging evidence to support or to change the guidance. But actually, what we realised was that there wasn't any. So, we decided as a group of experts to kind of leave the NICE guidelines as they were.
And the essence of the guideline is really the time criticalness, for want of a better word, of providing pain relief to children and adults or anybody with sickle cell when they present to the emergency department. And this has been the cornerstone of sickle cell care in the UK, really, we as sickle cell care providers really feel it's really important that this is provided in a timely manner, pain relief. And also, if you look at emergency departments themselves, they too, not just for sickle cell, but they have very stringent guidance themselves for providing pain relief to anybody that comes with pain. In fact, theirs is a little bit more stringent than sickle cell, so, there's, I think is 15 minutes.
But the sickle cell guidance goes a little bit further than the first dose of analgesia, which ideally should be within 30 minutes. What it does say is that the provider, the nurse or the doctor looking after that patient, should then return to the patient every 30 minutes to check the response of the pain relief.
The other thing that is very important and slightly different from all other sort of pain approaches in ET is that one thing that nice guidance was very clear about was that you should treat sickle cell disease pain as an emergency. And I think that is important to underscore, because patients are often and I'm talking about really young children here, three-four-year-olds will often be able to be able to somehow regulate their own sense of pain in a way that they don't have any external visible reaction to the pain. So, and this is such a human thing that when we see somebody in pain, we then go back within ourselves, to dig into ourselves, to see, you know, what is my reaction to pain? So, people might experience trauma pain, people might experience surgical pain, people might experience birth, labour pain, etc. But for people who haven't experienced sickle pain, it's very difficult. And you know, for children who have experienced pain all their lives, and I'm hoping, and I will talk about that later, I'm hoping with newer, better treatments, we are trying to avoid that now, but for children who experience pain all their lives, are able to somehow kind of distract themselves from the pain. So often they are withdrawn, they are absolutely still. They will often try and concentrate, maybe on their phone, on a game, or do something. And this is their own way of coping with the pain. And often this is interpreted as you know, you can't be in pain, you're on your phone. How could you possibly be in pain? And this, I find across the board, regardless of you know, the age of the patient, where a patient is being doubted about whether they're in pain or not.
Emma: Subarna, I think that's so important that the cornerstone of sickle cell care is about recognising and treating painful crises. And what I find absolutely interesting is your idea that actually it is only parents and children and families who can understand what pain looks like, and that you as a doctor have to take their word for it.
So, you had a really interesting point that you were telling me that pain and the kind of pain that your patients experience changes over their age. Do you want to tell me a bit more about that?
Subarna: Yes, so I think it's got to do with where the bone marrow is active as you age. So, when a very young child experiences sickle pain, usually with bone marrow infarction, they may experience something called dactylitis, which is a kind of painful swelling of their fingers and toes. This is where the physical manifestation of pain happens in children. But as the child grows, the pain often, and this is not universal, there are some exceptions, but by and large, the pain tends to become more central, so the child will then start to experience pain in their limbs, and as the child grows into a teenager, pain often is more central. So, they may experience pain in their ribs or pain in their back, in their spines, or their pelvis, and so it's almost like it goes centripetal. I'm really generalising here. There are exceptions, of course. So, apart from dactylitis, where you can see the swelling, there is no other external manifestation of pain. So really, you have to believe the child or the family, who know the child really well when they say they are in pain.
Emma: Perfection. Alright, so if we're talking about painful crisis, your top tips are first of all, listen to children and their families, believe them. Give them pain relief within 30 minutes, go back and check if that's worked and if they need anything else. And I guess we also have to think about other things, so make sure they're not dehydrated. They’ve got fluids. Do they need IV fluids? It's November. Are they warm? Do they need oxygen? Do they need antibiotics? Is there anything else we need to think about?
Subarna: No, I think you've covered it all. I think it's important to focus not just on the pain, but everything else that's happening with the child. So, a child might be in pain, but it may quickly progress to an acute chest syndrome. So, it's very important to ensure that the oxygen saturations are monitored, and antibiotics given as appropriate, and suddenly, this time of the year, you're looking to explore whether the child has any viral infections and support as necessary. And yes, hydration is extremely important as well, and keeping the child warm. Yeah, all of that is very important.
Emma: Of course, I'm an infectious disease doctor, so I'm always interested in antimicrobial stewardship. Now, if we have good diagnostics, we know that a child with sickle cell crisis has got flu, for example, I'm still a little nervous not to give them antibiotics, at least oral antibiotics, but I've got no evidence for that. Do you have any feelings? Because I'd love to give out less antibiotics, but I'm always too nervous. I end up giving them oral antibiotics. What do you do?
Subarna: I must be honest with you, I do the same. I might send them home on oral antibiotics even if they are positive for flu on the nasal swab, partly because, I guess I'm telling myself, I want to stop them from getting secondary bacterial infections. I mean, they are a very vulnerable group of patients, and we see pneumococcal deaths all the time, I have to admit.
Emma: Yes, I think this is a really good point. And I think this is an area where better diagnostics and better tests that would really reassure you and me there were no secondary bacterial infections, would make us a bit less nervous not to give them antibiotics at every point. And I guess in the future, what you would like is that your patients could actually test at home and decide if they had bacterial infections, if we had point of care blood tests that patients could use, but that's in the future. So, for now, pain relief, oxygen, warmth, antibiotics and just really, really good care and paying attention to detail.
Subarna: Absolutely, and may I add that actually universal vaccinations with Prevenar, and we also add Pneumovax, which is the PPV 23, has actually been shown to make a huge difference in outcomes, particularly with pneumococcal related deaths. So, part of good care, preventive care, vaccinations are very important.
Emma: Absolutely. And flu vaccine. Flu vaccine for everybody, perfect.
And so, I think let's ask a little bit slightly different question. You know your population really well, but most people don't see as many children with sickle cell as you do. So, what do families and young people want from a paediatrician? What can we offer them in terms of best quality care?
Subarna: I guess every paediatrician in the UK now will at least have one or two sickle patients in their clinic, just given how, widespread, people live everywhere in the country, so I think it's really important that, you know, paediatricians have the understanding of this condition. And also, I guess that relationship that develops between a child with a chronic illness and their family and the doctor and the specialist nurse or the multidisciplinary team that supports this chronic illness. So be it type one diabetes, be it any other chronic illness, and sickle cell is no different. And I think what families want is that kind of ongoing relationship, the relationship of trust, the relationship of kind of mutual understanding, learning from each other and supporting the family, and when done well, I think patients and families really value that.
Emma: I think that's really good advice. So even if you only have a few children that you look after with sickle cell, do your homework. Know a bit about it. And obviously we often say, just get in touch with somebody, somebody who sees a lot.
Secondly, any child with a chronic illness, it's about that relationship with the team, that MDT team relationship. So, listen to them, listen carefully, respond to what they want, and grow that relationship, because that's what matters to parents and families, that they have a trusted person that they can always turn to. Really good information. I think it's really easy to forget it's a lifelong illness.
Subarna, I think this brings up a really interesting point. You're in London, and you look after a really big population of children and families with sickle cell, but up here in Newcastle on Tyne, we see very few, but there's a really good system of hub and spoke. So, do you want to talk a little bit about network?
Subarna: Yes, so for the last five years or so, there has been a real restructuring in England of the way sickle cell care is developed through managed clinical networks. And the whole of England has been divided into 10 networks for sickle cell and they are called Hemoglobinopathy Coordinating Centres (HCCs) and essentially there is a hub of kind of governance, guideline, provision and clinical MDTs that happen centrally in these networks, in these HCCs. And every hospital within a defined geographic area within that network will have direct access to those MDTs. So it is now very well established that if you are a single handed paediatrician in a very low prevalence area where there is barely any sickle patients, and you come across a really complex patient, or you come across any problem with it, there are very clear lines of contact that you can make and find advice very readily.
Emma: Fabulous, it's always best to ask the expert, and then having people like you so accessible really makes a huge difference. I think that's a really important point. Just ask for help. Don't do things by yourself.
That's brilliant. So, we've talked about how the networks operate, so let's just have a little chat about the actual management of sickle cell disease. So, we've talked a bit about the acute management of painful crises. But as we've discussed, this is a long-term condition. So, what kind of options are there for children and families with sickle cell?
Subarna: Yes, so although we've been working on new drugs for a long time, one drug that we've understood and learned about a lot is hydroxycarbamide, and it's been around in the sickle cell space for over 40 years. But in the last five years or so, we have had evidence that has really changed the way we do paediatric management of sickle cell disease using hydroxycarbamide. So, one thing that is now very well embedded in clinical practice, based on a lot of good research, is offering hydroxycarbamide to patients very young, nine months onwards, and even asymptomatic children with sickle cell anaemia. So, this is haemoglobin SS, and haemoglobin S because Cirrus thalassemia. So, if you've got a patient with SS or SB to zero thalassemia, and they're over the age of between nine months to 12 months, there has to be a very good reason why they should not be on hydroxycarbamide. So that should be the norm. Just like penicillin is the norm, hydroxycarbamide beyond the age of nine to 12 months really should be the norm. And these are the kind of conversations that should take place at the first consultation that you ever see with that patient, you know, the three-month-old baby that's come through the screening program. You've seen them to start penicillin, you mention hydroxycarbonate.
Emma: That's so important, because I think this idea that prevention is always better than treatment, thinking about putting things in place before you hit crises and symptoms. So really, really interesting that is much younger than we've been used to. And just because this is my pet favourite topic, do you teach them all to swallow pills really early as well?
Subarna: It's a very good question. Yes, we have been doing that. We were very lucky now that we've got a syrup which is very palatable. Only five years ago, it used to smell like urine because it was compounded in the pharmacy, hydroxyurea and but now there is a palatable syrup, but it's very expensive. So, we do have pill schools. Our pharmacy where I work has a pill school, and it is really encouraging patients to start taking pills. And I think we've got a lot of uptake on that, I highly recommend that actually.
Emma: Yeah, as we promote KidzMed and pill swallowing a lot in Newcastle, and we actually routinely would suggest that children from the age of four, so anybody four and over swallow pills.
Subarna: Parents like that as well, particularly when they're traveling, it's much easier to carry pills than to carry bottles.
Emma: Cheaper, safer, easier to dose, less trips to go and get special medicines, because you can often only get the formulations from big centres. So, that's really, really interesting, that you are using these drugs at a lower age. What other new options for treatment can be offered for these families?
Subarna: One thing that has recently been approved in the NHS, and in fact, NHS was one of the first to approve this is gene therapy, and this is now available for children with sickle cell disease from the age of 12 and upwards. And this has been phenomenal, in the sense that for children who need cure from sickle cell disease but do not have a suitable donor, now have hope of cure.
Emma: So I think that's really important, that one of the options is a hematopoietic stem cell transplant, and that's actually been something that has happened for many years. How many of your children from your clinic get transplants now?
Subarna: Not that many, I have to say. So, we look after about 500 children at any given time with sickle cell disease, and annually, we probably send about three or four children for transplants, and these are children who generally tend to have very severe, chronic and progressive cerebrovascular disease. I think increasing use of hydroxycarbamide has made a big difference. What has happened is that they are not so ill during childhood, but we kind of have pushed it across to the adult age. And so quite a lot of the adult patients, young adults, are now getting more symptomatic with chronic pain or acute pain not responsive to hydroxycarbamide, and they are often needing transplant when they become adults.
Emma: Interesting, so we've gone through these different treatment options, early hydroxycarbamide, stem cell transplant for the most serious cases, which is now happening more in young adults, and for those who don't have a donor, gene therapy, which potentially, in the future, could be really good, because potentially you might have less side effects, and that might be simpler to give
Subarna: Absolutely, right now, what happens is an ex-vivo procedure. So, you have to take the stem cells out of the patient, give the patient myeloablative chemotherapy, and return the gene edited stem cells back to the patient. But in the future, it might all be in vivo, and I can imagine a time when you might need the odd injection from time to time, and your sickle cell is killed.
Emma: That is incredible, so exciting. Really, really interesting conversations that you're going to have with your patients in the future. So, we've talked about acute crisis, we've talked about different managements, we've talked about what patients want. Is there anything else you'd like to touch on?
Subarna: Yes, there is one thing that I think trainees might benefit from going back and looking up, is the No One's Listening report, which I think it's been a landmark report, I must say, in the sickle cell sphere in in the UK. So, this was published by an all-party parliamentary group for sickle cell and Thalassemia about four years ago now, so November 2021 and it basically the topic is no one's listening, that's what the report says. And this exactly means that it came out of avoidable couple of avoidable deaths amongst young adults with sickle cell. And it is basically, not only just telling how the state of affairs is, which was terrible four years ago, but also some really helpful advice on how to improve services. And I think it's worth giving that report a read, because it gives you very good ideas on how you can improve, with very minimal financial input, how you can improve care for your patients. And that requires empathy, consideration, listening, learning, humility, all of that, and that has actually triggered quite a lot of improvement initiatives by the government. And that is very welcome.
Emma: Absolutely. It sounds like something that everybody should read, the No One's Listening report from November 2021 which is actually driven by patients, and a roadmap on how you can improve your own services. Listening to you, it feels like all diseases need to read this report, not just people with sickle cell!
Subarna, it's been such a pleasure to talk to you. I feel like I've done all my homework now you've told me all the things that I really needed to do to improve my knowledge, to think about how I could improve the services locally, and just to think about what's best for patients and families. Before we go, we give everybody, it's a bit like Desert Island Discs! We give you the chance to give us three top tips. So, what would your three top tips be to all those paediatricians, clinicians, healthcare practitioners who are going to listen to this podcast be?
Subarna: So, one thing I would always say is, if you are lucky enough to train or work in a centre, or have access to a centre where there is a sickle cell clinic, go and sit in a clinic on your study education day, because seeing patients when they are in pain is very different from seeing patients when they are well. And you can then see the human side of them and that you will realise that these are just ordinary kids with aspirations like any other. And I think it's very important that you do that, and this is specifically for trainees. That is a top tip.
The second is, I guess, understanding, and this is more just to do with sickle cell, understanding that sickle cell is, to a certain extent, it's a hypostatic condition, so children are vulnerable to infections and so on. So, bearing that in mind.
And the third thing is that there is that inequity in care, without a doubt. You know, we know that there is lack of investment in research, there's lack of investment in care and having that awareness, and particularly with a group of patients who are already very societally sort of underprivileged. So, have that kind of understanding and empathy about the condition. It's very difficult to say people to change culture, but you know, just to understand that people can come from different circumstances, and they may not be similar to the ones that you're used to. Am I being preachy?
Emma: No, not at all. I love that. So, I think your three top tips are so important. I mean, go to clinic, absolutely. Go to clinic, see what children and families lives are like. Remember that children with sickle cell are a really vulnerable population. They're vulnerable to pain, they're vulnerable to infection, and most importantly, they're vulnerable because there is an inequity of care. There's a lack of investment. These are often children from marginalised groups. They're from different ethnic backgrounds. Maybe English isn't their first language. You need to be a sickle cell champion for these children. They need people to stand up and shout out and look after them, and I guess I'm just saying that's their job, isn't it?
Subarna: Absolutely.
This podcast is produced by Odland Education. The views, thoughts and opinions expressed in this podcast relate solely to the speaker and not necessarily to their employer, organisation, the Royal College of Paediatrics and Child Health, or any other groups or individual. You can find a wealth of information on the important work of the Royal College of Paediatrics and Child Health on rcpch.ac.uk, or #choosepaediatrics.
-
Episode 16: Food insecurity
What would you do if you saw a child at school stuffing toast into his backpack so his baby sister could eat, because there was no food at home? With four and a half million children in the UK living in poverty, food insecurity is a growing and deeply concerning issue. It has a profound impact on the health and wellbeing of children and young people.
This week Emma and the panel are joined by Professor Greta Defeyter to go over the effects of food insecurity on child development, the details of food deserts and food swamps, and the practical steps we can take.
Professor Greta Defeyter OBE is a Professor of Developmental Psychology at the Northumbria University and the founder and director of the Healthy Living Lab.
[Music starts]
Greta: When you look at the eating habits of those people who are food insecure, they're not healthy. They can't be healthy because of the cost of food.
Emma: I don't think people realise that obesity is a disease of poverty.
Greta: And I saw a little boy putting toast into his pockets and into his backpack.
[music ends]
Emma: Welcome Greta Defeyter. I'm really excited to welcome you to The Paeds Round podcast, and it's really, really, exciting to have different people to talk to us. And I believe your work is so important that all paediatricians should know about what you do.
Greta: Well, thank you so much. I'd love to speak to paediatricians. So, thank you for this opportunity to speak to you today, Emma.
Emma: I think that many people in paediatrics, but not in the wider world, may not know who you are and what you do. So, you're a Professor of Developmental Psychology in The Department of Social Work and Education and Community Wellbeing in Northumbria University, and the founder and Director of the Healthy Living Lab. And you've been awarded all sorts of exciting medals. You're a food hero. You are a Fellow of the British Psychological Society, and I think you've just won an OBE - is that correct?
Greta: Yes, that's correct.
Emma: Tell me how did you get interested in what you're doing now? How did it all happen?
Greta: Okay, so it's a kind of strange story, in a way, because I was in the Department of Psychology at the time, and I had a PhD student looking at the effects of breakfast cereal on children's cognition. And these are very controlled experiments where we go into schools or we used to bring children into the lab, and we'd weigh out all of the food, we'd look at all the ingredients in the food, and then we'd measure children's cognition on a variety of different cognitive tests. And one day, she was conducting this research in a school, and I just happened to see a school breakfast club operating in the corner of the school hall. This was now nearly 22 years ago, so quite some time ago, where not many people knew about school breakfast clubs, and I definitely didn't know about them. And I asked the head teacher, what's going on over there. She just looked at me like I was really stupid, and said, it's a school breakfast club Greta. And I said, ‘well, why are you doing that?’ And she said, ‘well, some of our children live in poverty, and they come in to school, and they haven't had breakfast’, I said, ‘could I go across and have a look?’ Typical psychologist and a woman very nosy.
So, we went across and had a look, and I saw a little boy putting toast into his pockets and into his backpack. And I thought, that's strange behaviour. So, I asked the head teacher, obviously, for child safeguarding whether I could go and talk to the young pupil and she came across with me. I said, ‘you're not in any trouble, but can you just tell me why you're putting toast in your backpack?’ And quite matter of fact, in a matter of fact, he said to me, ‘I'm taking toast home for my baby sister, as there's no food in the house’, and it was the way he said it as a practical solution that his child had thought of to address what we now call household foods insecurity.
It's spoken about quite widely, but that was the first time I'd ever come across it. And the image of that little boy putting that toast in his backpack has stayed with me right to this day and that just overnight, I changed my whole kind of, like, course of my research, so to speak, to say, this is out there. I can see it. I've just seen it. I've seen it right. So, I started to look at what research has been done with children and young people in the UK about food insecurity, and found there was very little.
Emma: Greta, that's an amazing story, and it's such a stark reminder of what life is like for many children and young people these days. So, tell me about food insecurity and how it affects children and young people.
Greta: In the UK, we currently have about four and a half million children living in poverty. Poverty is associated with food insecurity. So, food insecurity can be through lack of access to food. So it could be, for example, for elderly people in particular, they can't get to shops, and they haven’t got access to food in their communities, but that's a small proportion of those families that we classify as being food insecure. The majority of families who are food insecure is because they live in poverty.
When you look at the eating habits of those people who are food insecure, they're not healthy. They can't be healthy because of the cost of food. So, you find that families have what we call food insecurity with hunger. And I don't mean just mean feeling a little bit peckish, I mean, feeling hungry and there's no food to eat. It's a very different understanding of it. And we also have families who are classified as low to moderate food insecurity. What you typically find in those families is that they either downgrade in terms of the quality of the product of food they are buying, the value ranges, or typically, they have diets that are high in salt, sugar, saturated fat, and often it is classified now as ultra process food.
Emma: That is shocking, shocking statistics, when you look at the millions of children and young people living in poverty today in the UK, because we are a developed world country and we have the resources, that is actually a terrible statistic. What I want to ask you is, you've described how many children don't have food at all, so they're hungry and they can't get any food, or if they can get food, the quality of the food that is available to them is poor. And as a paediatrician, access to healthy food and fruit and vegetables and milk and calcium is so important to wellbeing and growth. So, what difference does it make? What are the health outcomes for these children and young people who can't get the food they need?
Greta: The podcast won't be long enough for me to list negative outcomes, but for the first time in decades, we're seeing things such as rickets, stunted growth, dental caries, so linked to poor oral hygiene, but also to the sugar content and food. We're seeing obesity and malnutrition sit side by side. We're seeing poor mental health, and we know that actually the food you eat, in terms of being absorbed into your circulation through the blood brain barrier, the amount of glucose in the food. So, the sugar conversion in the food affects how your cognition works, so your decision making. It also affects how well the children do at school. Not enough food actually doesn't allow the neurotransmitters to work properly, and so you have deficits and working memory, sustained attention, etc. So, food and the quality of food is important for children's health and development, but it's also important for their mood, their mental health and wellbeing and their cognitive processing.
Emma: Yes, it's very stark, isn't it? And I think it's a really important point. There are two things I want to talk about. I think it's a really important point that you need a certain type of food with complex carbohydrates, with fibre, with vitamins, and there's more and more work on your microbiome showing you need a big variety, and these ultra processed, cheap foods are not supplying that. And I just want to highlight something you said about obesity and poverty, because I think there's a misconception that people who are obese are eating too much. I don't think people realise that obesity is a disease of poverty.
Greta: Correct, and it's purely the fact that people don't have enough household income to buy a healthy diet. Poverty is also related not just to what you can purchase, but to where you live. So, if you live in poverty, you're more likely to live in poor housing. If you live in poverty, you're more likely to live in an area that actually doesn't have access to healthy food. I mean, I can share with everybody. I live in Blythe in Northumberland. I live in one of the poorest towns in Northumberland. We do not have a greengrocer. We don't have a bakers, we have lots of betting shops, we have lots of charity shops. I have a kind of a discount broken biscuit store. But in terms of accessing fresh produce, local produce, it's just not available in Blythe. That's it. That's a really good example.
So, poverty determines where you live, what you have access to, and therefore, obviously it also determines your financial income, to your household. And when you start loading these factors onto one another, you can see the ill effects of poverty, but you can see actually that poverty, I always think of poverty is like a prison with no bars, because poverty affects what you have in terms of your choice. People living in poverty don't have the same choice. So, it's not an individual behaviour. It's a structural problem that we have with our society.
Emma: I think that is so true. It's really interesting. I went to Detroit, and the whole town had collapsed with the collapse of the automobile industry. And they actually had food deserts, so you couldn't get hold of any food, and the only place that you could get food was at the petrol stations, because the only thing that was available was petrol. So, if you could walk to a petrol station, you could get food, there was nothing else in between.
Greta: Yeah, and we have the same in the UK. We have what we call food deserts and food swamps, as I call them. So, food deserts is where you can't access food. Food swamps, and we've all seen it, right! It's where you have on a line Kentucky Fried Chicken, McDonald's, Burger King, Wendy's, all of them, right! And they're cheap and they're easy. If you don't have a car, and you can't get access, you can see exactly what happens. And that then becomes normative, because everybody's doing it in that community. And so, it's again, I'll say it's a structural issue that we have. And sometimes I look at what I call big food operating across areas where there is really deep poverty, and I kind of just have to sometimes shake myself to say, keep fighting the fight. Because we have to fight this. We cannot allow this to happen. It's been happening for years, and it's just not good. It's costing our health service. It's costing our education service, and more importantly, it's costing the life of children and young people.
Emma: And I think it's really important that people understand this is not a quick solution. You can't give people vegetables because, actually, they may not have a stove. They may not be able to pay the electricity bill for them to actually cook the vegetables. They may not have, not only the implements, like all the things that you need, pots and pans, but the knowledge about what to do with the vegetables, because they have lost out on their education, and they are literally just living day by day, just getting by. So, this is a complex problem. This is not a simple problem.
Greta: Correct? And I'm going to add a further thought to that, that even if you have the knowledge, even if you have access to a cooker, if you are in house of multiple occupancy, for example, even if you can afford the electricity, when you have to make food choices, when you are living in poverty and you have high food insecurity, every decision you make is riskier.
So, if, for example, you cook, I can think of my own household if I cook jacket sweet potatoes instead of a normal potato. And my family tried them and they don't like them. You know what? I can go and cook something else, when you're looking at it in the terms of the risk of trying to do that sweet potato, the risk is tenfold when you live in poverty, to somebody like myself who can afford to cook something else. And it's an important thing, because poverty then changes the decision and risk making process, so that cognitive process of how much you take a risk. Okay? And that applies to food. It applies to gambling. It applies to whether you take a loan from a loan shop. Things that don't look rational for somebody that has money are completely rational when you live in poverty.
Emma: It is a really important thing that doctors and people in the medical profession who are looking after all these children with these effects of poor diet, which we know are huge, so obesity, diabetes, hypertension, malnutrition, and you're absolutely right. We've seen rickets. We've seen diseases of the Victorian age come back, which we have not seen in years. And it's really important that doctors understand the life that their patients lead.
Greta: Correct. So, I have examples where I've been working with children and young people, and they've been discharged from hospital, and they've been given a diet sheet. I mean, I have to laugh. I can absolutely appreciate what the clinician is trying to do. But I look at it, and I look at what I know the family can afford, there's a Red Sea. There's a there's an ocean between us, right! Because it's fine saying yes, you should eat according to the Eat Well Plate as one guide, for example, around food groups and nutritional standards. But the families I work with can't afford to eat an Eat Well Plate type of diet.
So, it then undermines, in a way, what the paediatrician, for example, is trying to do. And it also means that from the recipient point of view, that then starts to have a lack of trust, because it looks like the paediatrician doesn't understand the kind of home environment in which that child or young person live or you ask parents or carers to do something that maybe they can't do. Maybe they don't have access to a cooker. Maybe they have a refrigerator, but the food is stolen from the refrigerator. It's very difficult to try and match the two.
So, we have to think about how we reach out and how we work in a kind of, what I call a linking arms type of way to make people or support people, rather in having a better diet, but being really aware of the constraints on the situation in which young people live. Somebody will come out from hospital with a diet sheet, and the person that's taking care of that child or young person will say things like, we'll have a treat and we'll stop at McDonald's on the way home. There we go. And it's become a cultural treat, if not a normative everyday situation, and so we need to work with families to change that, but we need to work on the food system as well, and we need to work on the social welfare system, and we need to work on poverty. And all these levers have to work cross sectoral in terms of programmes, isn't it!
You can't just fix one programme. People's lives aren't like that. So, it is a complex problem, but it's something that both sides, having that greater understanding for both sides of the equation will go a long way to helping and supporting children and young people.
Emma: Yeah, I think it's really interesting what you say. t's so true about the McDonald's as a treat. What are treats? And I know from my children just going to the local state school, and they tell me that they actually don't like people looking in their packed lunch, because that makes them stand out. Their packed lunch doesn't have crisps; their packed lunch doesn't have biscuits. Their packed lunch has homemade food. One of my children doesn't like sandwiches, so I'll just take rice and lentils and things that are culturally appropriate for them. But that's very unusual. And children come to my house, and they sit down and they look on the table and they say, ‘what is that’? We were originally talking so we've talked about how food poverty and food insecurity leads to poor health. But what about the effect on your schoolwork? Because we are talking about children and young people here.
Greta: Yeah. So, we know when we look at studies that have looked at cognition and schoolwork, we know it is actually not just the fact of not having food, but the type of food you eat that affects your cognition. And the main processes that are affected are sustained attention and working memory. So, if you think about it in terms of schoolwork, well, you need to pay attention and you need to have a good working memory. So those processes are affected by default. Your educational attainment is going to be affected. And the government has been quite good and quite active in the last few months around school breakfast clubs. So, in England now we have a slow roll up, a good roll out of National School Breakfast clubs. And of course, we have the extension of free school meals to an additional 622,000 pupils come next September. So, both of those are really good programmes that the UK Government has introduced to try and combat both food insecurity, dietary intake and, also educational attainment.
Emma: Greta, what happens in the holidays because there's no school?
Greta: Well, so in the in the holidays and in days when children aren't in school, so children typically in state schools are in schools for about 190 days. But there are 173 days where children are not in school. So, you know, if you want to have an intervention, you have to think of the whole child, the whole system, the whole family. And so, I was very lucky that the All Party Parliamentary Group on school food gave me permission to conduct some research on their behalf. And we mapped the holiday clubs across England. We had over 400 organisations delivering but there was no governance, no quality assurance, and we spent the next five years collecting evidence about the impact of these clubs. And in 2017 Frank Field, actually presented a bill called the School Holidays, Food and Activities Bill to Parliament, and luckily the bill passed. It was a brand-new social policy, and after a few years, we got funding. And currently the government in England funds what they call the Holiday and Activities Food Programme, which I helped co design.
Emma: Tell me what the Holiday and activity Food Programme is?
Greta: The Holiday and Activity Food Programme is a programme that's funded by the Department for Education. It's funded at 200 million pounds a year, and it goes across every higher tier local authority in England. The programme itself is designed to offer free food and enriching activities for children aged 5 to 16 who are in receipt of free school meals.
Emma: I think that's so important. I would remember a friend of mine saying to me, I had 100% attendance at school because it's the only place I knew I would eat. I never missed a day of school. And as you said, like 173 days a year there is no school. So, this is a very, very basic need for people, and young people and children to have food. We've talked so much. There are so many things I could ask you, but I want to ask you something very specific. What is your ask to paediatricians when they see children and young people in their clinics or in their emergency departments, what do you want them to think about?
Greta: I suppose what I would ask them is try and put yourself in the shoes of your patients and think about them as people that may well live in a different environment or different household to your own. And the other thing I would ask them to do is to ensure that their hospital or their practice or their clinic has contacted the local authority and knows of the actual resources that are available. So whether you look at the HAP programme, whether you look at food pantries, whether you look at Citizens Advice numbers, whether you look at schools that are running breakfast clubs be aware of what's happening in your local vicinity, so that yourself or your social prescribers can actually direct and support families into those actual areas of help.
I think one of the things that's really difficult is keeping abreast of it for clinicians, but local authorities have that information, so the social prescriber has a really good link with the right person in the local authority. It's then quite easy to keep up to date with what's happening in your local area, and to think of some of the programmes, like the holiday activity programme, not as a deficit programme, but as an asset-based programme. And it doesn't have to be big things, even small things that we often take for granted, a trip to the park, for example, well, maybe it's buying a lollipop, or maybe it's taking a picnic. Well, if you don't have money and you don't have access to food, those things now become a problem, right! Or it may be something like going and playing football, but if you can't afford the football boots, then there's a problem. So, you're not engaging in the physical activity. So when you're thinking about food insecurity, remember that's just one part of that family's life, that life is affected by, especially if you're looking at poverty multiple factors so, damp housing, poor ventilation, can't afford the heating in the winter, clothes, school uniform, meals and the content in a packed lunch. I could go on and on, but hopefully you'll see it is complicated, but having that empathy, I think, and then setting realistic goals that that family can achieve, I think, is really important.
Emma: Yeah, I think the first thing I want people to do is just ask the question in a sympathetic manner. Very recently, I've been in clinic, and I was asked to see a baby who wasn't growing very well, and I said to the mother, you know, ‘what are you feeding?’ ‘What's happening?’ And she said, ‘at the end of the month, I can't afford formula milk. I can't afford milk for my baby’. It's just, if I hadn't asked the question, I could have gone down a whole route of investigation and taking bloods when I just needed to ask a simple question in a way that she felt safe to talk about this. As a result, there are the formula milk vouchers, and also the family might be eligible for warm home benefit and understanding, as you say, knowing that this is available, knowing that people can access it, you don't have to do it yourself. You just need to sign post them to the right place.
Greta: Yeah, and talking about it in a way that's normal, so you normalise it. Families trust paediatricians and school teachers much more than they trust academics so we're further down the list. Okay, but actually thinking about it in a normal way, if you're discharging a child or young person, or you're taking care of them, then actually, surely, you know, forgive me if I'm saying something out of term here, but surely you're taking care of the whole child, and a whole child isn't just in hospital. The whole child is going to go home to an environment there's no point in treating a child to me in hospital to send them home to, like a damp home or a home that's got mould coming down the wall or home that has got no food in the cupboards or the fridge, right! Because the child is just going to end right back with you again. So, it's thinking about how we as a whole society support what I call whole children, whole people.
Emma: Absolutely, there's no point in prescribing loads and loads of asthma inhalers when actually the root of the problem is poor housing.
Greta: Correct, and likewise there's no point in giving a diet sheet if the root of the problem is food insecurity,
Emma: Absolutely, and I think that, there's lots of ways that people can do small things. So, a good example is that we've started collecting for the children's clothes bank. I collect children's clothes that have been passed down from any of the staff in our hospital and secretaries, and every single time I tell people, if you don't give those clothes, children can't go to school, they can't go out of the house. There are people who don't have shoes. Tell me what we can do to make things better.
Greta: So, I think what we have to do is, as professionals, I think we have different roles to play at different levels. So, I think advocacy and campaigning around the issue, so that central government to look at policy. I think also locally, so thinking about how we work in the northeast, with our Northeast Mayor around interventions that she's putting in around her child poverty strategy. So, both the local and the national coming together, thinking about even small things. So, for example, how hospitals could play a role in - I'm going to say it, it's probably controversial, but I'm going to say it, it will be no surprise to Emma that I'm going to say it probably. But thinking about food served in hospitals, okay, thinking about, is that food really healthy!
Emma: I couldn't agree more. I think it's important. I think it's the one place where we can not only nourish children, but we can actually give parents and families the opportunity to see what they could have. But I'm actually quite ashamed of what happens in hospitals. We have done a whole lot of work, which I know you're aware of, where we don't actually, we haven't been feeding parents who come to hospital. And we have stories where we ask the parents, what do you do? And the parents said, I wait till my child was finished, and then I eat the scraps off their plate so they can't afford to eat. Generally, the cost of coming to hospital, and the pressure that then puts on the family for unnecessary admissions is huge. So, I think it's a really important thing to think about. You know, does this child need to be here? Do they need to be admitted? Is this the best place for them? Could you deliver this care closer to home? So, you've talked about what you want paediatricians to know, how you want paediatricians to ask questions, how you want paediatricians to understand where their patients come from, but we haven't really talked about what you'd like hospitals, management and even universities and academics to do on this. I'm sure you have an opinion, Greta, because you always do.
Greta: I do have an opinion on this. Okay, so, and I'm going to give you my opinion for what it's worth, I think that we really need to review the quality of food in hospitals and universities. So, I'm going to talk about universities, but what I'm going to say, I think, will apply to hospitals. So, when I look at schools or holiday activities and food that are - what we call school food standards - that actually govern the quality, and the food groups served to children and young people. Now we know from the science that brain development occurs all the way to age 21 right! So, this is now university students are included in my zone of development. When I look at the guidance for the food served in universities, you may be surprised. It's a completely blank page. There is no policy or guidance whatsoever. Emma: None. Greta: None. When I look at hospitals, if there is guidance, they are probably breaching it. I was at a local hospital to me not long ago, and the offer at the cafeteria was chips, or double cooked chips, or a bag of crisps or a sandwich that had so many ingredients in whose name I couldn't actually pronounce, and yet, these are places of learning and health and wellbeing, in terms of getting as well,
Emma: Right! Well, there's two bits of that, the hospitals, I absolutely agree, and I think it's really interesting, because I think that we can learn from other places that do it well. So I worked as a VSO (Voluntary Service Overseas) volunteer in the South Pacific, and I was a paediatrician in a hospital in Vanuatu, and what we did is, we had a hospital garden, and anybody who was staying more than a couple of days, they would go in their spare time, because there's a lot of time when you're sitting around in a hospital where things aren't happening and the garden was right below the wall, they would go to the garden, and they would help tend the garden, and they would pick the vegetables and food in the garden, and they would cook it all together for all the children and families on the ward. And it was such a good thing. It was such a sustainable thing, and it was fun, and it was an opportunity for the nurses and the children and the staff to do something together that wasn't just about immediate, I don't know, nasty things like giving injections and taking blood. So, it was a really positive thing. And I think something like that, we should be having things like that. So, there you go. That's what I think we should have.
Greta: So, I agree with that, but I think we should go further than that as well.
Emma: All right, Greta, it's been a huge pleasure. It's a bit like Desert Island Discs. You don't have 10 choices of discs, but you do get to give us your three top tips. So, we like to end on your three top tips. What would you like to say to all the paediatricians, all the healthcare workers who are looking after children and young people?
Greta: First thing I'd like to say is, thank you for all your hard work and professionalism. You saw us through Covid. You're still doing a grand job. You have my full support. That's the first thing I'd like to say. Second thing I'd like to say is, be aware of the whole child and young person, not just when they're in clinic or in your hospital but thinking about the environment that that child is going back to. And thirdly, is, have the conversation.
Emma: There we go, just like we are. It's been a great pleasure. Greta, it's just been so fun to talk to you, and you're right. We could have done this for a couple of hours, so we've just had to cut ourselves short.
[music starts]
This podcast is produced by Odland Education. The views, thoughts and opinions expressed in this podcast relate solely to the speaker and not necessarily to their employer, organisation, the Royal College of Paediatrics and Child Health, or any other groups or individual. You can find a wealth of information on the important work of the Royal College of Paediatrics and Child Health on rcpch.ac.uk, or #choosepaediatrics.
[music ends]
Further resources
-
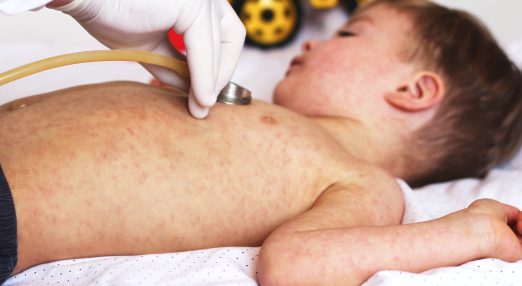
RCPCH Webinar: Measles – an update
In this topical webinar, Dr Elizabeth Whittaker, Professor Shamez Ladhani and Nalini Iyanger will provide an essential update on measles in children, ahead of an outbreak.

Resource Highlights: Measles
Have a few minutes to spare? Learn five top tips relating to measles | Contributor: Dr Liz Whittaker Senior Clinical Lecturer, Consultant Paediatrician. | Our collection of resource highlights give you concise, evidence-based insight into a health topic. They are a gateway to further learning with links to relevant educational activities on RCPCH Learning

RCPCH Webinar: Upskilling child health professionals to talk about air pollution
In this webinar, we join the RCPCH’s Clean Air Fund Partnership team to explore the barriers to talking to children, young people and their families about air pollution, and to learn how clinicians can overcome them.

RCPCH Webinar: Moving Towards Clean Air: Tackling Transport, Pollution, and Health Inequality
In this webinar, we explore transport, health, wellbeing, and air pollution. Transport is a key lever in both reducing air pollution and enhancing public wellbeing. We highlight case studies from the West Midlands Combined Authority and Living Streets, demonstrating initiatives that can be implemented locally to promote clean air and improve public health.

[ARCHIVED] RCPCH Webinar: Respiratory syncytial virus (RSV) – an update
In this webinar, Dr Elizabeth Whittaker, Dr Alison Kent and Dr Conall Watson will provide an update on respiratory syncytial virus (RSV), discussing the epidemiology of RSV, the maternal vaccination programme and what to expect this winter.
RCPCH webinar: Introduction to paediatric antimicrobial stewardship – How the rational use of antibiotics can improve the overall quality of paediatric care
In this webinar, Dr Sanjay Patel highlights the risk that antimicrobial resistance (AMR) poses to nenonates and children and speaks about the role of antimicrobial stewardship in addressing this growing problem.

Trainee Research Network Education Seminars (TREES) | Antimicrobial Stewardship in Paediatrics – Bridging Clinical Practice and Research (January 2025)
This session explores the global threat of antimicrobial resistance, the limits of current research, and how your antibiotic stewardship can help safeguard the future of healthcare.
Found an issue? Please get in touch with us:
Email us at rcpchlearning@rcpch.ac.uk



